
Medicare is always primary if it’s your only form of coverage. When you introduce another form of coverage into the picture, there’s predetermined coordination of benefits. The coordination of benefits will determine what form of coverage is primary and what form of coverage is secondary. The primary coverage will pay first, and the secondary coverage pays second.
Is Medicare always your primary insurance?
Oct 19, 2021 · Medicare is always primary if it’s your only form of coverage. When you introduce another form of coverage into the picture, there’s predetermined coordination of benefits. The coordination of benefits will determine what form of coverage is primary and what form of coverage is secondary. The primary coverage will pay first, and the secondary coverage pays …
How to make Medicare the primary insurance?
The “primary payer” pays what it owes on your bills first and sends the remaining amount to the second or “secondary payer.” There may also be a third payer in some cases. 1 Important facts to know include: The primary payer pays up to the limits of its coverage. The secondary payer only pays if there are costs the first payer didn’t cover.
When does Medicare pay secondary?
Sep 09, 2020 · This article includes a quick reference table that will help the billing staff of providers, physicians, and other suppliers determine whether Medicare is the primary or secondary payer based upon specific situational criteria. The information included within the table is based upon the “Medicare Secondary Payer Fact Sheet” published by the Centers for …
How does Medicare work as a secondary payer?
Dec 01, 2021 · Medicare pays Primary, GHP pays secondary Individual is age 65 or older, is covered by a GHP through current employment or spouse’s current employment AND the employer has 20 or more employees (or at least one employer is a multi-employer group that employs 20 or more individuals): GHP pays Primary, Medicare pays secondary
How do I know if my Medicare is primary?
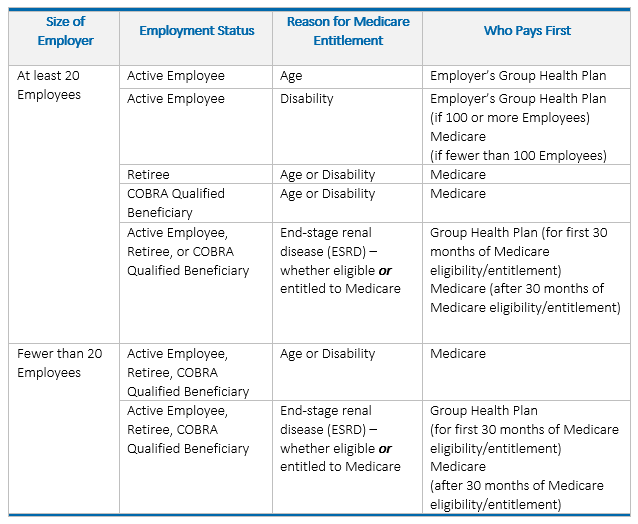
If the employer has 100 or more employees, then your family member's group health plan pays first, and Medicare pays second. If the employer has less than 100 employees, but is part of a multi-employer or multiple employer group health plan, your family member's group health plan pays first and Medicare pays second.
How do I know if my Medicare is secondary?
If you're under 65, eligible for Medicare due to a disability, and have group employer coverage through an employer with more than 100 employees, Medicare will be your secondary payer.
How do you determine which insurance is primary and which is secondary?
The insurance that pays first is called the primary payer. The primary payer pays up to the limits of its coverage. The insurance that pays second is called the secondary payer. The secondary payer only pays if there are costs the primary insurer didn't cover.Dec 1, 2021
When Medicare is the secondary payer?
Medicare may be the secondary payer when: a person has a GHP through their own or a spouse's employment, and the employer has more than 20 employees. a person is disabled and covered by a GHP through an employer with more than 100 employees.Oct 29, 2020
Is Medicare Part B primary or secondary?
Your group insurance plan is the secondary insurer, so you should enroll in Medicare Part B before your group plan will pay its portion of the claim.
How do you know which insurance is primary?
Primary insurance is a health insurance plan that covers a person as an employee, subscriber, or member. Primary insurance is billed first when you receive health care. For example, health insurance you receive through your employer is typically your primary insurance.Oct 8, 2019
When two insurance which one is primary?
If you have two plans, your primary insurance is your main insurance. Except for company retirees on Medicare, the health insurance you receive through your employer is typically considered your primary health insurance plan.
Can you have 2 primary insurances?
Yes, individuals can have coverage under two different health insurance plans. When two health insurance plan providers work together to pay the claims of one person, it's called coordination of benefits. The following situations are reasons employees would have dual insurance coverage: The employee is married.Feb 5, 2021
Is it illegal to have two health insurance policies?
Policyholders can have any number of health insurance plans. However, they cannot claim reimbursement for the same expense from multiple insurers. If one cover is not sufficient, the other cover can be used to cover the expenses. Health Insurance is of utmost importance for every individual.
How do I submit a Medicare claim as a secondary?
Medicare Secondary Payer (MSP) claims can be submitted electronically to Novitas Solutions via your billing service/clearinghouse, directly through a Secure File Transfer Protocol (SFTP) connection, or via Novitasphere portal's batch claim submission.Sep 9, 2021
Does Medicare Secondary cover primary copays?
Medicare is often the primary payer when working with other insurance plans. A primary payer is the insurer that pays a healthcare bill first. A secondary payer covers remaining costs, such as coinsurances or copayments.
Does Medicare as Secondary cover copays?
Usually, secondary insurance pays some or all of the costs left after the primary insurer has paid (e.g., deductibles, copayments, coinsurances). For example, if Original Medicare is your primary insurance, your secondary insurance may pay for some or all of the 20% coinsurance for Part B-covered services.
What is the difference between Medicare and Medicaid?
Eligible for Medicare. Medicare. Medicaid ( payer of last resort) 1 Liability insurance only pays on liability-related medical claims. 2 VA benefits and Medicare do not work together. Medicare does not pay for any care provided at a VA facility, and VA benefits typically do not work outside VA facilities.
Is Medicare a secondary insurance?
When you have Medicare and another type of insurance, Medicare is either your primary or secondary insurer. Use the table below to learn how Medicare coordinates with other insurances. Go Back. Type of Insurance. Conditions.
What does primary and secondary payer mean?
Each type of coverage you have is called a “payer.” When you have more than one payer, there are rules to decide who pays first, called the coordination of benefits. The “primary payer” pays what it owes on your bills first and sends the remaining amount to the second or “secondary payer.” There may also be a third payer in some cases. 1
When is Medicare primary or secondary?
A number of things can affect when Medicare pays first. The following chart explains some common scenarios. 3 For information on several other scenarios, check out how Medicare works with other insurance#N#, opens new window#N#.
How does Medicare know if I have other coverage?
Medicare doesn’t automatically know if you have other coverage. But your insurers must report to Medicare when they’re the primary payer on your medical claims.
Where to get more details
If you have additional questions about who pays your Medicare bills first, contact your insurance provider or call Medicare’s Benefits Coordination & Recovery Center (BCRC) at 855-798-2627 (TTY: 855-797-2627).
How can we help?
Licensed Humana sales agents are available Monday - Friday, 8 a.m. to 8 p.m., local time.
What is the age limit for a GHP?
Is age 65 or older, and is covered by a group health plan (GHP) through current employment or spouse’s current employment…. The employer has fewer than 20 employees…. Is age 65 or older, and is covered by a GHP through current employment or spouse’s current employment….
Is Medicare a cobra?
Medicare. Is age 65 or older OR is disabled and covered by Medicare and COBRA…. The patient is entitled to Medicare…. Medicare. COBRA. First Coast Service Options (First Coast) strives to ensure that the information available on our provider website is accurate, detailed, and current.
What is Medicare Secondary Payer?
Medicare Secondary Payer (MSP) is the term generally used when the Medicare program does not have primary payment responsibility - that is, when another entity has the responsibility for paying before Medicare. When Medicare began in 1966, it was the primary payer for all claims except for those covered by Workers' Compensation, ...
What age is Medicare?
Retiree Health Plans. Individual is age 65 or older and has an employer retirement plan: Medicare pays Primary, Retiree coverage pays secondary. 6. No-fault Insurance and Liability Insurance. Individual is entitled to Medicare and was in an accident or other situation where no-fault or liability insurance is involved.
Why is Medicare conditional?
Medicare makes this conditional payment so that the beneficiary won’t have to use his own money to pay the bill. The payment is “conditional” because it must be repaid to Medicare when a settlement, judgment, award or other payment is made. Federal law takes precedence over state laws and private contracts.
How long does ESRD last on Medicare?
Individual has ESRD, is covered by a GHP and is in the first 30 months of eligibility or entitlement to Medicare. GHP pays Primary, Medicare pays secondary during 30-month coordination period for ESRD.
When did Medicare start?
When Medicare began in 1966 , it was the primary payer for all claims except for those covered by Workers' Compensation, Federal Black Lung benefits, and Veteran’s Administration (VA) benefits.
What is the purpose of MSP?
The MSP provisions have protected Medicare Trust Funds by ensuring that Medicare does not pay for items and services that certain health insurance or coverage is primarily responsible for paying. The MSP provisions apply to situations when Medicare is not the beneficiary’s primary health insurance coverage.
What is conditional payment?
A conditional payment is a payment Medicare makes for services another payer may be responsible for.
What is primary insurance?
Primary insurance means that it pays first for any healthcare services you receive. In most cases, the secondary insurance won’t pay unless the primary insurance has first paid its share. There are a number of situations when Medicare is primary.
When does Medicare end for ESRD?
You would then re-enroll when you turn 65. Typically Medicare due to ESRD will end 36 months after you’ve had your kidney transplant unless you also qualify for Medicare due to age or other disability.
What is tricare for life?
You Have Tricare-for-Life. Tricare-for-Life (TFL) is for military retirees and their spouses who are also eligible for Medicare. In this scenario, Medicare is the primary insurance for any care you receive at non-military providers, so you need to enroll in both Part A and B.
Does Tricare cover vision?
People with Tricare sometimes also choose Medicare Advantage plans. Some Advantage plans include routine dental or vision benefits, and this may appeal to members with Tricare. Tricare for life will help to pick up some of the copays associated with Medicare Advantage.
Does medicaid pay first?
Medicaid is assistance with healthcare costs for people with low incomes. Medicaid never pays first. It will only pay after Medicare and or employer group health coverage has first paid. Not all Medicare providers accept Medicaid though. It’s important that you ask providers if they participate in Medicaid before seeking care. Otherwise, you may be responsible for the portions that Medicaid can’t cover.
Is Medicare a part of Medicaid?
Medicare is primary to Medicaid. People who qualify for Medicaid can get help paying for their Medicare Part B and D premiums. If your income is low and you think you might be eligible, contact your state Medicaid office for an application. To learn more about Medicare vs Medicaid, click here.
Is Medicare a secondary insurance?
Medicare is secondary to your group health insurance if the company has 20 or more employees. If the group insurance is affordable, you may choose to delay your enrollment in Part B. ALWAYS speak with a licensed insurance agent who specializes in Medicare before making this decision.
What is the difference between primary and secondary insurance?
The insurance that pays first (primary payer) pays up to the limits of its coverage. The one that pays second (secondary payer) only pays if there are costs the primary insurer didn't cover. The secondary payer (which may be Medicare) may not pay all the uncovered costs.
How does Medicare work with other insurance?
When there's more than one payer, "coordination of benefits" rules decide which one pays first. The "primary payer" pays what it owes on your bills first, and then sends the rest to the "secondary payer" (supplemental payer) ...
When does Medicare pay for COBRA?
When you’re eligible for or entitled to Medicare due to End-Stage Renal Disease (ESRD), during a coordination period of up to 30 months, COBRA pays first. Medicare pays second, to the extent COBRA coverage overlaps the first 30 months of Medicare eligibility or entitlement based on ESRD.
What is a group health plan?
If the. group health plan. In general, a health plan offered by an employer or employee organization that provides health coverage to employees and their families.
How long does it take for Medicare to pay a claim?
If the insurance company doesn't pay the claim promptly (usually within 120 days), your doctor or other provider may bill Medicare. Medicare may make a conditional payment to pay the bill, and then later recover any payments the primary payer should have made. If Medicare makes a. conditional payment.
What happens if a group health plan doesn't pay?
If the group health plan didn’t pay all of your bill, the doctor or health care provider should send the bill to Medicare for secondary payment. Medicare may pay based on what the group health plan paid, what the group health plan allowed, and what the doctor or health care provider charged on the claim.
What is a copayment?
A copayment is usually a set amount, rather than a percentage. For example, you might pay $10 or $20 for a doctor's visit or prescription drug. or a. deductible. The amount you must pay for health care or prescriptions before Original Medicare, your prescription drug plan, or your other insurance begins to pay.
What is secondary insurance?
Secondary insurance. The secondary health insurance payer covers bills that the primary insurance payer didn’t cover. However, it is crucial to remember that the secondary insurance company may not pay all of the rest of your bills. You may be responsible for some health care costs.
What happens if you have two health insurance plans?
If you carry two health insurance plans and have deductibles with each plan, you’re responsible for paying both of them when you make a claim. In other words, don’t expect that if you pay a deductible on one plan, it will eliminate your obligation for the deductible on the other plan.
What is the process of coordinating health insurance?
That way, both health plans pay their fair share without paying more than 100% of the medical costs. This process is called coordination of benefits.
How does COB work?
Here’s how COB works when there’s a health insurance claim: It first goes to the primary plan. The insurer pays what it owes. If there’s money still left on the bill, it then goes to the secondary insurer, which picks up what it owes.
Who pays the medical bill?
The primary insurance payer is the insurance company responsible for paying the claim first. When you receive health care services, the primary payer pays your medical bills up to the coverage limits. The secondary payer then reviews the remaining bill and picks up its portion.
Is Medicare considered primary?
Medicare and a private health plan – Typically, Medicare is considered primary if the worker is 65 or older and his or her employer has less than 20 employees. A private insurer is primary if the employer has 20 or more employees.
Can a child stay on their parents' health insurance?
A child under 26 - The Affordable Care Act lets children stay on their parents’ health plan until they turn 26. That could result in a child having her own health plan through an employer while remaining on the family’s plan. In that case, the child’s health plan is primary and the parents’ plan is secondary.
