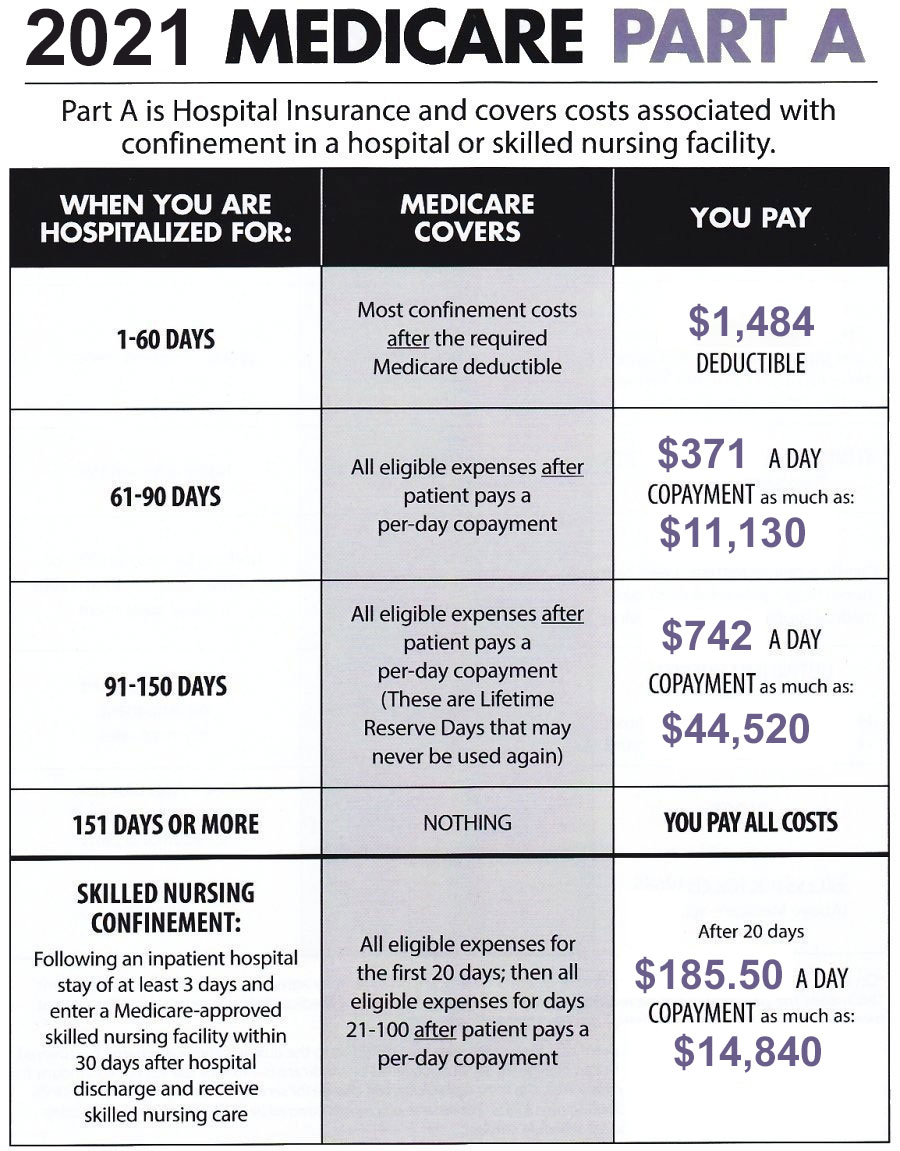
Medicare-covered hospital services include:
- Semi-private rooms
- Meals
- General nursing
- Drugs as part of your inpatient treatment (including methadone to treat an opioid use disorder)
- Other hospital services and supplies as part of your inpatient treatment
Does Medicare cover inpatient hospital services?
Hospital services (inpatient and outpatient) are covered when Medicare criteria are met. All hospital services must be reasonable and necessary to be covered. Decisions on the setting for delivery of healthcare services should be based on nationally recognized guidelines and evidence-based medical literature.
What services do you get as an outpatient from Medicare?
diagnostic and treatment services you get as an outpatient from a Medicare-participating hospital. Covered outpatient hospital services may include: Emergency or observation services, which may include an overnight stay in the hospital or outpatient clinic services, including same-day surgery.
What is covered under outpatient hospital services?
Outpatient hospital services. Medicare Part B (Medical Insurance) covers Medically necessary diagnostic and treatment services you get as an outpatient from a Medicare-participating hospital. Covered outpatient hospital services may include: Emergency or observation services, which may include an overnight stay in the hospital or services in an...
What are the services provided by a hospital?
Hospital facilities including the use of the emergency room Services of non-physician anesthetists, therapists and other aides Medical supplies, such as gauze, oxygen, ointments and surgical dressings Casts, splints and other devices used for the reduction of fractures and dislocations

Does Medicare cover hospital care?
Medicare Part A hospital insurance covers inpatient hospital care, skilled nursing facility, hospice, lab tests, surgery, home health care.
Which part of the Medicare program covers hospital services?
Medicare Part AMedicare Part A (Hospital Insurance) Part A covers inpatient hospital stays, care in a skilled nursing facility, hospice care, and some home health care.
Does Medicare pay 100 percent of hospital bills?
According to the Centers for Medicare and Medicaid Services (CMS), more than 60 million people are covered by Medicare. Although Medicare covers most medically necessary inpatient and outpatient health expenses, Medicare reimbursement sometimes does not pay 100% of your medical costs.
What types of services does Medicare pay for?
Medicare Services. Medicare Part A and Part B cover a variety of services, including inpatient hospital care, skilled nursing care, preventive services, home health care and ambulance transportation. Additional services such as vision and dental care may be available through a Medicare Advantage plan.
What will Medicare not pay for?
In general, Original Medicare does not cover: Long-term care (such as extended nursing home stays or custodial care) Hearing aids. Most vision care, notably eyeglasses and contacts. Most dental care, notably dentures.
How long can you stay in the hospital under Medicare?
90 daysMedicare covers a hospital stay of up to 90 days, though a person may still need to pay coinsurance during this time. While Medicare does help fund longer stays, it may take the extra time from an individual's reserve days. Medicare provides 60 lifetime reserve days.
Does Medicare cover emergency room visits?
Does Medicare Part A Cover Emergency Room Visits? Medicare Part A is sometimes called “hospital insurance,” but it only covers the costs of an emergency room (ER) visit if you're admitted to the hospital to treat the illness or injury that brought you to the ER.
Does Medicare cover ICU costs?
(Medicare will pay for a private room only if it is "medically necessary.") all meals. regular nursing services. operating room, intensive care unit, or coronary care unit charges.
What is the 3 day rule for Medicare?
The 3-day rule requires the patient have a medically necessary 3-consecutive-day inpatient hospital stay. The 3-consecutive-day count doesn't include the discharge day or pre-admission time spent in the Emergency Room (ER) or outpatient observation.
Do all hospitals accept Medicare?
Medicare is accepted at over 7,000 hospitals, which must meet Medicare's safety and care standards. In most cases, you can go to any doctor, healthcare provider, hospital or facility that's enrolled in Medicare. In fact, more than 7,000 hospitals in the U.S. provide services to Medicare patients.
What are the 4 types of Medicare?
There are four parts of Medicare: Part A, Part B, Part C, and Part D.Part A provides inpatient/hospital coverage.Part B provides outpatient/medical coverage.Part C offers an alternate way to receive your Medicare benefits (see below for more information).Part D provides prescription drug coverage.
Does Medicare cover surgery?
Does Medicare Cover Surgery? Medicare covers surgeries that are deemed medically necessary. This means that procedures like cosmetic surgeries typically aren't covered. Medicare Part A covers inpatient procedures, while Part B covers outpatient procedures.
What does Medicare Part B cover?
Part B also covers durable medical equipment, home health care, and some preventive services.
Is my test, item, or service covered?
Find out if your test, item or service is covered. Medicare coverage for many tests, items, and services depends on where you live. This list includes tests, items, and services (covered and non-covered) if coverage is the same no matter where you live.
What is covered by Medicare outpatient?
Covered outpatient hospital services may include: Emergency or observation services, which may include an overnight stay in the hospital or outpatient clinic services, including same-day surgery. Certain drugs and biologicals that you ...
How much does Medicare pay for outpatient care?
You usually pay 20% of the Medicare-approved amount for the doctor or other health care provider's services. You may pay more for outpatient services you get in a hospital than you’ll pay for the same care in a doctor’s office. However, the hospital outpatient Copayment for the service is capped at the inpatient deductible amount.
What is preventive care?
preventive services. Health care to prevent illness or detect illness at an early stage, when treatment is likely to work best (for example, preventive services include Pap tests, flu shots, and screening mammograms). . If you get hospital outpatient services in a critical access hospital, your copayment may be higher and may exceed ...
What is a copayment in a hospital?
An amount you may be required to pay as your share of the cost for a medical service or supply, like a doctor's visit, hospital outpatient visit, or prescription drug. A copayment is usually a set amount, rather than a percentage.
What is a deductible for Medicare?
deductible. The amount you must pay for health care or prescriptions before Original Medicare, your prescription drug plan, or your other insurance begins to pay. for each service. The Part B deductible applies, except for certain. preventive services.
Can you get a copayment for outpatient services in a critical access hospital?
If you get hospital outpatient services in a critical access hospital, your copayment may be higher and may exceed the Part A hospital stay deductible. If you get hospital outpatient services in a critical access hospital, your copayment may be higher and may exceed the Part A hospital stay deductible.
Does Part B cover prescription drugs?
Certain drugs and biologicals that you wouldn’t usually give yourself. Generally, Part B doesn't cover prescription and over-the-counter drugs you get in an outpatient setting, sometimes called “self-administered drugs.".
How to know if Medicare will cover you?
Talk to your doctor or other health care provider about why you need certain services or supplies. Ask if Medicare will cover them. You may need something that's usually covered but your provider thinks that Medicare won't cover it in your situation. If so, you'll have to read and sign a notice. The notice says that you may have to pay for the item, service, or supply.
What are the factors that determine Medicare coverage?
Medicare coverage is based on 3 main factors 1 Federal and state laws. 2 National coverage decisions made by Medicare about whether something is covered. 3 Local coverage decisions made by companies in each state that process claims for Medicare. These companies decide whether something is medically necessary and should be covered in their area.
What is national coverage?
National coverage decisions made by Medicare about whether something is covered. Local coverage decisions made by companies in each state that process claims for Medicare. These companies decide whether something is medically necessary and should be covered in their area.
What is a hospital?
A hospital is an institution primarily engaged in providing, by or under the supervision of physicians, inpatient diagnostic ...
What is an accredited hospital?
Accredited Hospitals - A hospital accredited by a CMS-approved accreditation program may substitute accreditation under that program for survey by the State Survey Agency.
Is a psychiatric hospital a Medicare provider?
Psychiatric hospitals are subject to additional regulations beyond basic hospital conditions of participation. The State Survey Agency evaluates and certifies each participating hospital as a whole for compliance with the Medicare requirements and certifies it as a single provider institution.
Can a hospital have multiple campuses?
Under the Medicare provider-based rules it is possible for ‘one' hospital to have multiple inpatient campuses and outpatient locations. It is not permissible to certify only part of a participating hospital. Psychiatric hospitals that participate in Medicare as a Distinct Part Psychiatric hospital are not required to participate in their entirety.
Do psychiatrists have to participate in Medicare?
Psychiatric hospitals that participate in Medicare as a Distinct Part Psychiatric hospital are not required to participate in their entirety. However, the following are not considered parts of the hospital and are not to be included in the evaluation of the hospital's compliance:
Can a hospital's Medicare provider agreement be terminated?
Should an individual or entity (hospital) refuse to allow immediate access upon reasonable request to either a State Agency , CMS surveyor, a CMS-approved accreditation organization, or CMS contract surveyors, the hospital's Medicare provider agreement may be terminated.
Does Medicare cover exceptions?
This booklet outlines the 4 categories of items and services Medicare doesn’t cover and exceptions (items and services Medicare may cover). This material isn’t an all-inclusive list of items and services Medicare may or may not cover.
Does Medicare cover personal comfort items?
Medicare doesn’t cover personal comfort items because these items don’t meaningfully contribute to treating a patient’s illness or injury or the functioning of a malformed body member. Some examples of personal comfort items include:
Does Medicare cover dental care?
Medicare doesn’t cover items and services for the care, treatment, filling, removal, or replacement of teeth or the structures directly supporting the teeth, such as preparing the mouth for dentures, or removing diseased teeth in an infected jaw. The structures directly supporting the teeth are the periodontium, including:
Does Medicare cover non-physician services?
Medicare normally excludes coverage for non-physician services to Part A or Part B hospital inpatients unless those services are provided either directly by the hospital/SNF or under an arrangement that the hospital/SNF makes with an outside source.