MTM services may be billed via universal claim form (HCFA-1500) using MTM CPT Codes. Universal claim forms are available online.
Full Answer
Does Medicaid Cover my MTM services?
May 22, 2020 · Requirements for Medication Therapy Management (MTM) Programs: Under 423.153 (d), a Part D sponsor must have established a MTM program that: Ensures optimum therapeutic outcomes for targeted beneficiaries through improved medication use. Reduces the risk of adverse events. Is developed in cooperation with licensed and practicing pharmacists …
What is the CPT code for MTM services?
Dec 14, 2021 · Developing a pharmaceutical treatment strategy. Medication therapy selection, initiation, modification, and administration. Monitoring and assessing the patient’s reaction to therapy, as well as its safety and efficacy. Conducting a thorough medication review to detect, treat, and prevent medication-related issues, such as adverse drug incidents.
Is MTM considered an administrative cost by CMS?
Feb 07, 2017 · We have been told that the codes we will start seeing are G0463.1-5 based on 15-minute increments for Medicare and replacements as well as 99606.0 (initial visit) and 99607.0 (for each additional 15 minutes) for all other payers. We will be billing these services under the ordering provider, and we should see a note from one of the pharmacists.
What percentage of MTM programs use medical data to identify beneficiaries?
Dec 15, 2021 · on an MTM claim must be a diagnosis code from the list of chronic conditions for MTM eligibility. The complete list can be found by clicking . here. Pharmacists are able to bill Medicaid’s CHAMPS system using the current procedural terminology (CPT) billing codes identified under Table 1. Note that each CPT Code is billed for a 15 minute ...

What part does Medicare cover MTM?
Medication Therapy Management (MTM) services are offered at no additional charge to Medicare Advantage plan members with Part D coverage who meet Centers for Medicare and Medicaid Services (CMS) criteria.
How do you bill for medication management?
What are MTM CPT codes?
What are the 5 components of MTM?
Which individual S may provide MTM services based on federal law?
What is the term for third party programs for Medicare Part D?
What is procedure code 90863?
How Much Does Medicare pay for 99211?
Reporting 99211 can bring additional revenue into your practice. Specific payment amounts will vary by payer, but the average unadjusted 2004 payment from Medicare for a 99211 service is $21.
What CPT codes can pharmacists bill?
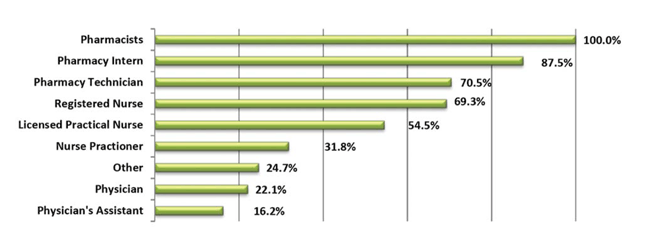
Which of the following healthcare professionals would be involved in an MTM review?
What is a factor when determining a patient's eligibility for MTM services?
Which document in MTM is a comprehensive medication record of the patient's prescription and nonprescription medications?
What do pharmacists need to do to improve MTM?
Pharmacists must train their staff, including interns and technicians, to help enhance MTM services. This may involve making phone calls, scheduling appointments, and making other preparations that do not involve clinical expertise.
When did MTM start?
It is a known fact that MTM services began in 2003 following the passage of the Medicare Modernization Act, and in 2006 MTM services were provided to Medicare Part D beneficiaries.
What is MTM in Medicaid?
MTM may be viewed as a value-added service that can be employed as part of a broader benefit. Some states have integrated MTM into broader Medicaid initiatives, such as a value-based purchasing program or a state waiver that tests a set of delivery or payment redesigns, with evidence reflecting improved health outcomes.26,27,28,29 Stakeholders can use these experiences to inform their decision making when addressing issues faced by communities experiencing particularly high prevalence of chronic conditions.
What are the benefits of MTM?
The positive results of MTM are especially relevant to the Medicaid population, given the disproportionate burden that chronic disease has on Medicaid beneficiaries. Medicaid beneficiaries experience higher rates of hypertension than people with commercial or private insurance plans. 14 Medicaid beneficiaries are also more likely than the general public to have at least one chronic condition, frequently having multiple diseases, such as hyperlipidemia, hypertension, and diabetes.14 The health disparities that Medicaid beneficiaries experience are due to a number of factors; they face higher levels of social barriers to health care than their privately insured peers, as well as higher rates of under- and unemployment, housing instability, substance use disorder, and mental illness.15,16 However, multisite MTM programs like Project IMPACT: Diabetes demonstrate that MTM can improve clinical outcomes for underserved communities that are disproportionately affected by chronic disease.10
What is MTM in Tennessee?
The Tennessee MTM pilot program, which began in 2018, offers MTM as a benefit to Medicaid managed care beneficiaries participating in the state’s Patient-Centered Medical Home (PCMH) or Health Link (HL) programs.30 PCMH and HL programs are care delivery models developed to coordinate health care services for Medicaid beneficiaries. Approximately 37% of Tennessee Medicaid beneficiaries are enrolled in a PCMH organization.31 For the MTM program, pharmacists provide services to beneficiaries who meet certain clinical risk criteria, through a collaborative practice agreement with PCMH and HL organizations.30
What are the core elements of MTM?
In states with more permissive scope-of-practice laws, pharmacists may be able to offer supplementary services, such as providing certain medical tests. State Medicaid stakeholders could review what activities pharmacists in their state are authorized to perform, in order to optimize how the Medicaid program can leverage their skills and services.17
What are the MTM activities?
MTM activities included under the five core elements are generally activities that pharmacists in all states are permitted to do, regardless of the expansiveness of a state’s pharmacist scope-of-practice laws. 17
How many states have MTM?
Some states address pharmacist-provided MTM through statutes, regulations, or other policies. As of November 30, 2019, 25 states had laws addressing pharmacist-provided MTM services, including some laws specific to the Medicaid program.† Of these, 12 states included provision of MTM services in pharmacists’ scope of practice, 13 states’ laws described activities that fit within the scope of MTM services, and eight states’ laws permitted Medicaid reimbursement for MTM services provided by pharmacists (Figure 1).In nine states, the law directed a state agency to
Can a pharmacist prescribe in Idaho?
Idaho’s pharmacist scope-of-practice laws are some of the broadest in the nation, offering pharmacists prescribing authority not permitted in other states. Since 2019, pharmacists in Idaho may prescribe drugs as long as one of the following four criteria are met: The conditions (1) do not require a new diagnosis, (2) are “minor and generally self-limiting,” (3) have a test to guide clinical decision making that is waived under the federal Clinical Laboratory Improvement Amendments of 1988 (CLIA), or (4) in an emergency, during which drugs are immediately necessary to protect the health and safety of a patient.18 This expanded authority could allow Idaho pharmacists who identify drug therapy issues to use their broad prescribing authority to adjust patients’ medication regimens.