If you have Medicare Part B (the medical insurance part of Original Medicare), you’ll likely be covered for the costs of test strips. Medicare covers blood glucose testing strips as a form of durable medical equipment. As such, Medicare will typically pay 80% of the costs of test strips.
How much does Medicare pay for laboratory tests?
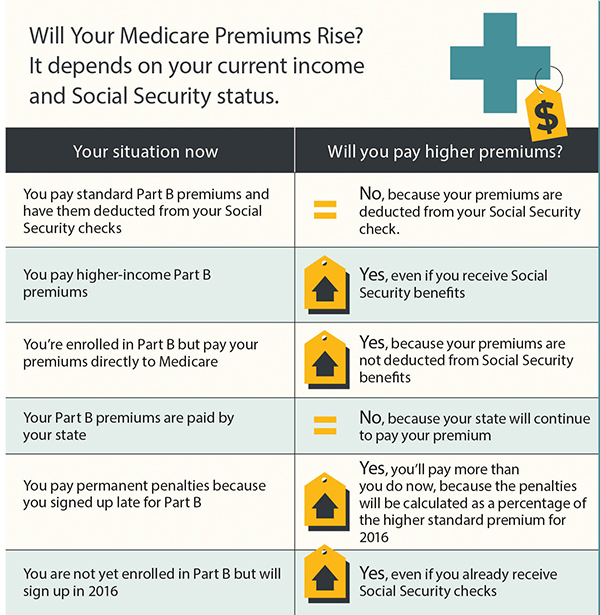
For 2021, this fee is $148.50 per month. But if you have a higher than average personal income (over $85,000) or household income (over $176,000), you …
Does Medicare cover every test?
· A fee schedule is a complete listing of fees used by Medicare to pay doctors or other providers/suppliers. This comprehensive listing of fee maximums is used to reimburse a physician and/or other providers on a fee-for-service basis. CMS develops fee schedules for physicians, ambulance services, clinical laboratory services, and durable medical ...
How much does Medicare pay for eye exams?
· Those using a non-CDC test will be reimbursed $51 per test. CMS noted that the exact reimbursement amounts may vary slightly according to the local Medicare Administrative Contractor (MAC), but all local rates are within a dollar of the above rates.
Will Medicare pay for a yearly physical exam?
· Medicare Part B also covers medically necessary outpatient blood tests. You have to meet your annual deductible for this coverage as well. In 2021, the deductible is $203 for most people. Remember,...

How much does a COVID-19 test cost?
The cost for testing should be covered by most insurance plans or through government-sponsored programs.For private pay patients, please contact your health care provider for cost to administer a COVID-19 test.
How many COVID-19 tests can I get reimbursed for?
Health plans must cover 8 individual at-home over-the-counter COVID-19 tests per person enrolled in the plan per month. That means a family of four can get 32 tests per month for free.
Will the CDC reimburse travelers for COVID-19 testing fees?
CDC is not able to reimburse travelers for COVID-19 testing fees. You may wish to contact your insurance provider or the location that provided your test about payment options.
Will I have to pay for my COVID-19 test up front?
See full answerThe Biden-Harris Administration is strongly incentivizing health plans and insurers to set up a network of convenient locations across the country such as pharmacies or retailers where people with private health coverage will be able to order online or walk in and pick up at-home over-the-counter COVID-19 tests for free, rather than going through the process of having to submit claims for reimbursement. Consumers can find out from their plan or insurer if it provides direct coverage of over-the-counter COVID-19 tests through such a program or whether they will need to submit a claim for reimbursement. If you are charged for your test after January 15, keep your receipt and submit a claim to your insurance company for reimbursement.
Can you contract COVID-19 through sexual intercourse?
Although there is currently no evidence that the COVID-19 virus transmits through semen or vaginal fluids, it has been detected in the semen of people recovering from COVID-19. We would thus recommend avoiding any close contact, especially very intimate contact like unprotected sex, with someone with active COVID-19 to minimize the risk of transmission
What if I can’t afford to pay for the at-home over-the-counter COVID-19 test(s) upfront?
See full answerHealth plans and insurers are strongly incentivized to set up a network of convenient options across the country, such as pharmacies and retailers, where people will be able to order online or walk in and pick up at-home over-the-counter COVID-19 tests for free rather than going through the process of having to submit claims for reimbursement. Consumers can find out from their plan or insurer if it is providing direct coverage of over-the-counter COVID-19 tests through such a network of preferred pharmacies or retailers.You can also access free testing in the community. A list of community-based testing sites can be found here. COVID-19 tests are also available without cost-sharing to covered individuals when administered by a health care provider like a nurse, doctor, or pharmacist, without limitation.
Can an airline deny boarding a passenger if they don't have a negative COVID-19 test?
Airlines must confirm the negative test result for all passengers or documentation of recovery before they board. If a passenger does not provide documentation of a negative test or recovery, or chooses not to take a test, the airline must deny boarding to the passenger.
Can the CDC help me get a refund for travel expenses if I delay travel because of testing or vaccination requirements for COVID-19?
See full answerCDC does not reimburse or help travelers get reimbursements for travel expenses as a result of canceled or delayed travel because of testing or vaccination requirements for air passengers flying to the United States or other issues related to COVID-19. While some companies may base their policies on CDC’s travel recommendations or requirements, each company establishes its own refund policies.In some cases, trip cancellation insurance can protect your financial investment in a trip if you need to change your itinerary in the event of an international outbreak. Visit CDC’s Travelers’ Health website if you’d like to learn more about travel insurance, including trip cancellation insurance.
Do I need to get tested for COVID-19 when traveling?
ALL Travelers Get tested for current infection with a viral test if your travel involved situations with greater risk of exposure such as being in crowded places while not wearing a well-fitting mask or respirator.
Do all COVID-19 tests require a prescription and do they need to be ordered by a physician?
A: Some COVID-19 tests require a prescription and others do not. COVID-19 tests authorized for use without a prescription include the attribute "DTC" (for direct-to-consumer home collection tests) or "OTC" (for over-the-counter at-home tests) in the EUA tables on the In Vitro Diagnostics EUA page.
When should you take Paxlovid?
When should I take Paxlovid? You have to take Paxlovid within five days of developing symptoms.
Are COVID-19 vaccines free?
FDA-authorized COVID-19 vaccines are distributed for free by states and local communities. You cannot buy COVID-19 vaccines online. You do not need to pay any out-of-pocket costs to get an authorized COVID-19 vaccine — not before, during, or after your appointment.
Should I repeat the at-home COVID-19 test if it is negative?
Some self-tests are designed to be used in a series (also known as serial testing). Consider repeating the test 24 to 48 hours later. Multiple negative tests increases the confidence that you are not infected with the virus that causes COVID-19.
What if an employee refuses to come to work for fear of infection?
Your policies, that have been clearly communicated, should address this.Educating your workforce is a critical part of your responsibility.Local and state regulations may address what you have to do and you should align with them.
How long will it take to receive my reimbursement from my plan during the COVID-19 pandemic?
See full answerHealth plans are encouraged to provide prompt reimbursement for claims for at-home tests, and consumers can find out directly from their plan how their claims process works and ask questions about reimbursement timing.The Biden-Harris Administration is strongly incentivizing plans to offer at-home over-the-counter COVID-19 tests through preferred pharmacies, retailers and online and mail-order programs without up-front out-of-pocket costs to you. Consumers can find out from their plan if it is providing such direct coverage of over-the-counter COVID-19 tests. You will not need to seek reimbursement later for tests received through such a program.
Can you get reinfected with COVID-19 after having COVID?
If you or a loved one had COVID‑19, you're likely wondering how long you might be protected from getting it again. In general, research suggests that natural immunity against infection is strong for about 3-5 months. After that, your risk of COVID‑19 reinfection may start to go up.
Does Medicare pay for mental health?
Medicare also pays for mental health care costs. Laboratory and radiology services. This includes blood tests, X-rays, and other tests. Outpatient hospital services. Medicare Part B covers some of these fees. You must pay a co-payment for outpatient hospital services The exact amount varies depending on the service.
How much is Medicare Part B 2021?
For Part B, you have to pay a monthly fee (called a premium ), which is usually taken out of your Social Security payment. For 2021, this fee is $148.50 per month. But if you have a higher than average personal income (over $85,000) or household income (over $176,000), you will have to pay a higher monthly premium for Medicare Part B.
What is Medicare Part B?
Medicare Part B pays for outpatient medical care, such as doctor visits, some home health services, some laboratory tests, some medications, and some medical equipment. (Hospital and skilled nursing facility stays are covered under Medicare Part A, as are some home health services.) If you qualify to get Medicare Part A, ...
What happens if you don't sign up for Medicare Part B?
If you don't sign up for Medicare Part B when you first become eligible (and you don’t have comparable coverage from an employer), your monthly fee may be higher than $148.50. You’ll pay a lifetime 10% penalty for every 12 months you delay your enrollment. Medical and other services.
What happens if a doctor doesn't accept assignment?
If your doctor is willing to accept what Medicare pays and won't charge you any more, they are said to "accept assignment.". But if your health care provider does not accept assignment and charges more than Medicare pays, you will have to pay the difference. For more information about Medicare Part B, see the Medicare web site at www.medicare.gov ...
What is the U0001 code?
Code U0001 identifies diagnostic testing performed by laboratories using a CDC-developed COVID-19 test. Code U0002 will be used for all non-CDC lab test for COVID-19, including those developed in-house according to new Federal Drug Administration (FDA) guidelines.
Who is Christian Worstell?
Christian Worstell is a licensed insurance agent and a Senior Staff Writer for MedicareAdvantage.com. He is passionate about helping people navigate the complexities of Medicare and understand their coverage options. .. Read full bio
Does Medicare cover blood tests?
Medicare covers many types of common blood tests needed to diagnose and manage health conditions as long as they are medically necessary. Here are a few final tips to consider:
What is Medicare Part A?
Medicare Part A offers coverage for medically necessary blood tests. Tests can be ordered by a physician for inpatient hospital, skilled nursing, hospice, home health, and other related covered services. Medicare Part B covers outpatient blood tests ordered by a physician with a medically necessary diagnosis based on Medicare coverage guidelines.
How much is Medicare Part B 2021?
You have to meet your annual deductible for this coverage as well. In 2021, the deductible is $203 for most people. Remember, you also have to pay your monthly Part B premium, which is $148.50 in 2021 for most beneficiaries.
How often does Medicare cover mammograms?
once a year if you meet criteria. *Medicare covers diagnostic mammograms more often if your doctor orders them. You are responsible for the 20 percent coinsurance cost. Other nonlaboratory diagnostic screenings Medicare covers include X-rays, PET scans, MRI, EKG, and CT scans.
Does Medicare cover ABN?
Medicare offers a tool you can use to check which tests are covered. You can also go here to look through the list of covered tests from Medicare. You can look through lists of codes and items Medicare does not cover. Before signing an ABN, ask about the cost of the test and shop around.
What is blood test?
A blood test is generally a simple procedure to measure how your body is functioning and find any early warning signs. to allow your healthcare provider to track your health and even screen for disease prevention. Coverage can depend on meeting Medicare-established criteria for testing.
What is the purpose of blood test?
Blood tests are an important diagnostic tool doctors use to screen for risk factors and monitor health conditions. A blood test is generally a simple procedure to measure how your body is functioning and find any early warning signs. Medicare covers many types of blood tests. Trusted Source.
How to get Medicare?
Initial visit: The “Welcome to Medicare” visit with your doctor aims to establish the state of your health when you enter the program and provide a plan of future care. The doctor will: 1 record your vital information (height, weight, blood pressure, body mass) 2 review your personal and family health history 3 check risk factors that could indicate future serious illnesses 4 recommend tests and screenings that could catch medical issues early and provide a checklist of preventive services (such as mammograms and vaccinations) to help you stay healthy 5 offer you the option of discussing end-of-life issues, including information on how to prepare an advance directive naming someone to make medical decisions on your behalf if you became too ill to make them yourself 6 provide counseling and referrals as appropriate
Does Medicare cover physicals?
But make sure that you ask specifically for "Welcome to Medicare" or annual wellness visit by name. If you ask for a “physical,” Medicare will not cover it and you’ll be responsible for whatever the doctor charges.
What does "assignment" mean in Medicare?
You’re enrolled in original Medicare (Part A and Part B) and you see a doctor who accepts “assignment” — meaning he or she accepts the Medicare-approved payment as full compensation. You’re enrolled in a Medicare Advantage (Part C) plan and see a doctor in the plan’s provider network.
What is an annual wellness visit?
Annual visit: During an annual wellness visit, the doctor measures your height, weight, body mass and blood pressure, and may listen to your heart through your clothes. The rest is a discussion of your own and your family’s medical history, any physical or mental impairments, and risk factors for diseases such as diabetes and depression.
Does Medicare cover allergy testing?
Some types of allergy testing are covered by Medicare. In order to qualify for these tests, your doctor must: have a documented history of your allergic reactions. show that you have significant symptoms that have not been controlled by other therapies.
Is Medicare Part D a private insurance?
Medicare Part D is outside of original Medicare. It’s purchased from a private insurance company that’s Medicare-approved. Part D typically covers the self-administered prescription drugs that aren’t covered by original Medicare. Premiums depend on the company from which you purchase Part D and the coverage your policy offers.
What is Medicare Part C?
Medicare Part C (Medicare Advantage) is purchased from a private insurance company and bundles Part A, Part B, and often Part D into a single comprehensive plan. It may also cover extra benefits not offered by Medicare such as vision and dental care.