Switching Medicare supplement plans requires you to simply contact the new insurance provider and apply for a plan. If your application is accepted, contact your old plan provider and request a cancellation of your policy. If switching plans within the same provider, just contact the provider and notify them you would like to switch plans.
Is Medicare and Medicaid the same thing?
No, these are two separate and distinct programs. Medicare is a federal program designed to assist older persons with healthcare coverage while Medicaid is funded jointly between the Federal and state governments and assists low income individuals and families.
Does Someone on Medicaid automatically qualify for Medicare?
Persons who are eligible for both Medicare and Medicaid are called “dual eligibles”, or sometimes, Medicare-Medicaid enrollees. To be considered dually eligible, persons must be enrolled in Medicare Part A (hospital insurance), and / or Medicare Part B (medical insurance).
Can you get Medicare and Medicaid at the same time?
Medicare and Medicaid are both public health insurance programs. If you are dual eligible, you can have both Medicare and Medicaid coverage at the same time. Two of the key differences between Medicare vs. Medicaid include: Medicare is for people age 65 and over and for certain people under 65 who have a qualifying disability.
Do I need Medicare if I have Medicaid?
The purpose of Medicare Supplement Insurance is to cover the cost left by deductibles and coinsurance in Original Medicare, but as full Medicaid coverage should cover the majority of those costs, a Medicare Supplement Insurance policy isn’t necessary. 3 A number of factors influence your coverage eligibility and decisions.

What is the highest income to qualify for Medicaid?
Federal Poverty Level thresholds to qualify for Medicaid The Federal Poverty Level is determined by the size of a family for the lower 48 states and the District of Columbia. For example, in 2022 it is $13,590 for a single adult person, $27,750 for a family of four and $46,630 for a family of eight.
What are the disadvantages of Medicaid?
Disadvantages of Medicaid They will have a decreased financial ability to opt for elective treatments, and they may not be able to pay for top brand drugs or other medical aids. Another financial concern is that medical practices cannot charge a fee when Medicaid patients miss appointments.
How do I switch from Medicare to medical?
To switch to Original Medicare, contact your current plan, or call us at 1-800-MEDICARE.
What is the difference in Medicare and Medicaid?
The difference between Medicaid and Medicare is that Medicaid is managed by states and is based on income. Medicare is managed by the federal government and is mainly based on age. But there are special circumstances, like certain disabilities, that may allow younger people to get Medicare.
Who qualifies for Medicaid?
To participate in Medicaid, federal law requires states to cover certain groups of individuals. Low-income families, qualified pregnant women and children, and individuals receiving Supplemental Security Income (SSI) are examples of mandatory eligibility groups (PDF, 177.87 KB).
How can I get Medicaid?
There are two ways to apply for Medicaid:Contact your state Medicaid agency. You must be a resident of the state where you are applying for benefits.Fill out an application through the Health Insurance Marketplace.
How do I qualify for dual Medicare and Medicaid?
Persons who are eligible for both Medicare and Medicaid are called “dual eligibles”, or sometimes, Medicare-Medicaid enrollees. To be considered dually eligible, persons must be enrolled in Medicare Part A (hospital insurance), and / or Medicare Part B (medical insurance).
Can you have Medicare and Medicaid at the same time?
Yes. A person can be eligible for both Medicaid and Medicare and receive benefits from both programs at the same time.
Can you have Medicare and Medicaid?
Medicare-Medicaid Plans Medicare is working with some states and health plans to offer demonstration plans for certain people who have both Medicare and Medicaid and make it easier for them to get the services they need. They're called Medicare-Medicaid Plans.
Who pays for Medicaid?
The Medicaid program is jointly funded by the federal government and states. The federal government pays states for a specified percentage of program expenditures, called the Federal Medical Assistance Percentage (FMAP).
What are the 4 types of Medicare?
There are four parts of Medicare: Part A, Part B, Part C, and Part D.Part A provides inpatient/hospital coverage.Part B provides outpatient/medical coverage.Part C offers an alternate way to receive your Medicare benefits (see below for more information).Part D provides prescription drug coverage.
How does Medicaid work?
The Medicaid entitlement is based on two guarantees: first, all Americans who meet Medicaid eligibility requirements are guaranteed coverage, and second, states are guaranteed federal matching dollars without a cap for qualified services provided to eligible enrollees.
Your other coverage
Do you have, or are you eligible for, other types of health or prescription drug coverage (like from a former or current employer or union)? If so, read the materials from your insurer or plan, or call them to find out how the coverage works with, or is affected by, Medicare.
Cost
How much are your premiums, deductibles, and other costs? How much do you pay for services like hospital stays or doctor visits? What’s the yearly limit on what you pay out-of-pocket? Your costs vary and may be different if you don’t follow the coverage rules.
Doctor and hospital choice
Do your doctors and other health care providers accept the coverage? Are the doctors you want to see accepting new patients? Do you have to choose your hospital and health care providers from a network? Do you need to get referrals?
Prescription drugs
Do you need to join a Medicare drug plan? Do you already have creditable prescription drug coverag e? Will you pay a penalty if you join a drug plan later? What will your prescription drugs cost under each plan? Are your drugs covered under the plan’s formulary? Are there any coverage rules that apply to your prescriptions?
Quality of care
Are you satisfied with your medical care? The quality of care and services given by plans and other health care providers can vary. Get help comparing plans and providers
Convenience
Where are the doctors’ offices? What are their hours? Which pharmacies can you use? Can you get your prescriptions by mail? Do the doctors use electronic health records prescribe electronically?
Key takeaways
What costs should you expect if you’re moving from expanded Medicaid to Medicare?
Millions under expanded Medicaid will transition to Medicare
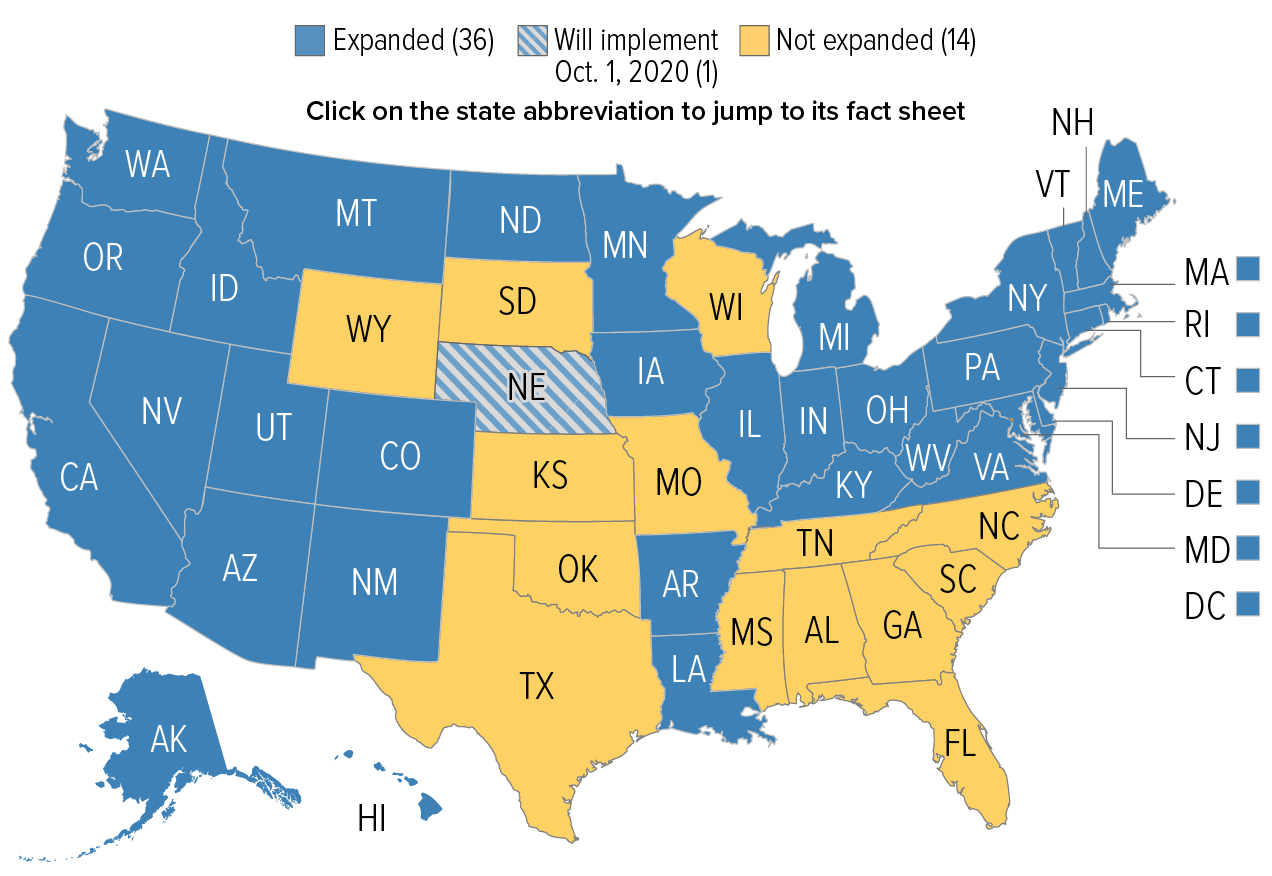
There are currently almost 20 million people covered under expanded Medicaid, accounting for almost a quarter of all Medicaid enrollees nationwide. Under ACA rules, there are no asset limitations for Medicaid eligibility for pregnant women, children, or adults eligible due to Medicaid expansion.
Moving from expanded Medicaid to Medicare Advantage
Depending on your circumstances, you might choose to enroll in a Medicare Advantage plan that provides prescription, dental, and vision coverage – and caps enrollees’ annual out-of-pocket costs for Parts A and B, which traditional Medicare does not do.
Transitioning from expanded Medicaid to Medigap
The more expensive way to cover the gaps in traditional Medicare is to buy a Medigap policy, which generally costs anywhere from a minimum of $25/month to more than $200/month to cover out-of-pocket costs for Parts A and B. That’s on top of premiums for Medicare Parts B and D (prescription drugs).
Medicare can pull you out of the coverage gap
Although the transition from expanded Medicaid to Medicare can be financially challenging, eligibility for Medicare will likely come as a welcome relief if you’ve been in the coverage gap in one of the 11 states that have refused to expand Medicaid.
What steps do I need to take to move from expanded Medicaid to Medicare?
If you’re enrolled in expanded Medicaid and you’ll soon be 65, you’ll want to familiarize yourself with the health coverage and assistance programs that might be available to you.
Legislation aims to make Medicare more affordable for lower-income Americans
The Improving Medicare Coverage Act, introduced in the U.S. House in September by Washington Representative Pramila Jayapal, would do away with cost-sharing and premiums for Medicare beneficiaries with income up to 200% of the poverty level (it would also lower the Medicare eligibility age to 60).
How to apply for medicaid?
How to Apply. To apply for Medicare, contact your local Social Security Administration (SSA) office. To apply for Medicaid, contact your state’s Medicaid agency. Learn about the long-term care Medicaid application process. Prior to applying, one may wish to take a non-binding Medicaid eligibility test.
What is Medicare and Medicaid?
Differentiating Medicare and Medicaid. Persons who are eligible for both Medicare and Medicaid are called “dual eligibles”, or sometimes, Medicare-Medicaid enrollees. Since it can be easy to confuse the two terms, Medicare and Medicaid, it is important to differentiate between them. While Medicare is a federal health insurance program ...
How much does Medicare Part B cost?
For Medicare Part B (medical insurance), enrollees pay a monthly premium of $148.50 in addition to an annual deductible of $203. In order to enroll in a Medicare Advantage (MA) plan, one must be enrolled in Medicare Parts A and B. The monthly premium varies by plan, but is approximately $33 / month.
What is the income limit for Medicaid in 2021?
In most cases, as of 2021, the individual income limit for institutional Medicaid (nursing home Medicaid) and Home and Community Based Services (HCBS) via a Medicaid Waiver is $2,382 / month. The asset limit is generally $2,000 for a single applicant.
How old do you have to be to qualify for medicare?
Citizens or legal residents residing in the U.S. for a minimum of 5 years immediately preceding application for Medicare. Applicants must also be at least 65 years old. For persons who are disabled or have been diagnosed with end-stage renal disease or Lou Gehrig’s disease (amyotrophic lateral sclerosis), there is no age requirement. Eligibility for Medicare is not income based. Therefore, there are no income and asset limits.
Does Medicare cover out-of-pocket expenses?
Persons who are enrolled in both Medicaid and Medicare may receive greater healthcare coverage and have lower out-of-pocket costs. For Medicare covered expenses, such as medical and hospitalization, Medicare is always the first payer (primary payer). If Medicare does not cover the full cost, Medicaid (the secondary payer) will cover the remaining cost, given they are Medicaid covered expenses. Medicaid does cover some expenses that Medicare does not, such as personal care assistance in the home and community and long-term skilled nursing home care (Medicare limits nursing home care to 100 days). The one exception, as mentioned above, is that some Medicare Advantage plans cover the cost of some long term care services and supports. Medicaid, via Medicare Savings Programs, also helps to cover the costs of Medicare premiums, deductibles, and co-payments.
Does Medicaid cover nursing home care?
Medicaid also pays for nursing home care, and often limited personal care assistance in one’s home. While some states offer long-term care and supports in the home and community thorough their state Medicaid program, many states offer these supports via 1915 (c) Medicaid waivers.
How to cancel Marketplace?
You can cancel your Marketplace plan any time, but there are important things to consider: 1 No one plans to get sick or hurt, but bad things happen — even to healthy people. Having medical debt can really limit your options. If you're paying for every medical service yourself, you may make some health care decisions based on money instead of what's best for your health. 2 Learn more about the benefits of health coverage.
Can medical debt limit your options?
Having medical debt can really limit your options. If you're paying for every medical service yourself, you may make some health care decisions based on money instead of what's best for your health. Learn more about the benefits of health coverage. To cancel your plan: Learn how to cancel your coverage.
Can I change my Marketplace health insurance?
You can change Marketplace health coverage through August 15 due to the coronavirus disease 2019 (COVID-19) emergency. If you’re currently enrolled in Marketplace coverage, you may qualify for more tax credits. Learn more about new, lower costs. Note: If you change plans or add a new household member, any out-of-pocket costs you already paid on ...
Can I change my health insurance in 2021?
You can also still change 2021 health plans any time if you qualify for a Special Enrollment Period due to a life event like losing other coverage, getting married, moving, or having a baby. You usually have 60 days from the life event to enroll in a new plan, but you should report your change as soon as possible.
How long does it take to switch from Medicare Advantage to Original Medicare?
If you’re covered by both Medicare and Medicaid and then you lose eligibility for Medicaid, you can switch from Medicare Advantage to Original Medicare up to three months from the date you lose Medicaid eligibility, or the date you’re notified, whichever is later.
How long can you switch to Medicare Advantage?
If you wait to tell your Medicare Advantage plan about your move, then you can switch to Original Medicare for up to two full months after the month that you inform your plan.
How to disenroll from Medicare Advantage?
Visit your local Social Security Office and ask to be disenrolled from Medicare Advantage ; Call 1-800-MEDICARE (1-800-633-4227) and process your disenrollment over the phone; or. Contact your Medicare Advantage insurer directly and request a disenrollment form.
What is Medicare Supplement Plan?
This kind of plan, also known as a Medigap policy, pays for gaps in Medicare’s coverage. For instance, Medicare Part B pays 80% of covered costs after you pay your annual deductible. A Medigap policy would pay the remaining 20% ...
When does Medicare open enrollment end?
Medicare Advantage Open Enrollment Period. This special opportunity to leave Medicare Advantage lasts from January 1 through March 31 each year. If you disenroll during January, your changes will be effective on February 1. If you disenroll during February, your changes will be effective on March 1. If you disenroll during March, your changes will ...
Can you switch to Original Medicare if you are eligible for medicaid?
If You Become Eligible for Medicaid. Once you become eligible for Medicaid benefits, then you can drop your Medicare Advantage plan and switch to Original Medicare. While you’re covered under Medicare and Medicaid, you can change that coverage once a quarter during the first three quarters of the year ...
Does Medicare Part B pay 80% of the cost?
For instance, Medicare Part B pays 80% of covered costs after you pay your annual deductible. A Medigap policy would pay the remaining 20% due. But if you’ve missed your Medigap Open Enrollment Period, an insurer could deny you coverage due to your health history.
