Generally speaking Medicare providers will submit a bill to Medicare using the program’s coding system which identifies every service that could be provided to a beneficiary. Medicare then sends payment back to the provider for the services provided.
What is a Medicare supplement plan?
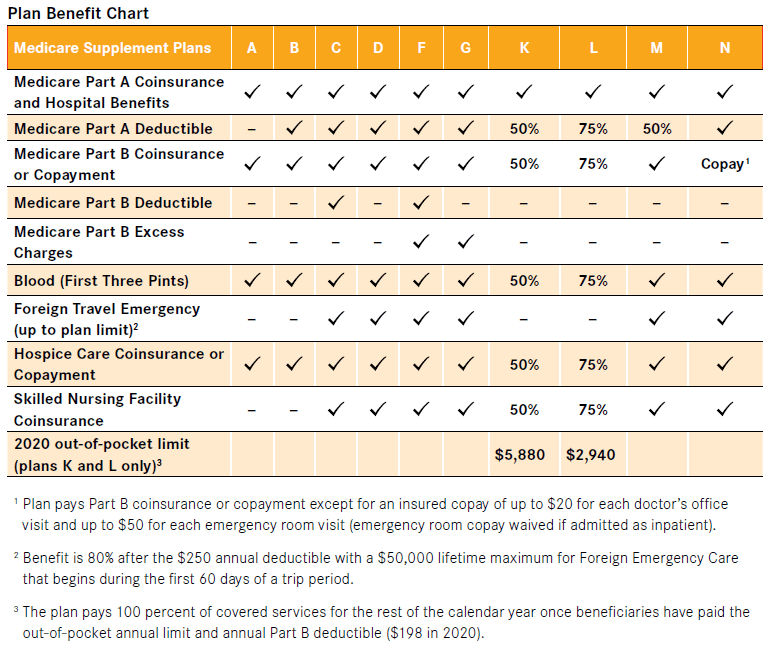
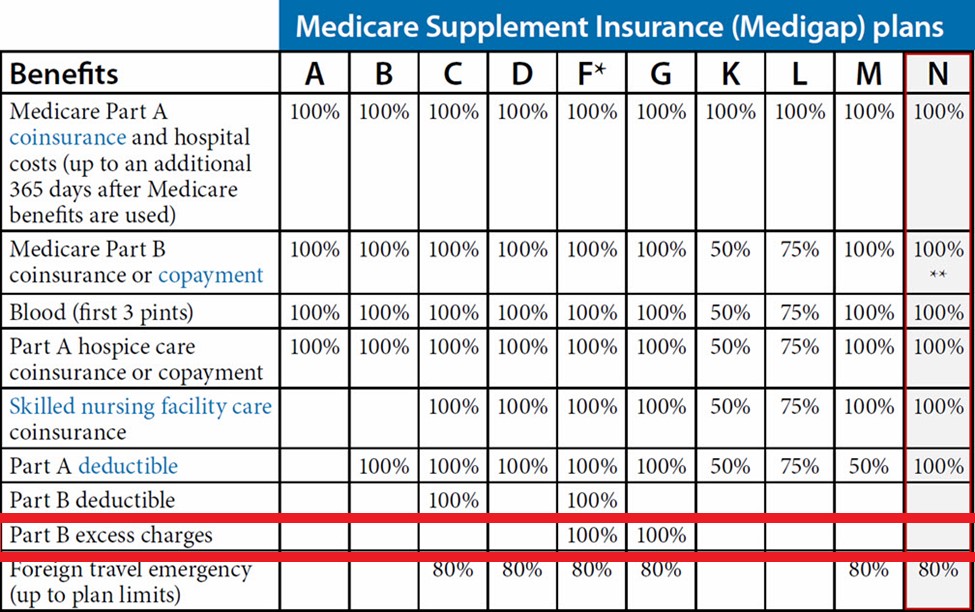
Medicare Supplement plans are standardized by the federal government and are identified as letters. Supplement insurance plans are sold by some private insurance providers in the United States. Not all companies have them, or sell all available plans, so you may have to look for one in your area.
What does a provider send a bill to Medicare?
The provider sends a bill to Medicare that identifies the services rendered to the patient. After a health care provider treats a Medicare patient, the provider sends a bill to Medicare that itemizes the services received by the beneficiary.
How does Medigap work with Medicare supplements?
If the member has a Medicare supplement attached, Medicare will forward the processed claim to the Medigap carrier to process accordingly (based on deductible, copays, and co-insurance for a given Medigap plan). The carrier will then look to Medicare to determine eligibility. This is a very important concept to understand.
Can You Bill a patient with a Medicare Advantage plan?
Don’t Confuse Medicare Advantage Plans with Medicare. If a patient has a Medicare Advantage plan, do not bill traditional Medicare. Medicare Advantage plans are not supplemental plans, and they must cover all traditional Medicare services, including Part A (hospital insurance) and Part B (medical insurance) coverage.

How does billing work with a Medicare Supplement?
Medigap pays for some of the bills left over by Medicare's coverage gaps – and it all happens automatically. Medicare and Medigap work together smoothly to pay for your medical bills. It's done automatically and usually without any input from you; that's how Medigap policies work.
How are Medicare and supplemental policies are billed?
When you have Medicare and other health insurance, such as a Medicare Supplement insurance plan, each type of coverage is called a “payer.” The primary payer will pay what it owes on your health-care bills first and then send the balance to the secondary payer. Coordination of benefit rules decide who pays first.
How are Medicare Supplement claims paid?
Medicare supplement and Medicare Cost plans: Your provider sends your claim to Medicare and your insurer. Medicare is primary payer and sends payment directly to the provider. The insurer is secondary payer and pays what they owe directly to the provider.
How do providers bill Medicare?
Payment for Medicare-covered services is based on the Medicare Physicians' Fee Schedule, not the amount a provider chooses to bill for the service. Participating providers receive 100 percent of the Medicare Allowed Amount directly from Medicare.
How is Medigap billed?
The periodic payment to Medicare, an insurance company, or a health care plan for health or prescription drug coverage. for your Medigap policy. You pay this monthly premium in addition to the monthly Part B premium that you pay to Medicare. A Medigap policy only covers one person.
Does CMS regulate Medicare Supplement plans?
The California Department of Insurance (CDI) regulates Medicare Supplement policies underwritten by licensed insurance companies.
Who files Medicare supplement claims?
Your Medicare Part A and B claims are submitted directly to Medicare by your providers (doctors, hospitals, labs, suppliers, etc.). Medicare takes approximately 30 days to process each claim.
Who pays claims with a Medicare Advantage plan?
If you have Original Medicare, the government pays for Medicare benefits when you get them. Medicare Advantage Plans, sometimes called “Part C” or “MA Plans,” are offered by private companies approved by Medicare. Medicare pays these companies to cover your Medicare benefits.
What is the difference between a Medicare supplement and an Advantage plan?
Medicare Advantage and Medicare Supplement are different types of Medicare coverage. You cannot have both at the same time. Medicare Advantage bundles Part A and B often with Part D and other types of coverage. Medicare Supplement is additional coverage you can buy if you have Original Medicare Part A and B.
How do I bill Medicare secondary claims electronically?
Medicare Secondary Payer (MSP) claims can be submitted electronically to Novitas Solutions via your billing service/clearinghouse, directly through a Secure File Transfer Protocol (SFTP) connection, or via Novitasphere portal's batch claim submission.
Can I bill Medicare for non covered services?
Under Medicare rules, it may be possible for a physician to bill the patient for services that Medicare does not cover. If a patient requests a service that Medicare does not consider medically reasonable and necessary, the payer's website should be checked for coverage information on the service.
Can a provider charge less than Medicare?
Here's my answer: Yes, you can charge self-pay patients less than Medicare, but you want to make it clear that this lower charge is not your “usual and customary fee” (lest Medicare decides to pay you that much, too).
What happens if a provider does not accept Medicare?
Keep in mind that if a provider does not participate in Medicare's network or accepts assignment, a claims form may need to be submitted. If you paid up front, Medicare typically would reimburse you accordingly. A non-assignment provider might request the excess amount up front (up to 15% higher than what Medicare allows). These providers may file a claim on your behalf to Medicare in these situations. Ideally, use providers that accept assignment as the claims processing is extremely streamlined and your out-of-pocket expenses should be much lower depending on the Medigap plan that you have. Some Medicare supplement plans such as the F plan, cover excess and this is a big reason to consider the F plan.
How does accepting assignment affect Medicare?
First, it affects the rates that the provider will charge for a given diagnostic code since accepting assignment also means accepting Medicare's schedule of reimbursements ( or up to 15% higher if a provider chooses). The other big impact is on the claims side.
What does it mean when a provider accepts an assignment?
The term for this is that a provider accepts "assignment" which essentially means that the provider is in Medicare's network. This has two major impacts.
Does Medicare supplement work with Medigap?
First, it's important to understand how Medicare itself deals with providers and secondly, how Medigap supplements coordinate with Medicare itself. The first point depends on the status of the particular provider (doctor or hospital) in question. If the provider participates with Medicare, the claims process can be pretty smooth and coordinated.
Is Medicare a scary thing?
It's scary enough to go through a major health scare but the billing and claims side can be downright terrifying even if you have Medicare and a Medicare supplement. There can be many pages of detail with codes and descriptions that are foreign to most of us. Let's take a look at how Medicare supplement claims are processed in conjunction with Medicare itself so that we go into the paperwork tornado with a safety rope.
Does Medicare Supplement Plan pay for a procedure?
We have to be careful here. For a given medical procedure, if Medicare deems that it is not covered, the Medicare supplement plan will also not pay. The supplement looks to Medicare to determine what is eligible and then pays accordingly.
Does Medicare pay part of a covered benefit?
Medicare will pay part of a covered benefit and the supplement will pay all or part of the remaining claim. You will then get an Explanation of Benefits or an EOB showing what the total amount was, what Medicare and supplement paid, and your responsibility if any for that particular claim.
What is Medicare Supplement?
Medicare supplement insurance policies help fill in the gaps left by Original Medicare health care insurance. For many people, Medicare Supplement, also known as Medigap, insurance helps them economically by paying some of the out-of-pocket costs associated with Original Medicare.
What percentage of Medicare supplement is paid?
After this is paid, your supplement policy pays your portion of the remaining cost. This is generally 20 percent. Some policies pay your deductibles The deductible is a set amount which you must pay before Medicare begins covering your health care costs.
How many people does Medicare Supplement cover?
Keep in mind that, just like Medicare, Medicare Supplement plans are individual insurance policies. They only cover one person per plan. If you want coverage for your spouse, you must purchase a separate plan.
How long does it take to get a Medigap plan?
When you turn 65 and enroll in Part B, you will have a 6-month Initial Enrollment Period to purchase any Medigap plan sold in your state. During this time, you have a “guaranteed issue right” to buy any plan available. They are required to accept you and cannot charge you more due to any pre-existing conditions.
How long does Medicare cover travel?
Each plan varies in what it covers, but all plans pay for Medicare Part A (hospital insurance) coinsurances for up to 365 days beyond the coverage that Medicare offers. Some of the plans cover a percentage of the cost for emergency health care while traveling abroad.
How old do you have to be to qualify for medicare?
To be eligible for Medicare, you must be at least 65 years old, a citizen of the United States or permanent legal resident for at least five consecutive years. Also, you, or your spouse, must have worked and paid federal taxes for at least ten years (or 40 quarters).
Does Medicare cover long term care?
Most plans do not cover long-term care, vision, dental, hearing care, or private nursing care. All Medicare Supplement insurance coverage comes with a monthly premium which you pay directly to your provider. How much you pay depends on which plan you have.
What is Medicare Advantage?
Medicaid. A joint federal and state program that helps with medical costs for some people with limited income and resources.
What is the difference between Medicare and Original Medicare?
Original Medicare. Original Medicare is a fee-for-service health plan that has two parts: Part A (Hospital Insurance) and Part B (Medical Insurance). After you pay a deductible, Medicare pays its share of the Medicare-approved amount, and you pay your share (coinsurance and deductibles). and is sold by private companies.
What is a Medigap policy?
Those plans are ways to get Medicare benefits, while a Medigap policy only supplements your Original Medicare benefits. The periodic payment to Medicare, an insurance company, or a health care plan for health or prescription drug coverage.
What happens if you buy a Medigap policy?
If you have Original Medicare and you buy a Medigap policy, here's what happens: Medicare will pay its share of the. Medicare-Approved Amount. In Original Medicare, this is the amount a doctor or supplier that accepts assignment can be paid. It may be less than the actual amount a doctor or supplier charges.
How many people does a Medigap policy cover?
for your Medigap policy. You pay this monthly premium in addition to the monthly Part B premium that you pay to Medicare. A Medigap policy only covers one person. If you and your spouse both want Medigap coverage, you'll each have to buy separate policies.
Does Medicare cover prescription drugs?
Some Medigap policies sold in the past cover prescription drugs. But, Medigap policies sold after January 1, 2006 aren't allowed to include prescription drug coverage. If you want prescription drug coverage, you can join a Medicare Prescription Drug Plan (Part D). If you buy Medigap and a Medicare drug plan from the same company, you may need to make 2 separate premium payments. Contact the company to find out how to pay your premiums.
Does Medigap cover everything?
Medigap policies don't cover everything. Medigap policies generally don't cover. long-term care. Services that include medical and non-medical care provided to people who are unable to perform basic activities of daily living, like dressing or bathing.
How to determine primary payer for Medicare?
The CMS Questionnaire should be used to determine the primary payer of the beneficiary’s claims. This questionnaire consists of six parts and lists questions to ask Medicare beneficiaries. For institutional providers, ask these questions during each inpatient or outpatient admission, with the exception of policies regarding Hospital Reference Lab Services, Recurring Outpatient Services, and Medicare+Choice Organization members. (Further information regarding these policies can be found in Chapter 3 of the MSP Online Manual.) Use this questionnaire as a guide to help identify other payers that may be primary to Medicare. Beginning with Part 1, ask the patient each question in sequence. Comply with all instructions that follow an answer. If the instructions direct you to go to another part, have the patient answer, in sequence, each question under the new part. Note: There may be situations where more than one insurer is primary to Medicare (e.g., Black Lung Program and Group Health Plan). Be sure to identify all possible insurers.
When do hospitals report Medicare Part A retirement?
When a beneficiary cannot recall his/her retirement date, but knows it occurred prior to his/her Medicare entitlement dates, as shown on his/her Medicare card, hospitals report his/her Medicare Part A entitlement date as the date of retirement. If the beneficiary is a dependent under his/her spouse's group health insurance and the spouse retired prior to the beneficiary's Medicare Part A entitlement date, hospitals report the beneficiary's Medicare entitlement date as his/her retirement date. If the beneficiary worked beyond his/her Medicare Part A entitlement date, had coverage under a group health plan during that time, and cannot recall his/her precise date of retirement but the hospital determines it has been at least five years since the beneficiary retired, the hospital enters the retirement date as five years retrospective to the date of admission. (Example: Hospitals report the retirement date as January 4, 1998, if the date of admission is January 4, 2003)
What is secondary payer?
Medicare is the Secondary Payer when Beneficiaries are: 1 Treated for a work-related injury or illness. Medicare may pay conditionally for services received for a work-related illness or injury in cases where payment from the state workers’ compensation (WC) insurance is not expected within 120 days. This conditional payment is subject to recovery by Medicare after a WC settlement has been reached. If WC denies a claim or a portion of a claim, the claim can be filed with Medicare for consideration of payment. 2 Treated for an illness or injury caused by an accident, and liability and/or no-fault insurance will cover the medical expenses as the primary payer. 3 Covered under their own employer’s or a spouse’s employer’s group health plan (GHP). 4 Disabled with coverage under a large group health plan (LGHP). 5 Afflicted with permanent kidney failure (End-Stage Renal Disease) and are within the 30-month coordination period. See ESRD link in the Related Links section below for more information. Note: For more information on when Medicare is the Secondary Payer, click the Medicare Secondary Payer link in the Related Links section below.
Why did CMS develop an operational policy?
CMS developed an operational policy to help alleviate a major concern that hospitals have had regarding completion of the CMS Questionnaire.
Does Medicare pay for black lung?
Federal Black Lung Benefits - Medicare does not pay for services covered under the Federal Black Lung Program. However, if a Medicare-eligible patient has an illness or injury not related to black lung, the patient may submit a claim to Medicare. For further information, contact the Federal Black Lung Program at 1-800-638-7072.
Does Medicare pay for the same services as the VA?
Veteran’s Administration (VA) Benefits - Medicare does not pay for the same services covered by VA benefits.
Does no fault insurance cover medical expenses?
Treated for an illness or injury caused by an accident, and liability and/or no-fault insurance will cover the medical expenses as the primary payer.
How does Medicare work with other insurance?
When there's more than one payer, "coordination of benefits" rules decide which one pays first. The "primary payer" pays what it owes on your bills first, and then sends the rest to the "secondary payer" (supplemental payer) ...
When is Medicare paid first?
When you’re eligible for or entitled to Medicare because you have End-Stage Renal Disease (ESRD), during a coordination period of up to 30 months, the group health plan or retiree coverage pays first and Medicare pays second. You can have group health plan coverage or retiree coverage based on your employment or through a family member.
What is a Medicare company?
The company that acts on behalf of Medicare to collect and manage information on other types of insurance or coverage that a person with Medicare may have, and determine whether the coverage pays before or after Medicare. This company also acts on behalf of Medicare to obtain repayment when Medicare makes a conditional payment, and the other payer is determined to be primary.
How long does it take for Medicare to pay a claim?
If the insurance company doesn't pay the claim promptly (usually within 120 days), your doctor or other provider may bill Medicare. Medicare may make a conditional payment to pay the bill, and then later recover any payments the primary payer should have made. If Medicare makes a. conditional payment.
What is a group health plan?
If the. group health plan. In general, a health plan offered by an employer or employee organization that provides health coverage to employees and their families.
What is the difference between primary and secondary insurance?
The insurance that pays first (primary payer) pays up to the limits of its coverage. The one that pays second (secondary payer) only pays if there are costs the primary insurer didn't cover. The secondary payer (which may be Medicare) may not pay all the uncovered costs.
How many employees does a spouse have to have to be on Medicare?
Your spouse’s employer must have 20 or more employees, unless the employer has less than 20 employees, but is part of a multi-employer plan or multiple employer plan. If the group health plan didn’t pay all of your bill, the doctor or health care provider should send the bill to Medicare for secondary payment.
How does Medicare and Medigap work?
Medicare and Medigap work together smoothly to pay for your medical bills. It’s done automatically and usually without any input from you; that’s how Medigap policies work. That ease-of-use is a big appeal of owning a Medigap policy. Your doctors are in charge of your medical care. They know that Medicare’s rules require ...
What If You Have a Billing Issue?
In rare cases, if a bill does get lost in the system or is left unpaid, it’s possible for you to file a claim with Medicare yourself. To help you monitor that, every three months Medicare will mail you an Explanation of Benefits (EOB) that summarizes all the bills they approved and paid on your behalf. You can also create an online Medicare account and view your bills there.
Does Medicare cover gaps?
After that, Medicare uses a system called “crossover” to electronically notify your Medigap insurance company that they have to pay the part of the remainder (the gaps) that your Medigap policy covers. All you have to remember is this: always show your Medigap policy identification card, along with your Medicare card, to your medical providers. The rest is done automatically for you.
What is Medicare's rule for MRI?
They know that Medicare’s rules require that any procedure or treatment, such as surgery, a blood test or MRI, that the order is medically necessary. That means it is necessary to diagnose and treat a medical condition.
Does Healthcare.com sell insurance?
We do not sell insurance products, but there may be forms that will connect you with partners of healthcare.com who do sell insurance products. You may submit your information through this form, or call 855-617-1871 to speak directly with licensed enrollers who will provide advice specific to your situation. Read about your data and privacy.
Should You Doublecheck Your Medigap Coverage?
This means, however, that it’s up to you to check what treatments and services will be covered. If a doctor suggests a certain treatment or surgery, make sure that it’ll be covered by Original Medicare or your Medigap policy.
3. Use the Medicare Beneficiary Identifier When Billing Medicare
Healthcare providers must use (effective January 1, 2020) the 11-character alphanumeric Medicare Beneficiary Identifier (MBI) when billing Medicare, regardless of the date of service.
4. Confirm the Medicare Part B Annual Deductible Has Been Met
Every calendar year, Medicare beneficiaries must meet their Medicare Part B annual deductible before Medicare makes a payment. In 2022, the annual deductible for all Medicare Part B beneficiaries increased to $233 ($203 in 2021). Non-covered expenses will not apply toward the deductible.
5. Follow CMS Rules When Billing Medicare Advantage Plans
Medicare Advantage plans are an “all in one” alternative to traditional Medicare plans offered through private insurance companies. All Medicare Advantage plans are approved by Medicare and must follow CMS rules regarding coding, billing, submitting claims, and reimbursement.
6. Verify Vision Benefits to Avoid Billing Rejections and Denials
Many Medicare Advantage plans provide extra coverage for vision-related items or services, such as preventive and routine vision coverage, eyeglasses, and intraocular lenses (IOLs) related services.
7. Be Diligent with LCD and NCD Guidelines
Medicare Advantage plans follow Medicare guidelines, and providers must retain or have access to appropriate documentation if requested. To ensure you are coding your eye care claims correctly, be diligent with CMS Local Coverage Determinations (LCD), National Coverage Determinations (NCD), and Medicare Administrative Contractors (MAC).
8. Know When to Use an Advance Beneficiary Notice of Noncoverage
An Advance Beneficiary Notice of Noncoverage (ABN) is an informed consent document that informs the patient they may be financially liable for the costs should their insurance carrier deny the claim.
10. Review Common Coding Denials and Adjustment Reasons
A majority of claim denials are due to administrative errors. For example, the procedure code is inconsistent with the modifier you used or the required modifier is missing for the decision process (adjudication). Once you correct the errors, you can resubmit the claim to the insurance payer.