Depending on your situation, you may be able to enroll in a Medicare Advantage plan during a Medicare SEP. You should note that Medicare Advantage plans require you to be enrolled in Part B. You may need to pay the Part B premium in addition to the Medicare Advantage plan premium, though some Medicare Advantage plans feature $0 premiums.
Full Answer
Do you have to pay Part B with Medicare Advantage?
You may need to pay the Part B premium in addition to the Medicare Advantage plan premium, though some Medicare Advantage plans feature $0 premiums. Can I switch from a Medicare Advantage plan to Part B?
What is a Medicare Advantage plan?
A Medicare Advantage is another way to get your Medicare Part A and Part B coverage. Medicare Advantage Plans, sometimes called "Part C" or "MA Plans," are offered by Medicare-approved private companies that must follow rules set by Medicare.
Do I still have Medicare if I join a Medicare Advantage plan?
If you join a Medicare Advantage Plan, you’ll still have Medicare but you’ll get most of your Part A and Part B coverage from your Medicare Advantage Plan, not Original Medicare.
When can I get Medicare Part B?
General Enrollment Period—If you have Part A coverage and you get Part B for the first time during this period (between January 1—March 31 each year), you can also join a Medicare Advantage Plan. Your coverage may not start until July 1.

Do I still pay Medicare Part B with a Medicare Advantage plan?
You continue to pay premiums for your Medicare Part B (medical insurance) benefits when you enroll in a Medicare Advantage plan (Medicare Part C). Medicare decides the Part B premium rate. The standard 2022 Part B premium is estimated to be $158.50, but it can be higher depending on your income.
Do you pay Part B if you have Advantage plan?
Many Medicare Advantage Plans have a $0 premium. If you enroll in a plan that does charge a premium, you pay this in addition to the Part B premium (and the Part A premium if you don't have premium-free Part A). Part B covers certain doctors' services, outpatient care, medical supplies, and preventive services.
Can you have Medicare and Medicare Advantage at the same time?
People with Medicare can get their health coverage through either Original Medicare or a Medicare Advantage Plan (also known as a Medicare private health plan or Part C).
Can I have an advantage plan and a supplemental plan?
You cannot have both at the same time. Medicare Advantage bundles Part A and B often with Part D and other types of coverage. Medicare Supplement is additional coverage you can buy if you have Original Medicare Part A and B.
How do I add Medicare Part B?
Contact Social Security to sign up for Part B:Fill out Form CMS-40B (Application for Enrollment in Medicare Part B). ... Call 1-800-772-1213. ... Contact your local Social Security office.If you or your spouse worked for a railroad, call the Railroad Retirement Board at 1-877-772-5772.
What is the biggest disadvantage of Medicare Advantage?
Medicare Advantage can become expensive if you're sick, due to uncovered copays. Additionally, a plan may offer only a limited network of doctors, which can interfere with a patient's choice. It's not easy to change to another plan. If you decide to switch to a Medigap policy, there often are lifetime penalties.
When can you add a Medicare Supplement to a client with a Medicare Advantage plan?
Can I combine Medicare Supplement with Medicare Advantage? If you already have Medicare Advantage plan, you can generally enroll in a Medicare Supplement insurance plan under one condition – your Medicare Advantage plan must end before your Medicare Supplement insurance plan goes into effect.
Can you go back and forth between Original Medicare and Medicare Advantage?
Yes, you can elect to switch to traditional Medicare from your Medicare Advantage plan during the Medicare Open Enrollment period, which runs from October 15 to December 7 each year. Your coverage under traditional Medicare will begin January 1 of the following year.
Does Medicare Advantage pay 100%?
All Medicare Supplement insurance plans generally pay 100% of your Part A coinsurance amount, including an additional 365 days after your Medicare benefits are used up.
Can you have two supplemental insurance plans?
Having two health insurance plans is perfectly legal, and many people have multiple health insurance policies under certain circumstances.
Can you have 2 Medicare Supplement plans?
Retirees can't have more than one Medicare supplement plan or one at the same time as a Medicare Advantage plan. To cut costs on health care, start by calculating whether a supplement or an Advantage plan will save you the most money.
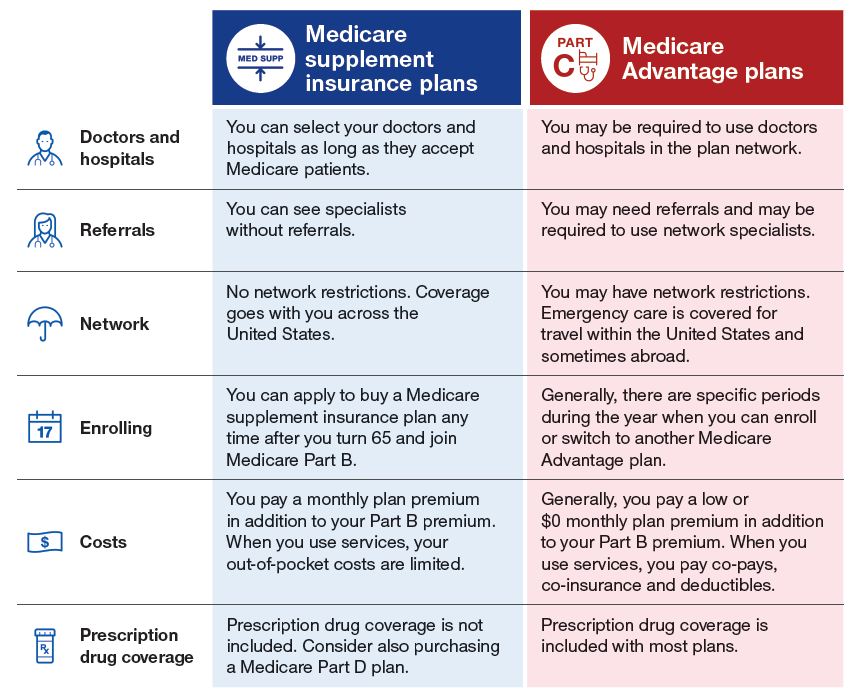
What is the difference between a Medicare Supplement plan and a Medicare Advantage plan?
Medicare Supplement plans. A Medicare Advantage plan (Medicare Part C) is structured to be an all-in-one option with low monthly premiums. Medicare Supplement plans offer additional coverage to Original Medicare with low to no out-of-pocket costs.
What is an HMO plan?
Health Maintenance Organization (HMO) plan is a type of Medicare Advantage Plan that generally provides health care coverage from doctors, other health care providers, or hospitals in the plan’s network (except emergency care, out-of-area urgent care, or out-of-area dialysis). A network is a group of doctors, hospitals, and medical facilities that contract with a plan to provide services. Most HMOs also require you to get a referral from your primary care doctor for specialist care, so that your care is coordinated.
What is a special needs plan?
Special Needs Plan (SNP) provides benefits and services to people with specific diseases, certain health care needs, or limited incomes. SNPs tailor their benefits, provider choices, and list of covered drugs (formularies) to best meet the specific needs of the groups they serve.
What happens if you get a health care provider out of network?
If you get health care outside the plan’s network, you may have to pay the full cost. It’s important that you follow the plan’s rules, like getting prior approval for a certain service when needed. In most cases, you need to choose a primary care doctor. Certain services, like yearly screening mammograms, don’t require a referral. If your doctor or other health care provider leaves the plan’s network, your plan will notify you. You may choose another doctor in the plan’s network. HMO Point-of-Service (HMOPOS) plans are HMO plans that may allow you to get some services out-of-network for a higher copayment or coinsurance. It’s important that you follow the plan’s rules, like getting prior approval for a certain service when needed.
Do providers have to follow the terms and conditions of a health insurance plan?
The provider must follow the plan’s terms and conditions for payment, and bill the plan for the services they provide for you. However, the provider can decide at every visit whether to accept the plan and agree to treat you.
Can a provider bill you for PFFS?
The provider shouldn’t provide services to you except in emergencies, and you’ll need to find another provider that will accept the PFFS plan .However, if the provider chooses to treat you, then they can only bill you for plan-allowed cost sharing. They must bill the plan for your covered services. You’re only required to pay the copayment or coinsurance the plan allows for the types of services you get at the time of the service. You may have to pay an additional amount (up to 15% more) if the plan allows providers to “balance bill” (when a provider bills you for the difference between the provider’s charge and the allowed amount).
What are the benefits of Medicare Part B?
3 things to know about Medicare Part B: 1 It is medical insurance that provides coverage for medically necessary services and preventative services. 2 You have to pay a monthly premium for it. The standard monthly premium is $148.50 in 2021, but you may pay more or less than that. 3 Coverage for medical services and supplies comes with deductibles, copayments, and coinsurance.
How much is Part B insurance in 2021?
Part B comes with a monthly premium. Many people pay the standard premium amount of $148.50 per month in 2021. You may pay higher or lower premiums than the standard premium based on how you pay your premium or your yearly income.
How much is the 2021 Medicare premium?
You have to pay a monthly premium for it. The standard monthly premium is $148.50 in 2021, but you may pay more or less than that.
What happens if you don't send your Medicare card back?
If you do not follow these instructions, you will be enrolled in Part B and must pay the Part B premiums.
Is Medicare Part B optional?
Medicare Part B provides medical insurance coverage. It covers many different services such as doctor visits and medical services. Part B is optional. If you are automatically enrolled in Medicare Parts A and B, you can opt out of Medicare Part B.
What is Medicare Advantage Plan?
Medicare Advantage Plan (Part C) A type of Medicare health plan offered by a private company that contracts with Medicare. Medicare Advantage Plans provide all of your Part A and Part B benefits, excluding hospice. Medicare Advantage Plans include: Health Maintenance Organizations. Preferred Provider Organizations.
How much does Medicare pay for Part B?
For Part B-covered services, you usually pay 20% of the Medicare-approved amount after you meet your deductible. This is called your coinsurance. You pay a premium (monthly payment) for Part B. If you choose to join a Medicare drug plan (Part D), you’ll pay that premium separately.
What happens if you don't get Medicare?
If you don't get Medicare drug coverage or Medigap when you're first eligible, you may have to pay more to get this coverage later. This could mean you’ll have a lifetime premium penalty for your Medicare drug coverage . Learn more about how Original Medicare works.
What is Medicare Supplement Insurance?
You can get a Medicare Supplement Insurance (Medigap) policy to help pay your remaining out-of-pocket costs (like your 20% coinsurance). Or, you can use coverage from a former employer or union, or Medicaid.
What are the extra benefits that Medicare doesn't cover?
Plans may offer some extra benefits that Original Medicare doesn’t cover—like vision, hearing, and dental services.
What is the original Medicare?
Original Medicare. Original Medicare is a fee-for-service health plan that has two parts: Part A (Hospital Insurance) and Part B (Medical Insurance). After you pay a deductible, Medicare pays its share of the Medicare-approved amount, and you pay your share (coinsurance and deductibles). (Part A and Part B) or a.
Does Medicare Advantage cover prescriptions?
Most Medicare Advantage Plans offer prescription drug coverage. . Some people need to get additional coverage , like Medicare drug coverage or Medicare Supplement Insurance (Medigap). Use this information to help you compare your coverage options and decide what coverage is right for you.
What is Medicare Advantage Plan?
A Medicare Advantage (Medicare Part C) plan is an alternative to Part A and Part B (though you still need to enroll in Part B before you can enroll in a Medicare Advantage plan). Your Medicare Advantage plan carrier (a private insurance company) provides all of your Part A and Part B benefits, instead of the federal government.
What is Medicare Supplement Insurance?
If you have Medicare Part A and Part B, you might also consider a Medicare Supplement Insurance (also called Medigap) plan. Medigap plans can help cover some of the out-of-pocket costs that Medicare does not cover, such as deductibles, coinsurance and copayments.
What happens if you don't have creditable coverage?
If you do not have “creditable coverage” after you first become eligible for Medicare Part B, you incur a penalty that you will pay when you eventually do enroll in Part B . The late enrollment penalty fee amount is a 10 percent increase in your Part B premium (which is $135.50 per month for most people in 2019) for each 12-month period you could ...
How much is the penalty for not enrolling in Part B?
For example, if you did not enroll in Part B when first eligible and delayed your enrollment for 14 months (and if no enrollment exception applied), your standard Part B premium amount – including your late enrollment penalty – would be $149.05 per month.
When is the open enrollment period for Medicare?
This enrollment period (also called the Open Enrollment Period for Medicare Advantage & Medicare prescription drug coverage) lasts from October 15 to December 7 every year.
Do retirees have to enroll in Medicare?
You may be automatically enrolled in Medicare Part A. Your retiree health plan (if you have one) may require you to enroll in Medicare. Whether or not this is the case, many health plans coordinate benefits with Medicare. Medicare is the usually the primary payer.
Is Medicare Part B optional?
Medicare Part B is optional. Whether or not you need Part B depends on your individual situation . You need to be aware that once you become eligible for Part B (generally when you turn 65), you will incur a late enrollment penalty for not signing up for Part B and decide you want it later, unless you meet one of the exceptions to ...
How much is Medicare Part B premium 2020?
The standard Medicare Part B premium for 2020 is $144.60. While most Medicare beneficiaries will pay the standard premium amount, the premium you will pay is dependent on your income. If your income falls below the federal standards, help is available for Medicare beneficiaries through Medicare Savings Programs (MSP).
What are the resources that can't be counted as assets in Medicare?
Each Medicare Savings Plan has a specific income and asset limit, resources that can’t be counted as assets include: Your primary house. One car. Household goods and wedding/ engagement rings. Burial spaces.
Is Medicare Part A free?
Medicare Part A, which covers hospitalization, is free for anyone eligible for Social Security, even if they have not claimed benefits yet. If enrolled in Part B but not yet collecting Social Security benefits, you’ll be billed quarterly by Medicare. As a Medicare beneficiary, you have many options when it comes to how you receive your Medicare ...
Does Medicare Part B deduct premiums?
If you sign up for both Social Security and Medicare Part B – the part of Original Medicare that covers medically necessary and preventative services, The Social Security Administration will automatically deduct the premium from your monthly benefit.
How does Medicare work with other insurance?
When there's more than one payer, "coordination of benefits" rules decide which one pays first. The "primary payer" pays what it owes on your bills first, and then sends the rest to the "secondary payer" (supplemental payer) ...
How long does it take for Medicare to pay a claim?
If the insurance company doesn't pay the claim promptly (usually within 120 days), your doctor or other provider may bill Medicare. Medicare may make a conditional payment to pay the bill, and then later recover any payments the primary payer should have made. If Medicare makes a. conditional payment.
What is a Medicare company?
The company that acts on behalf of Medicare to collect and manage information on other types of insurance or coverage that a person with Medicare may have, and determine whether the coverage pays before or after Medicare. This company also acts on behalf of Medicare to obtain repayment when Medicare makes a conditional payment, and the other payer is determined to be primary.
What is a group health plan?
If the. group health plan. In general, a health plan offered by an employer or employee organization that provides health coverage to employees and their families.
How many employees does a spouse have to have to be on Medicare?
Your spouse’s employer must have 20 or more employees, unless the employer has less than 20 employees, but is part of a multi-employer plan or multiple employer plan. If the group health plan didn’t pay all of your bill, the doctor or health care provider should send the bill to Medicare for secondary payment.
Which pays first, Medicare or group health insurance?
If you have group health plan coverage through an employer who has 20 or more employees, the group health plan pays first, and Medicare pays second.
What is the phone number for Medicare?
It may include the rules about who pays first. You can also call the Benefits Coordination & Recovery Center (BCRC) at 1-855-798-2627 (TTY: 1-855-797-2627).
