Skilled nursing facility (SNF) care. Medicare Part A (Hospital Insurance) covers. Skilled nursing care. provided in a SNF in certain conditions for a limited time (on a short-term basis) if all of these conditions are met: You have Part A and have days left in your Benefit period.
Full Answer
What qualifies as skilled nursing care for Medicare?
Skilled nursing facility (SNF) care is health care given when you need skilled nursing or therapy staff to treat, manage, observe, and evaluate your care. Examples of SNF care include intravenous injections and physical therapy. Care that can be given by non‑professional staff isn’t considered skilled care.
What is the difference between hospice and skilled nursing facility?
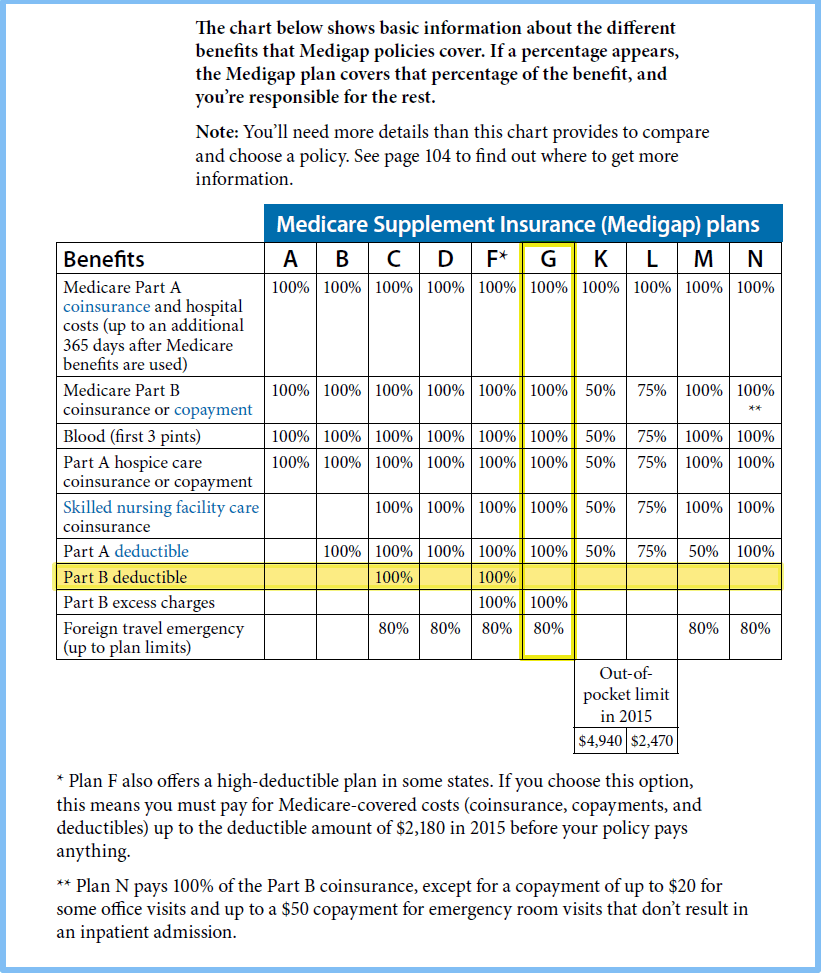
Medicare Part A coverage—skilled nursing facility care. Skilled nursing facility care coverage. Skilled Nursing Facility Checklist [PDF, 174KB] [PDF, 174 KB] Assessments. Care plans. Your rights in a skilled nursing facility. Reporting & resolving problems. Get help paying for skilled nursing facility care. Find hospitals & skilled nursing ...
Does Medicare cover skilled nursing at home?
Sep 15, 2018 · Medicare defines a skilled nursing facility as “a nursing facility with the staff and equipment to give skilled nursing care and, in most cases, skilled rehabilitative services and other related health services.”
What are the benefits of skilled nursing?
Skilled nursing facility (SNF) situations Medicare covers skilled nursing facility (SNF) care. There are some situations that may impact your coverage and costs. Observation services Your doctor may order observation services to help decide whether you need to be admitted to the hospital as an inpatient or can be discharged.

When Could I Need Skilled Nursing Care?
You may need skilled nursing care if you have an illness or injury that requires treatment or monitoring. Skilled nursing facilities provide 24-hou...
When Would I Be Eligible For Medicare Coverage of Skilled Nursing Facility Care?
Generally Medicare will help pay for skilled nursing facility (SNF) care if all of these are true: 1. You were a hospital inpatient for at least th...
What Skilled Nursing Facility Services Does Medicare Cover?
Typically Medicare will pay for the following items and services delivered by trained health professionals: 1. Semi-private room 2. Meals 3. Care b...
How Can I Get Help Paying Skilled Nursing Facility Costs?
You might want to consider a Medicare Supplement plan for help paying some of your skilled nursing facility out-of-pocket costs. Medicare Supplemen...
How Can I Find A Medicare-Certified Skilled Nursing Facility?
You can call Medicare to find out about Medicare-certified skilled nursing facilities in your area. Call Medicare at 1-800-MEDICARE (1-800-633-4227...
How long does Medicare pay for skilled nursing?
Generally Medicare will pay 100% of the Medicare-approved cost for the first 20 days and part of the cost for another 80 days of medically necessary care in a Medicare-certified skilled nursing facility each benefit period. You typically need to pay coinsurance for days 21-100. If your stay in a skilled nursing facility longer than 100 days in ...
What is SNF care?
Your SNF care is related to a condition you were treated for in the hospital, or is a new condition that started during that treatment. You haven’t used up all the days in your Medicare benefit period.
What does Medicare pay for?
Typically Medicare will pay for the following items and services delivered by trained health professionals: 1 Semi-private room 2 Meals 3 Care by registered nurses 4 Therapy care (including physical, speech and occupational therapy) 5 Medical social services 6 Nutrition counseling 7 Prescription medications 8 Certain medical equipment and supplies 9 Ambulance transportation (when other transportation would be dangerous to your health) if you need care that’s not available at the skilled nursing facility
How long does Medicare benefit last?
You haven’t used up all the days in your Medicare benefit period. A benefit period starts the day you’re admitted to a hospital as an inpatient. It ends when you haven’t been an inpatient in a hospital or skilled nursing facility for 60 days in a row. If you meet these requirements, Medicare may cover skilled nursing facility care ...
What is Medicare Supplement Plan?
Medicare Supplement (Medigap) plans help pay for some of your out-of-pocket costs under Medicare Part A and Part B, including certain cost-sharing expenses.
How long does Medicare cover coinsurance?
You typically need to pay coinsurance for days 21-100. If your stay in a skilled nursing facility longer than 100 days in a benefit period, Medicare generally doesn’t cover these costs.
Why do you need skilled nursing?
You may need skilled nursing care if you have an illness or injury that requires treatment or monitoring. Skilled nursing facilities provide 24-hour care for people who need rehabilitation services or who suffer from serious health issues that are too complicated to be tended at home. Some skilled nursing facilities might have laboratory, ...
How long does a break in skilled care last?
If your break in skilled care lasts for at least 60 days in a row, this ends your current benefit period and renews your SNF benefits. This means that the maximum coverage available would be up to 100 days of SNF benefits.
What happens if you refuse skilled care?
Refusing care. If you refuse your daily skilled care or therapy, you may lose your Medicare SNF coverage. If your condition won't allow you to get skilled care (like if you get the flu), you may be able to continue to get Medicare coverage temporarily.
What happens if you leave SNF?
If you stop getting skilled care in the SNF, or leave the SNF altogether, your SNF coverage may be affected depending on how long your break in SNF care lasts.
Can you be readmitted to the hospital if you are in a SNF?
If you're in a SNF, there may be situations where you need to be readmitted to the hospital. If this happens, there's no guarantee that a bed will be available for you at the same SNF if you need more skilled care after your hospital stay. Ask the SNF if it will hold a bed for you if you must go back to the hospital.
Does Medicare cover skilled nursing?
Medicare covers skilled nursing facility (SNF) care. There are some situations that may impact your coverage and costs.
What is skilled nursing facility?
Skilled nursing facilities are sometimes called post-acute rehabilitation centers, but the rules for a stay in an acute care rehabilitation center, or inpatient rehab facility (IRF), are different. For more information, see our article on Medicare coverage of inpatient rehab facility stays. Skilled nursing facility care, which takes place in ...
How many days do you have to stay in a skilled nursing facility?
Your stay in a skilled nursing facility must follow at least three consecutive days, not counting the day of discharge, in the hospital. And you must have been actually "admitted" to the hospital, not just held "under observation."
How long does custodial care last?
Custodial care often lasts months or years, and is not covered at all by Medicare. For the most part, custodial care amounts to assistance with the tasks of daily life: eating, dressing, bathing, moving around, and some recreation.
How long does Medicare cover inpatient care?
For each spell of illness, Medicare will cover only a total of 100 days of inpatient care in a skilled nursing facility, and then only if your doctor continues to prescribe skilled nursing care or therapy. For the first 20 of 100 days, Medicare will pay for all covered costs, which include all basic services but not television, telephone, ...
What does a doctor need to certify?
Your doctor must certify that you require daily skilled nursing care or skilled rehabilitative services. This care can include rehabilitative services by professional therapists, such as physical, occupational, or speech therapists, or skilled nursing treatment that require a trained professional, such as giving injections, changing dressings, ...
How long does nursing home care last?
It is intended to follow acute hospital care due to serious illness, injury, or surgery—and usually lasts only a matter of days or weeks. In contrast, most nursing homes provide what is called custodial care—primarily personal, nonmedical care for people who are no longer able to fully care for themselves. Custodial care often lasts months ...
Does Medicare cover skilled nursing?
Medicare Part A will cover part of your stay in a skilled nursing facility if you meet a number of requirements. A growing number of patients recovering from surgery or a major illness are referred by their doctors to skilled nursing facilities.
How long do you have to be in a skilled nursing facility to qualify for Medicare?
The patient must go to a Skilled Nursing Facility that has a Medicare certification within thirty days ...
What is skilled nursing?
Skilled nursing services are specific skills that are provided by health care employees like physical therapists, nursing staff, pathologists, and physical therapists. Guidelines include doctor ordered care with certified health care employees. Also, they must treat current conditions or any new condition that occurs during your stay ...
Who is Lindsay Malzone?
Lindsay Malzone is the Medicare expert for MedicareFAQ. She has been working in the Medicare industry since 2017. She is featured in many publications as well as writes regularly for other expert columns regarding Medicare.
Does Medicare cover hospice?
Yes, Medica re will cover hospice at a Skilled Nursing Facility as long as they are a Medicare-certified hospice center. However, Medicare will not cover room and board. What does Medicare consider skilled nursing? Medicare considers skilled nursing to be physical therapists, nursing staff, pathologists, physical therapists, etc.
How long does a SNF stay in a hospital?
The 3-day rule ensures that the beneficiary has a medically necessary stay of 3 consecutive days as an inpatient in a hospital facility.
When is a skilled nursing facility readmitted?
When the beneficiary is discharged from a skilled nursing facility, and then readmitted within 30 days , this is considered readmission. Another instance of readmission is if a beneficiary were to be in the care of a Skilled Nursing Facility and then ended up needing new care within 30 days post the first noncoverage day.
Can a beneficiary move to a skilled nursing facility?
If a beneficiary needs a Skilled Nursing Facility and goes but doesn’t have a qualifying stay in a hospital facility, they can move to a Skilled Nursing Facility after they remain for the night. They’ll then go the next night and receive coverage.
What is skilled nursing?
What Is a Skilled Nursing Facility? A skilled nursing facility is an in-patient rehabilitation and medical treatment center staffed with trained medical professionals. They provide the medically-necessary services of licensed nurses, physical and occupational therapists, speech pathologists, and audiologists.
How much does a skilled nursing facility cost?
In 2019, for example, a private room in a skilled nursing facility or nursing home cost an average of $102,200 a year, according to a report on long-term care by Genworth. 5 .
How long can a patient stay in a skilled nursing facility?
Patients needing post-hospital care in a skilled nursing facility who are enrolled in Medicare are covered for stays of up to 100 days in a Medicare-certified skilled nursing facility if the patient meets Medicare's requirements.
Who can report nursing home violations?
Skilled nursing facilities that violate the rules can be reported to authorities, such as the local long-term care ombudsmen and state nursing home regulatory agencies. 3 . For example, a woman who suspects her mother was denied entry to a particular nursing home in California because of her race could report the incident to ...
Who is Julia Kagan?
Julia Kagan has written about personal finance for more than 25 years and for Investopedia since 2014. The former editor of Consumer Reports, she is an expert in credit and debt, retirement planning, home ownership, employment issues, and insurance. She is a graduate of Bryn Mawr College (A.B., history) and has an MFA in creative nonfiction ...
What is notice issue in Medicare?
The key points are that Medicare beneficiaries are entitled to have Medicare, not the facility, determine whether the beneficiary’s care is covered by Medicare; a SNF must give a beneficiary the proper notices (in expedited and standard appeals) and provide information to the BFCC-QIO (in expedited appeals) or else it is responsible for the costs of the beneficiary’s care; and even if Medicare does not pay for the care, a resident has the right to remain in the SNF (if the resident has another source of payment).
What is expedited appeal?
The SNF must give notice to the beneficiary at least two days prior to termination of all Part A services when the beneficiary still has days left in the benefit period , [4] using the Notice of Medicare Provider Non-Coverage, Form CMS-10123, to inform the beneficiary of how to request an expedited redetermination and, if the beneficiary seeks an expedited determination, the Detailed Explanation of Non-Coverage (DENC), Form CMS-10124. [5]
Can a SNF discharge a Medicare beneficiary?
Skilled nursing facilities (SNFs) often tell Medicare beneficiaries and their families that they intend to “discharge” a Medicare beneficiary because Medicare will not pay for the beneficiary’s stay under either Part A (traditional Medicare) or Part C (Medicare Advantage). Such a statement unfortunately misleads many beneficiaries into incorrectly believing, not only that Medicare has decided that it will not pay for the stay, but also that a SNF can evict a resident from the facility if it concludes that Medicare is unlikely to pay for the resident’s stay. [1] The truth is that when a SNF tells a beneficiary that he or she is “discharged,” (1) at that point, Medicare has not yet made any determination about coverage and (2) a resident cannot be evicted solely because Medicare will not pay for the stay.
:max_bytes(150000):strip_icc()/GettyImages-182800841-5894f4825f9b5874ee438219.jpg)