
Proper coding is necessary on Medicare claims because codes are generally used in determining coverage and payment amounts. CMS
Centers for Medicare and Medicaid Services
The Centers for Medicare & Medicaid Services, previously known as the Health Care Financing Administration, is a federal agency within the United States Department of Health and Human Services that administers the Medicare program and works in partnership with state government…
Full Answer
What types of codes are included in a billing and coding article?
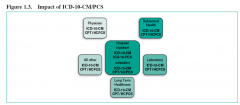
Billing and Coding articles typically include CPT/HCPCS procedure codes, ICD-10-CM diagnosis codes, as well as Bill Type, Revenue, and CPT/HCPCS Modifier codes.
What information do I need to bill for Medicare?
When billing for traditional Medicare (Parts A and B), billers will follow the same protocol as for private, third-party payers, and input patient information, NPI numbers, procedure codes, diagnosis codes, price, and Place of Service codes.
What are the billing responsibilities of a Medicare provider?
Your Billing Responsibilities For Medicare programs to work effectively, providers have a significant responsibility for the collection and maintenance of patient information. They must ask questions to secure employment and insurance information.
What are the requirements for billing and billing for diagnostic tests?
The billing physician or other supplier must keep on file the name, the National Provider Identifier, and address of the performing physician. The physician or other supplier furnishing the technical component or professional component of the diagnostic test must be enrolled in the Medicare program. No formal reassignment is necessary.
What is required to bill Medicare?
In summary, a provider, whether participating or nonparticipating in Medicare, is required to bill Medicare for all covered services provided. If the provider has reason to believe that a covered service may be excluded because it may be found not to be reasonable and necessary the patient should be provided an ABN.
Does Medicare require G-codes?
Note: Due to CY 2019 Physician Fee Schedule (PFS) rulemaking, effective for dates of service on or after January 1, 2019, Medicare no longer requires the functional reporting of nonpayable HCPCS G-codes and severity modifiers − adopted to implement section 3005(g) of MCTRJCA − on claims for therapy services.
Are G-codes required for Medicare in 2021?
The Centers for Medicare & Medicaid Services (CMS) has finalized its new add-on code for visit complexity, which should be a financial boon to primary care doctors. All family physicians should be aware of the code, G2211, and use it appropriately on a frequent basis starting in 2021.
Should I use GT or 95 modifier?
A GT modifier is an older coding modifier that serves a similar purpose as the 95 modifier. CMS recommends 95, different companies have varying standards for which codes to be billed. It is a good idea to check with the plans before billing.
Does CPT code G0439 need a modifier?
Along with code G0438 or G0439, CPT code modifier -25 must be appended to the medically necessary E&M service. CPT guidelines define the -25 modifier as "Significant, separately identifiable evaluation and management (E/M) service by the same physician on the same day of the procedure or other service."
What is G0463 used for?
HCPCS Code G0463 is used for all FACILITY evaluation and management visits, regardless of the intensity of service provided.
When should G codes be used?
G-codes are used to report a beneficiary's functional limitation being treated and note whether the report is on the beneficiary's current status, projected goal status, or discharge status.
What are G HCPCS codes used for?
G codes are national codes assigned by CMS to identify professional healthcare procedures and services that may not have assigned CPT® codes.
What is the reimbursement rate for 99441?
Coding claims during COVID-19 Telehealth CPT codes 99441 (5-10 minutes), 99442 (11-20 minutes), and 99443 (20-30 minutes) Reimbursements match similar in-person services, increasing from about $14-$41 to about $60-$137, retroactive to March 1, 2020.
Does Medicare use GT or 95 modifier?
Some insurance companies, such as Medicare, also accept modifier 95, which means that the visit was a synchronous telehealth service administered via real-time interactive audio and video telecommunications system.
Does Medicare require GT modifier?
Does Medicare Accept GT? No. The CMS standards changed in the beginning of 2018, when they replaced GT with 95. Medicaid also requires 95.
What is GT and GQ modifier?
The two primary modifiers for telehealth services were GT (indicating the service was delivered via an interactive audio and video telecommunications system) and GQ (indicating the service was delivered via an asynchronous telecommunications system).
What form do you need to bill Medicare?
If a biller has to use manual forms to bill Medicare, a few complications can arise. For instance, billing for Part A requires a UB-04 form (which is also known as a CMS-1450). Part B, on the other hand, requires a CMS-1500. For the most part, however, billers will enter the proper information into a software program and then use ...
What is 3.06 Medicare?
3.06: Medicare, Medicaid and Billing. Like billing to a private third-party payer, billers must send claims to Medicare and Medicaid. These claims are very similar to the claims you’d send to a private third-party payer, with a few notable exceptions.
What is a medical biller?
In general, the medical biller creates claims like they would for Part A or B of Medicare or for a private, third-party payer. The claim must contain the proper information about the place of service, the NPI, the procedures performed and the diagnoses listed. The claim must also, of course, list the price of the procedures.
How long does it take for Medicare to process a claim?
The MAC evaluates (or adjudicates) each claim sent to Medicare, and processes the claim. This process usually takes around 30 days .
Is it harder to bill for medicaid or Medicare?
Billing for Medicaid. Creating claims for Medicaid can be even more difficult than creating claims for Medicare. Because Medicaid varies state-by-state, so do its regulations and billing requirements. As such, the claim forms and formats the biller must use will change by state. It’s up to the biller to check with their state’s Medicaid program ...
Can you bill Medicare for a patient with Part C?
Because Part C is actually a private insurance plan paid for, in part, by the federal government, billers are not allowed to bill Medicare for services delivered to a patient who has Part C coverage. Only those providers who are licensed to bill for Part D may bill Medicare for vaccines or prescription drugs provided under Part D.
Do you have to go through a clearinghouse for Medicare and Medicaid?
Since these two government programs are high-volume payers, billers send claims directly to Medicare and Medicaid. That means billers do not need to go through a clearinghouse for these claims, and it also means that the onus for “clean” claims is on the biller.
When do hospitals report Medicare beneficiaries?
If the beneficiary is a dependent under his/her spouse's group health insurance and the spouse retired prior to the beneficiary's Medicare Part A entitlement date, hospitals report the beneficiary's Medicare entitlement date as his/her retirement date.
Does Medicare pay for the same services as the VA?
Veteran’s Administration (VA) Benefits - Medicare does not pay for the same services covered by VA benefits.
Does Medicare pay for black lung?
Federal Black Lung Benefits - Medicare does not pay for services covered under the Federal Black Lung Program. However, if a Medicare-eligible patient has an illness or injury not related to black lung, the patient may submit a claim to Medicare. For further information, contact the Federal Black Lung Program at 1-800-638-7072.
Is Medicare a primary or secondary payer?
Providers must determine if Medicare is the primary or secondary payer; therefore, the beneficiary must be queried about other possible coverage that may be primary to Medicare. Failure to maintain a system of identifying other payers is viewed as a violation of the provider agreement with Medicare.
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
Article Guidance
The billing and coding information in this article is dependent on the coverage indications, limitations and/or medical necessity described in the associated LCD L35490 Category III Codes with the exception of the following CPT codes:
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
Language quoted from Centers for Medicare and Medicaid Services (CMS), National Coverage Determinations (NCDs) and coverage provisions in interpretive manuals is italicized throughout the policy.
Article Guidance
The Medicare Administrative Contractor has determined in review of submitted claims that there is inappropriate use of CPT codes 96401-96549 for chemotherapy and other highly complex drug or highly complex biologic agent administration.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
Title XVIII of the Social Security Act, §1833 (e) prohibits Medicare payment for any claim which lacks the necessary information to process the claim.
Article Guidance
The information in this article contains billing, coding or other guidelines that complement the Local Coverage Determination (LCD) for Advance Care Planning L38970.
ICD-10-CM Codes that Support Medical Necessity
No specific diagnosis is required for the ACP codes to be billed. An ICD-10 code pertaining to the condition for which counseling is being provided, or to reflect an administrative examination, or a well exam diagnosis when furnished as part of the AWV.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
Title XVIII of the Social Security Act, §1833 (e) prohibits Medicare payment for any claim which lacks the necessary information to process the claim
Article Guidance
The information in this article contains billing, coding or other guidelines that complement the Local Coverage Determination (LCD) for Ambulance Services L34549.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
How many days of hospitalization is required for MA?
Most MA plans waive the 3-day hospitalization requirement. For each benefit period, Medicare Part A covers up to 20 days of care in full. After that, Medicare Part A covers up to an additional 80 days, with the patient paying coinsurance for each day.
Is SNF medically predictable?
It is medically predictable at the time of the hospital discharge they need covered care within a pre-determined time period and the care begins within that time. They need skilled nursing or rehabilitation services daily which, as a practical matter, can only be provided in a SNF on an inpatient basis.
Does Medicare cover SNF days?
Medicare Advantage (MA), 1876 Cost, or Programs of All-Inclusive Care for the Elderly (PACE) Plans typically waive the 3-day hospitalization requirement. MA plans must cover the same number of SNF days Original Medicare covers, but they may cover more SNF days than Original Medicare.
