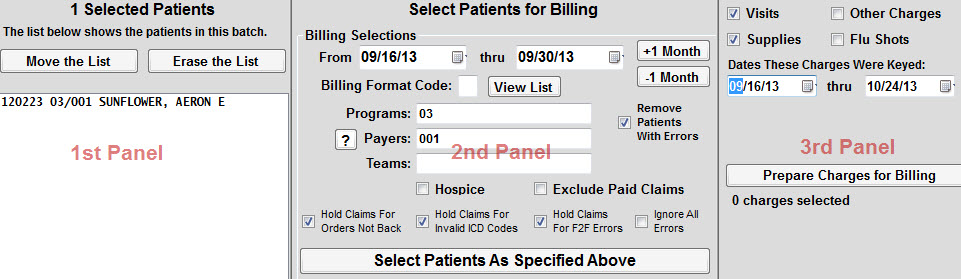
- sign in. Sign in to myGov and select Medicare. If you’re using the app, open it and enter your myGov pin. On your homepage, select Make a claim.
- confirm patient details. If you have multiple people listed on your Medicare card, select who received the service, followed by Next.
- confirm payment details. Tell us if the service has been paid in full. No if you haven’t, then Next. ...
- add provider and item details. Tell us the doctor’s Provider number. You can find this on the account or receipt. ...
- review and submit. Review your claim details. If the details are wrong, select Edit to make changes. Cancel to stop the claim.
- sign out. From your homepage you can complete other transactions or select the myGov icon to return to myGov. ...
How to file your claims with Medicare?
To pay your bill, you can: Log into (or create) your secure Medicare account. Sign up for Medicare Easy Pay. Check if your bank offers an online bill payment service to pay electronically from your savings or checking account. Mail your payment by check, money order, credit card, or debit card ...
Do I need to file any claims with Medicare?
Sep 15, 2021 · How to File a Medicare Claim Yourself If you need to file your own Medicare claim, you’ll need to fill out a Patient Request for Medical Payment Form, the 1490S. Make sure it’s filed no later than 1 full calendar year after the date of service. Medicare can’t pay its share if the submission doesn’t happen within 12 months.
How do I make a Medicare claim?
Medicare Part A (Hospital Insurance) or Medicare Part B (Medical Insurance) claims: Log into (or create) your secure Medicare account. You’ll usually be able to see a claim within 24 hours after Medicare processes it. Check your Medicare Summary Notice (MSN) . The MSN is a notice that people with Original Medicare get in the mail every 3 months.
How long do you have to submit a claim to Medicare?
Dec 01, 2021 · How to Submit Claims: Claims may be electronically submitted to a Medicare Administrative Contractor (MAC) from a provider using a computer with software that meets electronic filing requirements as established by the HIPAA claim standard and by meeting CMS requirements contained in the provider enrollment & certification category area of this web site …
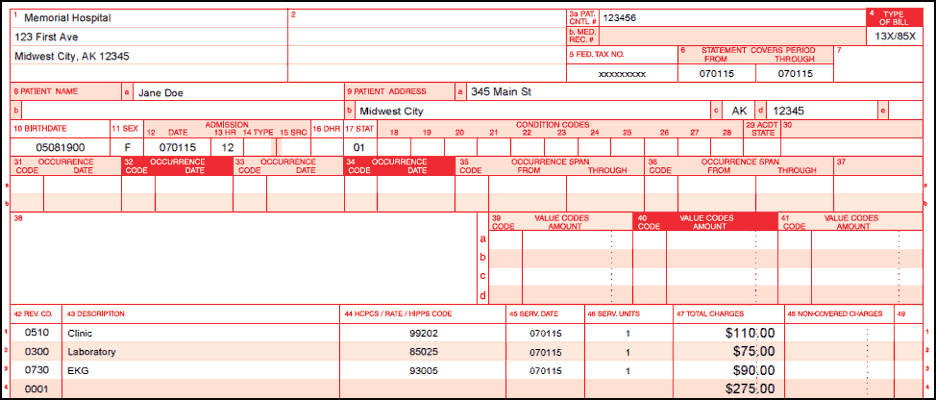
How do I get my Medicare reimbursement?
What is the first step in submitting Medicare claims?
- The first thing you'll need to do when filing your claim is to fill out the Patient's Request for Medical Payment form. ...
- The next step in filing your own claim is to get an itemized bill for your medical treatment.
Who submits Medicare Part A claims?
What form is used to send claims to Medicare?
Can you submit your own claims to Medicare?
How do I claim Medicare online?
How do I get reimbursed for Medicare Part B?
How long do you have to submit a claim to Medicare?
How do I check my Medicare billing?
Where do I send Medicare claims?
| State | Claim mailing address | |
|---|---|---|
| Alabama | AL | Alabama Medicare Part B Claims PO Box 830140 Birmingham, AL 35283-0140 |
| Georgia | GA | Georgia Medicare Part B Claims PO Box 12847 Birmingham, AL 35202-2847 |
| Tennessee | TN | Tennessee Part B Claims PO Box 12086 Birmingham, AL 35202-2086 |
What is the difference between UB-04 and CMS 1500?
Who is eligible for Medicare reimbursement?
File a complaint (grievance)
Find out how to file a complaint (also called a "grievance") if you have a concern about the quality of care or other services you get from a Medicare provider. Contact your State Health Insurance Assistance Program (SHIP) for local, personalized Medicare counseling.
File a claim
Get information on how and when to file a claim for your Medicare bills (sometimes called "Medicare billing"). You should only need to file a claim in very rare cases.
Check the status of a claim
Check your claim status with your secure Medicare account, your Medicare Summary Notice (MSN), your Explanation of Benefits (EOB), Medicare's Blue Button, or contact your plan.
File an appeal
How to appeal a coverage or payment decision made by Medicare, your health plan, drug plan or Medicare Medical Savings Account (MSA) Plan.
Your right to a fast appeal
Learn how to get a fast appeal for Medicare-covered services you get that are about to stop.
Authorization to Disclose Personal Health Information
Access a form so that someone who helps you with your Medicare can get information on your behalf.
What is Medicare 500?
The “Medicare Premium Bill ” (CMS-500) is a bill for people who pay Medicare directly for their Part A premium, Part B premium, and/or Part D IRMAA (an extra amount in addition to the Medicare Part D premium). If you’re having trouble paying your premiums now or if you have any questions about your Medicare premium bill, call us at 1-800-MEDICARE.
What is the April bill?
If you get a bill each month, the bill you get in April is for May coverage. If you get a bill every 3 months, the bill you get in April is for May, June, and July coverage. Your bill may also include premiums for past months if you missed a payment, if you're getting your first bill, or if you had a change in your premium amount.
Do you get a confirmation number when you pay Medicare?
You'll get a confirmation number when you make your payment. Your credit/debit card statement will show a payment made to "CMS Medicare.". You can't set up payments automatically each month — you'll need to log into your account each time you need to pay your premium.
How to file a claim for Medicare?
How to File a Medicare Claim Yourself. If you need to file your own Medicare claim, you’ll need to fill out a Patient Request for Medical Payment Form, the 1490S. Make sure it’s filed no later than 1 full calendar year after the date of service. Medicare can’t pay its share if the submission doesn’t happen within 12 months.
How to check Medicare claim status?
You can easily check the status of Medicare claims by visiting MyMedicare.gov; all you need to do is log into your account. Most claims are sent in within 24 hours of processing.
What to do if Medicare is denied?
If your Medicare claim is denied, you’ll want to file an appeal.
What is a claim number?
A claim number helps Medicare track your claim. This number is most likely your social security number with a letter after it.
How long does it take for Medicare to process a claim?
How Are Medicare Claims Processed? Your doctor will submit the claims. Then, Medicare will take about 30 days to process the claim. When it comes to Part A services, Medicare will pay the hospital directly. But, with Part B claims payment depends on whether or not the doctor accepts Medicare assignment.
Can a doctor submit a claim to Medicare?
But, in some instances, like foreign travel or doctors that don’t accept assignment, you’ll file the claim. If you receive an Advance Beneficiary Notice of Noncoverage and decide to proceed, it’s best to request your doctor submit the claim to Medicare before billing you.
Is Medicare always primary?
Medicare isn’t always primary. In this instance where Medicare is secondary, you’ll bill the primary insurance company before Medicare. Then, you can submit an Explanation of Benefits from the primary payor with the claim. The primary payer must process the claim first, and if they don’t, your doctor may bill Medicare.
How long does it take to see a Medicare claim?
Log into (or create) your secure Medicare account. You’ll usually be able to see a claim within 24 hours after Medicare processes it. A notice you get after the doctor, other health care provider, or supplier files a claim for Part A or Part B services in Original Medicare.
What is Medicare Part A?
Check the status of a claim. To check the status of. Medicare Part A (Hospital Insurance) Part A covers inpatient hospital stays, care in a skilled nursing facility, hospice care, and some home health care. or.
What is MSN in Medicare?
The MSN is a notice that people with Original Medicare get in the mail every 3 months. It shows: All your Part A and Part B-covered services or supplies billed to Medicare during a 3-month period. What Medicare paid. The maximum amount you may owe the provider. Learn more about the MSN, and view a sample.
What is Medicare Advantage Plan?
Medicare Advantage Plan (Part C) A type of Medicare health plan offered by a private company that contracts with Medicare. Medicare Advantage Plans provide all of your Part A and Part B benefits, excluding hospice. Medicare Advantage Plans include: Health Maintenance Organizations. Preferred Provider Organizations.
Is Medicare paid for by Original Medicare?
Medicare services aren’t paid for by Original Medicare. Most Medicare Advantage Plans offer prescription drug coverage. or other. Medicare Health Plan. Generally, a plan offered by a private company that contracts with Medicare to provide Part A and Part B benefits to people with Medicare who enroll in the plan.
Does Medicare Advantage offer prescription drug coverage?
Medicare Advantage Plans may also offer prescription drug coverage that follows the same rules as Medicare drug plans. Check your Explanation of Benefits (EOB). Your Medicare drug plan will mail you an EOB each month you fill a prescription. This notice gives you a summary of your prescription drug claims and costs.
How to submit Medicare claims electronically?
How to Submit Claims: Claims may be electronically submitted to a Medicare Administrative Contractor (MAC) from a provider using a computer with software that meets electronic filing requirements as established by the HIPAA claim standard and by meeting CMS requirements contained in the provider enrollment & certification category area of this web site and the EDI Enrollment page in this section of the web site. Providers that bill institutional claims are also permitted to submit claims electronically via direct data entry (DDE) screens.
What chapter is Medicare claim processing manual?
For more information please contact your local MAC or refer to the Medicare Claims Processing Manual (IOM Pub.100-04), Chapter 24.
How long does it take for Medicare to process a claim?
Medicare claims to providers take about 30 days to process. The provider usually gets direct payment from Medicare. What is the Medicare Reimbursement fee schedule? The fee schedule is a list of how Medicare is going to pay doctors. The list goes over Medicare’s fee maximums for doctors, ambulance, and more.
What if my doctor doesn't bill Medicare?
If your doctor doesn’t bill Medicare directly, you can file a claim asking Medicare to reimburse you for costs that you had to pay.
What is Medicare reimbursement form?
The Medicare reimbursement form, also known as the “Patient’s Request for Medical Payment, ” is available in both English and Spanish on the Medicare website.
What happens if you see a doctor in your insurance network?
If you see a doctor in your plan’s network, your doctor will handle the claims process. Your doctor will only charge you for deductibles, copayments, or coinsurance. However, the situation is different if you see a doctor who is not in your plan’s network.
Does Medicare cover out of network doctors?
Coverage for out-of-network doctors depends on your Medicare Advantage plan. Many HMO plans do not cover non-emergency out-of-network care, while PPO plans might. If you obtain out of network care, you may have to pay for it up-front and then submit a claim to your insurance company.
Do participating doctors accept Medicare?
Most healthcare doctors are “participating providers” that accept Medicare assignment. They have agreed to accept Medicare’s rates as full payment for their services. If you see a participating doctor, they handle Medicare billing, and you don’t have to file any claim forms.
Do you have to pay for Medicare up front?
But in a few situations, you may have to pay for your care up-front and file a claim asking Medicare to reimburse you. The claims process is simple, but you will need an itemized receipt from your provider.
What is the ASCA requirement for Medicare?
The Administrative Simplification Compliance Act (ASCA) requirement that claims be sent to Medicare electronically as a condition for payment; How you can obtain access to Medicare systems to submit or receive claim or beneficiary eligibility data electronically; and. EDI support furnished by Medicare contractors.
What is EDI in Medicare?
EDI is the automated transfer of data in a specific format following specific data content rules between a health care provider and Medicare, or between Medicare and another health care plan. In some cases, that transfer may take place with the assistance of a clearinghouse or billing service that represents a provider of health care or another payer. EDI transactions are transferred via computer either to or from Medicare. Through use of EDI, both Medicare and health care providers can process transactions faster and at a lower cost.
