Get care from a home health agency (HHA) that contracts with your plan Request prior authorization or a referral before receiving home health care Pay a copayment for your care (Original Medicare fully covers home health)
Full Answer
How much does Medicare pay for home health care?
Your costs in Original Medicare $0 for home health care services. 20% of the Medicare-approved amount for Durable Medical Equipment (DME). Before you start getting your home health care, the home health agency should tell you how much Medicare will pay.
Does Medicare pay for part time home health aide services?
According to Medicare.gov, Medicare does pay for “part-time or intermittent home health aide services.” This is understandably confusing. It means that a home health worker may provide personal care services that a home health aide provides. The difference is that, for reimbursement, you must be getting skilled nursing services as well.
Do I qualify for home health care if I have Medicare?
If you need more than “intermittent” skilled nursing care, you don’t qualify for home health services. To determine if you’re eligible for home health care, Medicare defines “intermittent” as skilled nursing care that’s needed: Fewer than 7 days each week.
How do I get home health care services?
Get care from a home health agency (HHA) that contracts with your plan Request prior authorization or a referral before receiving home health care Know that HHAs can choose who to accept as a patient or refuse to provide you with home health services if they do not believe they can ensure your safety.
Does Medicare pay for home assistant?
Home health aide: Medicare pays in full for an aide if you require skilled care (skilled nursing or therapy services). A home health aide provides personal care services, including help with bathing, toileting, and dressing.
What will Medicare not pay for?
In general, Original Medicare does not cover: Long-term care (such as extended nursing home stays or custodial care) Hearing aids. Most vision care, notably eyeglasses and contacts. Most dental care, notably dentures.
What is the methodology through which Medicare reimbursement for home health services is paid?
Patient Driven Groupings Model (PDGM)As of January 1, 2020, Medicare pays for home health services via a value-based payment model known as the Patient Driven Groupings Model (PDGM).
What percentage does Medicare cover?
Medicare Part B pays 80% of the cost for most outpatient care and services, and you pay 20%. For 2022, the standard monthly Part B premium is $170.10.
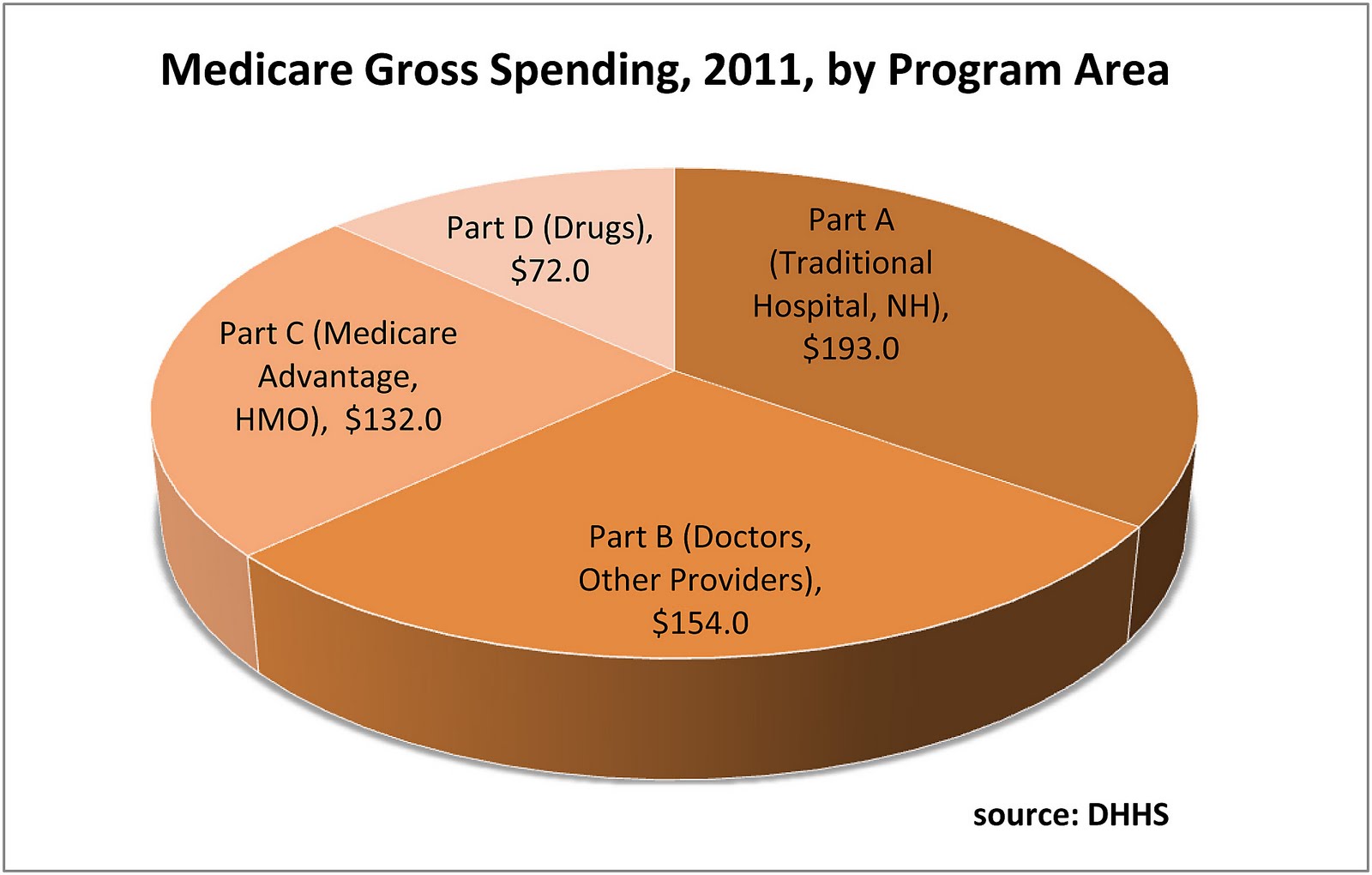
What are the 4 types of Medicare?
There are four parts of Medicare: Part A, Part B, Part C, and Part D.Part A provides inpatient/hospital coverage.Part B provides outpatient/medical coverage.Part C offers an alternate way to receive your Medicare benefits (see below for more information).Part D provides prescription drug coverage.
How Much Does Medicare pay for home health care per hour?
Medicare will cover 100% of the costs for medically necessary home health care provided for less than eight hours a day and a total of 28 hours per week. The average cost of home health care as of 2019 was $21 per hour.
How Long Will Medicare pay for home health care?
Medicare pays your Medicare-certified home health agency one payment for the covered services you get during a 30-day period of care. You can have more than one 30-day period of care. Payment for each 30-day period is based on your condition and care needs.
How much does 24/7 in home care cost per month?
But sometimes, an elderly adult needs hands-on assistance all day and night. So, how much does 24/7 in-home care cost? The average cost of 24/7 care at home stacks up to around $15,000 a month, whether that's 24-hour companion care or home health care.
How to qualify for home health care?
Ideally, home health can enhance your care and prevent re-admission to a hospital. There are several steps and conditions to qualify for home health care: 1 You must be under the care of a doctor who has created a plan for you that involves home health care. Your doctor must review the plan at regular intervals to make sure it is still helping you. 2 Your doctor must certify that you need skilled nursing care and therapy services. To need this care, your doctor must decide that your condition will improve or maintain through home health services. 3 Your doctor must certify that you are homebound. This means it is very difficult or medically challenging for you to leave your home.
What is home health aide?
Home health aides are health professionals who help people in their home when they have disabilities, chronic illnesses, or need extra help. Aides may help with activities of daily living, such as bathing, dressing, going to the bathroom, or other around-the-home activities. For those who need assistance at home, home health aides can be invaluable.
What is the difference between home health and skilled nursing?
The difference is that, for reimbursement, you must be getting skilled nursing services as well.
What is Medicare Part A?
Medicare Part A is the portion that provides hospital coverage. Medicare Part A is free to most individuals when they or their spouse worked for at least 40 quarters paying Medicare taxes.
What education do you need to be a home health aide?
According to the U.S. Bureau of Labor Statistics, the typical educational level for a home health aide is a high school diploma or equivalent. Some people may use the term “home health aide” to describe all occupations that provide care at home, but a home health aide is technically different from a home health nurse or therapist.
Who must review home health care plans?
You must be under the care of a doctor who has created a plan for you that involves home health care. Your doctor must review the plan at regular intervals to make sure it is still helping you. Your doctor must certify that you need skilled nursing care and therapy services.
Is long term care insurance part of Medicare?
Some people choose to purchase separate long-term care insurance, which isn’t a part of Medicare . These policies may help to cover more home health care services and for longer time periods than Medicare. However, the policies vary and do represent an extra cost to seniors.
How do I contact Medicare for home health?
If you have questions about your Medicare home health care benefits or coverage and you have Original Medicare, visit Medicare.gov, or call 1-800-MEDICARE (1-800-633-4227) . TTY users can call 1-877-486-2048. If you get your Medicare benefits through a Medicare Advantage Plan (Part C) or other
What happens when home health services end?
When all of your covered home health services are ending, you may have the right to a fast appeal if you think these services are ending too soon. During a fast appeal, an independent reviewer called a Beneficiary and Family Centered Care Quality Improvement Organization (BFCC-QIO) looks at your case and decides if you need your home health services to continue.
What is an appeal in Medicare?
Appeal—An appeal is the action you can take if you disagree with a coverage or payment decision made by Medicare, your Medicare health plan, or your Medicare Prescription Drug Plan. You can appeal if Medicare or your plan denies one of these:
Why is home health important?
In general, the goal of home health care is to provide treatment for an illness or injury. Where possible, home health care helps you get better, regain your independence, and become as self-sucient as possible. Home health care may also help you maintain your current condition or level of function, or to slow decline.
Can Medicare take home health?
In general, most Medicare-certified home health agencies will accept all people with Medicare . An agency isn’t required to accept you if it can’t meet your medical needs. An agency shouldn’t refuse to take you because of your condition, unless the agency would also refuse to take other people with the same condition.
What is home health agency?
The home health agency will be responsible for all of your medical, nursing, and rehabilitative care and will communicate your needs to the managing physician. Your condition will be monitored and assessed regularly and will create discharge plans when appropriate.
What can a registered nurse do for home care?
A registered nurse or licensed practical nurse may administer your home care which may include giving IV drugs, changing wound dressings, tube feedings, teaching about diabetes care, or certain injections. The home health aides must work for a Medicare-approved home health agency and your doctor must certify that you are homebound.
Is home health care as effective as inpatient care?
Most patients would prefer to receive care for an illness or injury in the comfort of their own home. Fortunately, home health care can be as effective as inpatient care in a hospital or skilled nursing facility. Studies on healing at home have shown improved outcomes and quicker recoveries for patients. Home health care can be less costly ...
Does Medicare cover home health care?
Home health care can be less costly than a long hospital stay and Medicare can help cover the costs. If your physician orders reasonable and medically necessary treatment of an illness or injury, Medicare will help pay for home health services as long as you meet certain criteria.
Do home health aides have to be Medicare approved?
The home health aides must work for a Medicare-approved home health agency and your doctor must certify that you are homebound. These agencies agree to be paid the Medicare-approved amount and to be paid directly by Medicare. The home health agency will be responsible for all of your medical, nursing, and rehabilitative care ...
Does Medicare Part B cover out of pocket costs?
The Medicare Part B deductible will apply. Many Medicare recipients choose to purchase supplemental insurance to help cover the out-of-pocket costs from Part A and Part B. If you have enrolled in a Medigap plan, it may help pay for deductibles and coinsurance associated with home health care.
When will HHAs get paid?
30-Day Periods of Care under the PDGM. Beginning on January 1 2020, HHAs are paid a national, standardized 30-day period payment rate if a period of care meets a certain threshold of home health visits. This payment rate is adjusted for case-mix and geographic differences in wages. 30-day periods of care that do not meet ...
When did the Home Health PPS rule become effective?
Effective October 1, 2000, the home health PPS (HH PPS) replaced the IPS for all home health agencies (HHAs). The PPS proposed rule was published on October 28, 1999, with a 60-day public comment period, and the final rule was published on July 3, 2000. Beginning in October 2000, HHAs were paid under the HH PPS for 60-day episodes ...
Is telecommunications technology included in a home health plan?
In response CMS amended § 409.43 (a), allowing the use of telecommunications technology to be included as part of the home health plan of care, as long as the use of such technology does not substitute for an in-person visit ordered on the plan of care.
What to do if you have no HHA?
If no HHA in your area can provide you with care, speak to your doctor about other options for receiving care. If you need information about the costs and coverage rules for home health care, or if you are experiencing problems, contact your Medicare Advantage Plan.
Does Medicare Advantage cover home health?
All Medicare Advantage Plans must provide at least the same level of home health care coverage as Original Medicare, but they may impose different rules, restrictions, and costs. Depending on your plan, you may need to: Get care from a home health agency (HHA) that contracts with your plan.
