
Call the plan you wish to leave and ask for a disenrollment form Call 1-800-MEDICARE (1-800-633-4227) to request that your disenrollment be processed over the phone Call the Social Security Administration or visit your Social Security Office to file your disenrollment request
Full Answer
How do I get Out of my Medicare Advantage plan?
The Disenrollment Period is gone and has been replaced by the OEP. Using your Medicare Advantage trial right is another way to get out of your Medicare Advantage Plan. Basically, if you choose Medicare Advantage during your open enrollment period, you have up to 1 year to “try it out.”
Are Medicare managed care plans right for You?
Medicare managed care plans can provide some relief. Enrolling in the right plan for you is key to making health-care more affordable. The number of Medicare beneficiaries enrolling in managed care plans is on the rise. Instead of working alongside Medicare-like Medigap insurance, Advantage plans replace Original Medicare.
Can I Cancel my Medicare Advantage plan and go back to original?
You can disenroll from or cancel your current Medicare Advantage plan and return to Original Medicare (Medicare Part A and Part B). If you choose to go through Medicare Advantage disenrollment and return to Original Medicare, you also have the option of enrolling in a Prescription Drug Plan (Part D) during this period.
How do I disenroll from my Medicare plan?
1 Call 1-800-MEDICARE (1-800-633-4227). 2 Mail a signed written letter to your plan’s mailing address notifying them of your desire to disenroll. 3 Submit a disenrollment request through the plan’s website (if such a feature is offered). 4 Call your plan and ask a representative to mail you a disenrollment form which you will fill out and return.
Can I switch from a Medicare Advantage plan back to Original Medicare?
Yes, you can elect to switch to traditional Medicare from your Medicare Advantage plan during the Medicare Open Enrollment period, which runs from October 15 to December 7 each year. Your coverage under traditional Medicare will begin January 1 of the following year.
Can you cancel a Medicare Advantage plan at any time?
No, you can't switch Medicare Advantage plans whenever you want. But you do have options if you're unhappy with your plan. You can jump to another plan or drop your Medicare Advantage plan and change to original Medicare during certain times each year.
Can I cancel my Medicare plan?
You can voluntarily terminate your Medicare Part B (medical insurance). It is a serious decision. You must submit Form CMS-1763 (PDF, Download Adobe Reader) to the Social Security Administration (SSA). Visit or call the SSA (1-800-772-1213) to get this form.
What is the difference between managed Medicare and Medicare?
Medicare care managed care plans are an optional coverage choice for people with Medicare. Managed care plans take the place of your original Medicare coverage. Original Medicare is made up of Part A (hospital insurance) and Part B (medical insurance). Plans are offered by private companies overseen by Medicare.
How do I switch back to regular Medicare?
How to switchTo switch to a new Medicare Advantage Plan, simply join the plan you choose during one of the enrollment periods. You'll be disenrolled automatically from your old plan when your new plan's coverage begins.To switch to Original Medicare, contact your current plan, or call us at 1-800-MEDICARE.
Can you switch out of Medicare Advantage?
You're free to leave Medicare Advantage and enroll in certain types of private plans. If your employer or union offers a plan that you find more appealing than Medicare Advantage, you can disenroll without penalty.
How do I disenroll from Medicare as a provider?
Submit the applicable CMS-855 application to voluntarily terminate your Medicare enrollment or to deactivate your reassignment.
What is the penalty for canceling Medicare Part B?
Your Part B premium penalty is 20% of the standard premium, and you'll have to pay this penalty for as long as you have Part B. (Even though you weren't covered a total of 27 months, this included only 2 full 12-month periods.) Find out what Part B covers.
How do I opt out of Medicare Part B?
To disenroll, you're required to submit a form (CMS-1763) that must be completed either during a personal interview at a Social Security office or on the phone with a Social Security representative. For an interview, call the Social Security Administration at 1-800-772-1213, or your local office.
What is Medicare Fee for Service vs managed care?
Under the FFS model, the state pays providers directly for each covered service received by a Medicaid beneficiary. Under managed care, the state pays a fee to a managed care plan for each person enrolled in the plan.
What is the biggest disadvantage of Medicare Advantage?
Medicare Advantage can become expensive if you're sick, due to uncovered copays. Additionally, a plan may offer only a limited network of doctors, which can interfere with a patient's choice. It's not easy to change to another plan. If you decide to switch to a Medigap policy, there often are lifetime penalties.
Is Medicare Advantage cheaper than original Medicare?
The costs of providing benefits to enrollees in private Medicare Advantage (MA) plans are slightly less, on average, than what traditional Medicare spends per beneficiary in the same county. However, MA plans that are able to keep their costs comparatively low are concentrated in a fairly small number of U.S. counties.
What are the benefits of Medicare managed care?
Benefits can include routine vision, dental and hearing services. Additionally, managed care plans offer prescription drug coverage. The cost of medications out-of-pocket can be financially exhausting. Medicare managed care plans can provide some relief.
What is managed care plan?
Managed-care plans or Advantage plans bundles all health-care coverage under one neat plan. MA plans decide on rate amounts, making prices different from plan to plan. Processing payments are done through the private plan, not Medicare.
What is Medicare Advantage 2021?
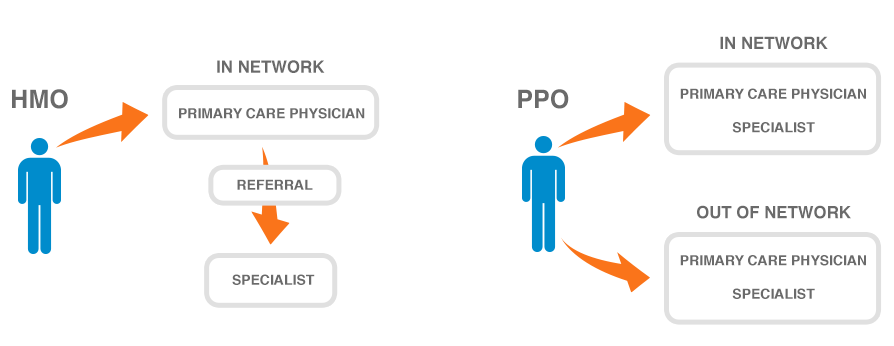
Updated on March 19, 2021. Medicare managed care plans are an alternative to Original Medicare. Otherwise known as Medicare Advantage plans with many plan types, most are either HMOs or PPOs. Managed-care plans provide benefits for gaps in Parts A and B coverage. These alternative health-care plans make up Part C of Medicare.
Why is it important to enroll in the right plan?
Enrolling in the right plan for you is key to making health-care more affordable. The number of Medicare beneficiaries enrolling in managed care plans is on the rise. Instead of working alongside Medicare-like Medigap insurance, Advantage plans replace Original Medicare. While providing additional benefits, these plans must also include all ...
Does an indemnity plan have a provider network?
Members will receive reimbursement for medical expenses (up to a certain amount). Indemnity plans have no provider network, members can visit the doctor (s) of their choice. Contrarily, managed care plans have a network (s) of providers, with different plan options.
Does managed care plan limit doctors?
On the other hand, managed care plans may limit beneficiaries to only the doctors within the plan’s network. If having the freedom to see any healthcare provider of choice is important, remember that Advantage plans limit provider options. While traveling within the country, managed care pays for emergency services only.
Is Medicare Supplement the same as Managed Care?
Managed-care plans and Medicare Supplement plans are not the same. This misconception is common. Both provide additional benefits to Original Medicare. However, they serve two totally different purposes. Managed-care plans or Advantage plans bundles all health-care coverage under one neat plan.
How to change Medicare Advantage plan?
During the Medicare Advantage Open Enrollment Period, you can change your Medicare plans in the following ways: 1 You can switch from your current Medicare Advantage plan (Medicare Part C) to another Medicare Advantage plan, whether or not either plan offers prescription drug coverage. 2 You can disenroll from or cancel your current Medicare Advantage plan and return to Original Medicare (Medicare Part A and Part B). 3 If you choose to go through Medicare Advantage disenrollment and return to Original Medicare, you also have the option of enrolling in a Prescription Drug Plan (Part D) during this period.
How to disenroll from Medicare Part D?
There are four ways in which you may disenroll from Medicare Part D during this time: Call 1-800-MEDICARE (1-800-633-4227). Mail a signed written letter to your plan’s mailing address notifying them of your desire to disenroll. Submit a disenrollment request through the plan’s website (if such a feature is offered).
How to disenroll from Part B?
If you do not initially disenroll in Part B, you will have to do so by contacting your local Social Security office or calling 1-800-772-1213 (TTY 1-800-325-0778). You may not disenroll from Part B online. You will have to speak directly to a Social Security agent to complete the process.
When is the disenrollment period for Medicare?
The time to disenroll from a Medicare Prescription Drug Plan (or to switch to a different drug plan) is during the yearly fall Medicare Open Enrollment Period for Medicare Advantage and prescription drug plans, which – as mentioned above – takes place from October 15 to December 7.
When is Medicare open enrollment?
Medicare Advantage Open Enrollment Period. Starting in 2019, the Medicare Advantage Open Enrollment Period takes place from January 1 to March 31. During the Medicare Advantage Open Enrollment Period, you can change your Medicare plans in the following ways: You can switch from your current Medicare Advantage plan (Medicare Part C) ...
When is the fall enrollment period?
Fall Open Enrollment Period, also called the Annual Enrollment Period or Annual Election Period (AEP) The Fall Open Enrollment Period, also called the Annual Enrollment Period (AEP) takes place from October 15 to December 7 each year. During AEP, you can change your Medicare plans in the following ways: You may disenroll from one Medicare Advantage ...
What's New
December 2019: The Parts C and D Enrollee Grievance, Organization/Coverage Determinations and Appeals Guidance has been updated to include recent regulatory changes and will be effective January 1, 2020. Questions related to the guidance or appeals policy may be submitted to the Division of Appeals Policy at https://appeals.lmi.org.
Overview
Medicare health plans, which include Medicare Advantage (MA) plans (such as Health Maintenance Organizations, Preferred Provider Organizations, Medical Savings Account plans and Private Fee-For-Service plans) Cost Plans and Health Care Prepayment Plans, must meet the requirements for grievance, organization determination, and appeals processing under the MA regulations found at 42 CFR Part 422, Subpart M.
Web Based Training Course Available for Part C
The course covers requirements for Part C organization determinations, appeals, and grievances. Complete details can be accessed on the "Training" page, using the link on the left navigation menu on this page.
When is the MA model enrollment period?
All enrollments with an effective date on or after January 1, 2021, must be processed in accordance with the revised guidance requirements, including the new model MA enrollment form. MA plans are expected to use the new model form for the 2021 plan year Annual Enrollment Period (AEP) which begins on October 15, 2020.
When does MA default enrollment start?
As outlined in the 2019 guidance, only MA organizations who meet the criteria outlined and are approved by CMS to conduct default enrollment for coverage effective dates of January 1, 2019 , or later.
When does Medicare kick in?
If you make a change during the Medicare Advantage Open Enrollment Period, your new Medicare benefits will kick in on the first day of the month following your enrollment. For example, if you make a change to your Medicare Advantage plan at any point during the month of January, your new coverage will take effect on February 1.
When does Medicare open enrollment end?
Any changes that you make will take effect on January 1 of the following year. Medicare Advantage Open Enrollment Period. This open enrollment period applies to recipients who are currently using a Medicare Advantage plan. This period lasts from January 1 to March 31 each year, and during this time, you can make one change to your healthcare ...
When is the Medicare election period?
Annual Election Period. From October 15 to December 7 each year is the Annual Election Period. This period is also referred to as the Annual Enrollment Period. During this time, you can elect to make changes to your Medicare coverage.
What is Medicare managed care?
Medicare care managed care plans are an optional coverage choice for people with Medicare. Managed care plans take the place of your original Medicare coverage. Original Medicare is made up of Part A (hospital insurance) and Part B (medical insurance). Plans are offered by private companies overseen by Medicare.
What is a Medigap plan?
A Medigap plan, also known as Medicare supplement insurance, is optional coverage you can add to original Medicare to help cover out-of-pocket costs. Medigap plans can help you pay for things like: coinsurance costs. copayments. deductibles. These aren’t a type of managed care plan.
What is Medicare Advantage?
Sometimes referred to as Medicare Part C or Medicare Advantage, Medicare managed care plans are offered by private companies. These companies have a contract with Medicare and need to follow set rules and regulations. For example, plans must cover all the same services as original Medicare.
How much does Medicare cost in 2021?
Most people receive Part A without paying a premium, but the standard Part B premium in 2021 is $148.50. The cost of your managed care plan will be on top of that $148.50.
What is a SNP?
Special Needs Plan (SNP). An SNP is a managed care plan designed with a specific population in mind. SNPs offer additional coverage beyond a standard plan. There are SNPs for people with limited incomes, who are managing certain conditions, or who live in long-term care facilities.
What is a poor performer health plan?
you live in a “disaster area,” as declared by the Federal Emergency Management Agency (FEMA) — for example, if your area has been struck by a hurricane or other natural disaster. your current health plan is a “poor performer,” according to Medicare.
Does Medicare Part A cover managed care?
When you have a managed care plan, all your costs will be included. You don’t need to know whether Part A or Part B cover a service because your managed care plan will cover all the same things.
