Private insurance companies provide Medicare Advantage (MA), Medigap
Medigap
Medigap refers to various private health insurance plans sold to supplement Medicare in the United States. Medigap insurance provides coverage for many of the co-pays and some of the co-insurance related to Medicare-covered hospital, skilled nursing facility, home health care, ambulance, durable medical equipment, and doctor charges. Medigap's name is derived from the notion that it exists to …
Full Answer
How does income affect monthly Medicare premiums?
- Marriage
- Divorce/Annulment
- Death of Your Spouse
- Work Stoppage or Reduction
- Loss of Income-Producing Property
- Loss of Pension Income
- Employer Settlement Payment
What is the monthly premium for Medicare Part B?
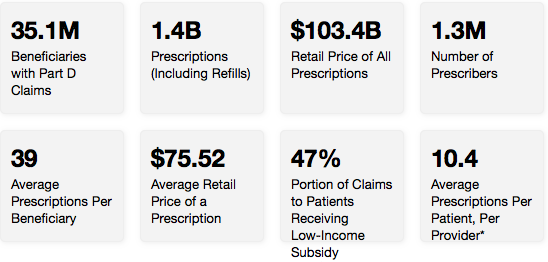
The standard monthly premium for Medicare Part B is $148.50 per month in 2021. Some Medicare beneficiaries may pay more or less per month for their Part B coverage. The Part B premium is based on your reported income from two years ago (2019).
How do I Pay my Medicare premium?
Ways to Pay Your Medicare Premium
- Most people don’t receive a bill from Medicare for their Part A and Part B premiums.
- If you do receive a bill (Medicare form CMS-500), you can pay it online through your bank or Medicare Easy Pay.
- You can use your debit or credit card to pay, either online or by mailing your credit card information to Medicare.
Who pays for Medicare premiums?
Kroger adopted a carrot-and-stick approach. The company offers $100 bonuses for workers to get vaccinated. It also offered customer and employee giveaways to encourage the shots, including five $1 million checks and free groceries.
How are insurance companies paid by Medicare?
The plans receive some funding through monthly plan premiums, but most of the money comes from Medicare. The private insurance companies that offer the plans receive a payment each month from Medicare. This covers the costs of Medicare parts A and B for each beneficiary.
How are Medicare premiums paid?
premium deducted automatically from their Social Security benefit payment (or Railroad Retirement Board benefit payment). If you don't get benefits from Social Security (or the Railroad Retirement Board), you'll get a premium bill from Medicare. Get a sample of the Medicare bill.
How Does Medicare pay providers in Part B?
If the provider accepts assignment (agrees to accept Medicare's approved amount as full reimbursement), Medicare pays the Part B claim directly to him/her for 80% of the approved amount. You are responsible for the remaining 20% (this is your coinsurance ).
Are Medicare premiums paid monthly or quarterly?
BILL TYPE Some people with Medicare are billed either monthly or quarterly. If you are billed for Part A or IRMAA Part D, you will be billed monthly. If this box says: • FIRST BILL, it means your last payment was received timely or this is your initial bill. SECOND BILL, it means a payment is late by at least 60 days.
Do you have to pay Medicare premiums?
Most people don't pay a monthly premium for Part A (sometimes called "premium-free Part A"). If you buy Part A, you'll pay up to $499 each month in 2022. If you paid Medicare taxes for less than 30 quarters, the standard Part A premium is $499.
Why do doctors not like Medicare Advantage plans?
If they don't say under budget, they end up losing money. Meaning, you may not receive the full extent of care. Thus, many doctors will likely tell you they do not like Medicare Advantage plans because private insurance companies make it difficult for them to get paid for their services.
How do providers submit claims to Medicare?
Contact your doctor or supplier, and ask them to file a claim. If they don't file a claim, call us at 1-800-MEDICARE (1-800-633-4227). TTY: 1-877-486-2048. Ask for the exact time limit for filing a Medicare claim for the service or supply you got.
Does Medicare Part B cover 100 percent?
Although Medicare covers most medically necessary inpatient and outpatient health expenses, Medicare reimbursement sometimes does not pay 100% of your medical costs.
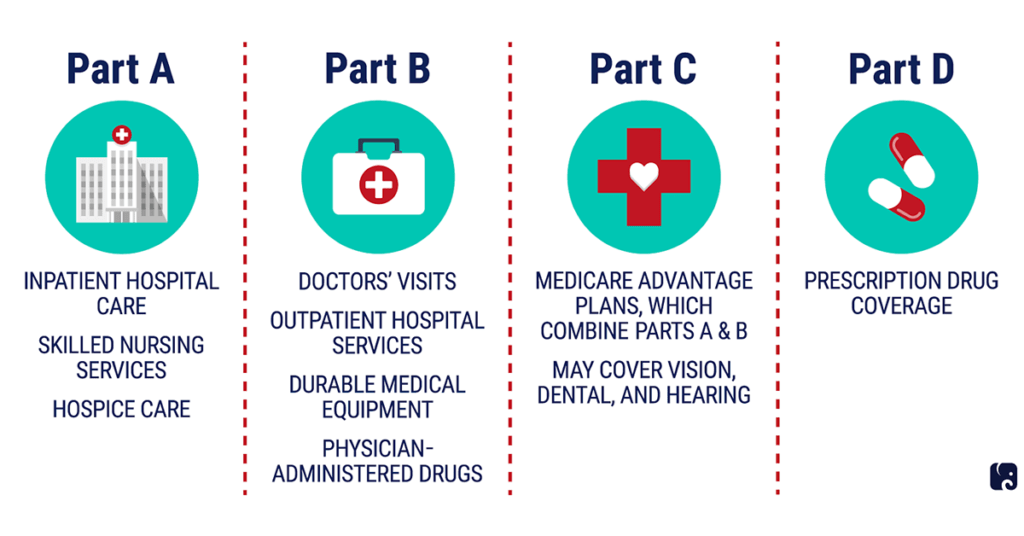
Medicare Advantage (Part C)
You pay for services as you get them. When you get a covered service, Medicare pays part of the cost and you pay your share.
You can add
You join a Medicare-approved plan from a private company that offers an alternative to Original Medicare for your health and drug coverage.
Most plans include
Some extra benefits (that Original Medicare doesn’t cover – like vision, hearing, and dental services)
Medicare drug coverage (Part D)
If you chose Original Medicare and want to add drug coverage, you can join a separate Medicare drug plan. Medicare drug coverage is optional. It’s available to everyone with Medicare.
Medicare Supplement Insurance (Medigap)
Medicare Supplement Insurance (Medigap) is extra insurance you can buy from a private company that helps pay your share of costs in Original Medicare.
What is the SGR for Medicare?
Under current law, Medicare’s physician fee-schedule payments are subject to a formula, called the Sustainable Growth Rate (SGR) system, enacted in 1987 as a tool to control spending. For more than a decade this formula has called for cuts in physician payments, reaching as high as 24 percent.
Does Medicare have a fee for service?
Current payment systems in traditional Medicare have evolved over the last several decades, but have maintained a fee-for-service payment structure for most types of providers. In many cases, private insurers have modeled their payment systems on traditional Medicare, including those used for hospitals and physicians.
Does Medicare use prospective payment systems?
Medicare uses prospective payment systems for most of its providers in traditional Medicare. In general, these systems require that Medicare pre-determine a base payment rate for a given unit of service (e.g., a hospital stay, an episode of care, a particular service).
What is an HMO plan?
Health Maintenance Organization (HMO) plan is a type of Medicare Advantage Plan that generally provides health care coverage from doctors, other health care providers, or hospitals in the plan’s network (except emergency care, out-of-area urgent care, or out-of-area dialysis). A network is a group of doctors, hospitals, and medical facilities that contract with a plan to provide services. Most HMOs also require you to get a referral from your primary care doctor for specialist care, so that your care is coordinated.
What happens if you get a health care provider out of network?
If you get health care outside the plan’s network, you may have to pay the full cost. It’s important that you follow the plan’s rules, like getting prior approval for a certain service when needed. In most cases, you need to choose a primary care doctor. Certain services, like yearly screening mammograms, don’t require a referral. If your doctor or other health care provider leaves the plan’s network, your plan will notify you. You may choose another doctor in the plan’s network. HMO Point-of-Service (HMOPOS) plans are HMO plans that may allow you to get some services out-of-network for a higher copayment or coinsurance. It’s important that you follow the plan’s rules, like getting prior approval for a certain service when needed.
What is a special needs plan?
Special Needs Plan (SNP) provides benefits and services to people with specific diseases, certain health care needs, or limited incomes. SNPs tailor their benefits, provider choices, and list of covered drugs (formularies) to best meet the specific needs of the groups they serve.
Do providers have to follow the terms and conditions of a health insurance plan?
The provider must follow the plan’s terms and conditions for payment, and bill the plan for the services they provide for you. However, the provider can decide at every visit whether to accept the plan and agree to treat you.
Can a provider bill you for PFFS?
The provider shouldn’t provide services to you except in emergencies, and you’ll need to find another provider that will accept the PFFS plan .However, if the provider chooses to treat you, then they can only bill you for plan-allowed cost sharing. They must bill the plan for your covered services. You’re only required to pay the copayment or coinsurance the plan allows for the types of services you get at the time of the service. You may have to pay an additional amount (up to 15% more) if the plan allows providers to “balance bill” (when a provider bills you for the difference between the provider’s charge and the allowed amount).
What is Medicare Easy Pay?
Medicare Easy Pay is a free way to set up recurring payments for your Medicare premium. If you sign up for Medicare Easy Pay, your Medicare premiums will be automatically deducted from your checking or savings account each month. If you get a "Medicare Premium Bill" (Form CMS-500) from Medicare, you can sign up for Medicare Easy Pay.
How long does it take to get Medicare Easy Pay?
Mail your completed form to: It can take up to 6-8 weeks for your automatic deductions to start. Until your automatic deductions start, you'll need to pay your premiums another way. If you can't process your Medicare Easy Pay request, we'll send you a letter explaining why.
When will Medicare Easy Pay deduct premiums?
We'll deduct your premium from your bank account on or around the 20th of the month.
How long does it take to get Medicare if you change your bank account?
If you stop Medicare Easy Pay: It can take up to 4 weeks for your automatic deductions to stop.
What happens when someone receives Medicare benefits?
When someone who receives Medicare benefits visits a physician’s office, they provide their Medicare information , and instead of making a payment, the bill gets sent to Medicare for reimbursement.
Why do doctors accept Medicare?
The reason so many doctors accept Medicare patients, even with the lower reimbursement rate, is that they are able to expand their patient base and serve more people.
Do you have to pay Medicare bill after an appointment?
For some patients, this means paying the full amount of the bill when checking out after an appointment, but for others , it may mean providing private insurance information and making a co-insurance or co-payment amount for the services provided. For Medicare recipients, however, the system may work a little bit differently.
Can a patient receive treatment for things not covered by Medicare?
A patient may be able to receive treatment for things not covered in these guidelines by petitioning for a waiver. This process allows Medicare to individually review a recipient’s case to determine whether an oversight has occurred or whether special circumstances allow for an exception in coverage limits.