There are five successive levels of appeal in the Medicare Part D program. Redetermination by the Part D Plan Sponsor; Reconsideration by the Independent Review Entity; Hearing by an Administrative Law Judge or Attorney Adjudicator; Review by the Medicare Appeals Council; Review by a Federal District Court
What is the appeal process for Medicare Part D coverage?
The appeal process is the same in stand-alone Part D plans and Medicare Advantage Plans with Part D coverage. Follow the steps below if your plan denied coverage for your prescription.
What kinds of Medicare notices can set off an appeal?
There are a few different notices you might receive from Medicare that would set off an appeal. Some common notices include: Advance Beneficiary Notice of Noncoverage (ABN). An ABN lets you know that an item, service, or prescription won’t be covered or will no longer be covered. Skilled Nursing Facility Advance Beneficiary Notice (SNF ABN).
Can a drug be appealed under Part D?
Introduction to Part D appeals. For example, you may be able to try a comparable drug that is on the formulary. If switching to another drug is not an option, you can choose to appeal. Your provider may appeal on your behalf or help you with the appeal process, but is not required to do so.
How many levels of Appeal are there for Medicare?
The appeals process has five levels. Each level is a different review process with a different timetable. You’ll need to request an appeal at each level. If your appeal is successful at the first level, or if you agree with Medicare’s reasoning for denying your appeal, you can stop there.
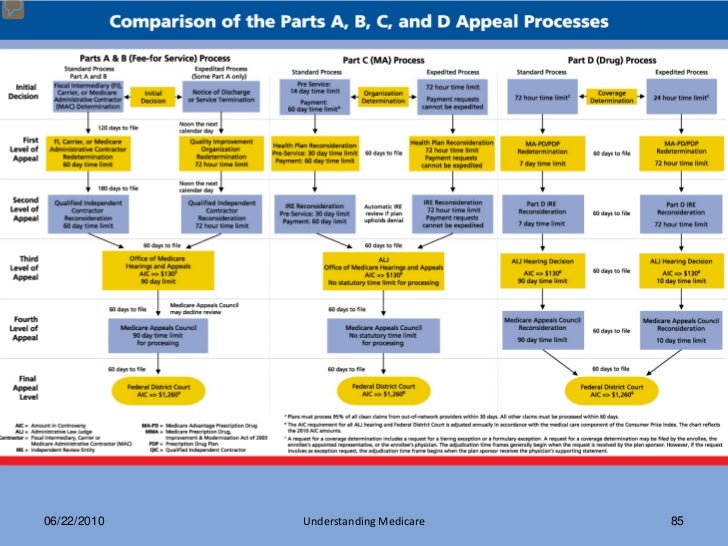
What are the five steps in the Medicare appeals process?
The Social Security Act (the Act) establishes five levels to the Medicare appeals process: redetermination, reconsideration, Administrative Law Judge hearing, Medicare Appeals Council review, and judicial review in U.S. District Court. At the first level of the appeal process, the MAC processes the redetermination.
What are the chances of winning a Medicare appeal?
People have a strong chance of winning their Medicare appeal. According to Center, 80 percent of Medicare Part A appeals and 92 percent of Part B appeals turn out in favor of the person appealing.
What are the steps taken when appealing a Medicare claim?
Left navigationFile a complaint (grievance)File a claim.Check the status of a claim.File an appeal. Appeals if you have a Medicare health plan. Get help filing an appeal.Your right to a fast appeal.Authorization to Disclose Personal Health Information.
What is the first step in the Medicare appeals process?
If you have a Medicare health plan, start the appeal process through your plan. Follow the directions in the plan's initial denial notice and plan materials. You, your representative, or your doctor must ask for an appeal from your plan within 60 days from the date of the coverage determination.
What should I say in a Medicare appeal?
What are the steps for filing an appeal for original Medicare?your name and address.your Medicare number (as shown on your Medicare card)the items you want Medicare to pay for and the date you received the service or item.the name of your representative if someone is helping you manage your claim.More items...•
How long does it take Medicare to respond to an appeal?
about 60 daysHow Long Does a Medicare Appeal Take? You can expect a decision on your Medicare appeal within about 60 days. Officially known as a “Medicare Redetermination Notice,” the decision may come in a letter or an MSN. Medicare Advantage plans typically decide within 14 days.
How many levels of appeal does Medicare have?
five levelsOverview - Standard Appeals Process There are five levels in the Medicare Part A and Part B appeals process. The levels are: First Level of Appeal: Redetermination by a Medicare Administrative Contractor (MAC) Second Level of Appeal: Reconsideration by a Qualified Independent Contractor (QIC)
How does Medicare handle disputes over claims?
You'll get a “Medicare Redetermination Notice” from the MAC, which will tell you how they decided your appeal. If you disagree with the decision made, you have 180 days to request a Reconsideration by a Qualified Independent Contractor (QIC), which is level 2 in the appeals process.
How do I write a Medicare appeal letter?
The Medicare appeal letter format should include the beneficiary's name, their Medicare health insurance number, the claim number and specific item or service that is associated with the appeal, dates of service, name and location of the facility where the service was performed and the patient's signature.
Who pays if Medicare denies a claim?
The denial says they will not pay. If you think they should pay, you can challenge their decision not to pay. This is called “appealing a denial.” If you appeal a denial, Medicare may decide to pay some or all of the charge after all.
What is a first level appeal?
Any party to the initial claim determination that is dissatisfied with the decision may request a redetermination.
What is a standard appeal?
Under the de novo standard, the appellate court reviews the evidence as though considering the matter for the first time, allowing the appeals court to substitute its own judgment about the application of the law to the facts to determine whether the lower court acted correctly.
What is an ABN in nursing?
An ABN lets you know that an item, service, or prescription won’t be covered or will no longer be covered. Skilled Nursing Facility Advance Beneficiary Notice (SNF ABN). An SNF ABN lets you know that Medicare will no longer be covering your stay in a skilled nursing facility.
Why is Medicare denying my coverage?
There are a few reasons Medicare might deny your coverage, including: Your item, service, or prescription isn’t medically necessary.
What is the first level of Medicare appeal?
The first level is called redetermination. This is where your initial appeal request will go. Redetermination is handled by the Medicare administrative contractor. They’ll review all the information you’ve sent and determine whether to cover your item, service, or prescription.
How long do you have to appeal a Medicare denial?
You have 120 days from a Medicare denial or penalty to file an appeal. Medicare will let you know in writing if your coverage has been denied or you’ve been assessed a penalty. The notice you’ll receive will let you know the steps you can take to file an appeal. In a few cases, you’ll file what’s called a fast appeal.
What is it called when you disagree with a Medicare decision?
One of those is the right to take action if you disagree with a Medicare coverage decision. This is called an appeal, and you can use it for concerns about each part of Medicare, including:
What is Medicare appeal?
It helps to provide evidence that supports your appeals case from a doctor or other provider. There might be times when Medicare denies your coverage for an item, service, or test. You have the right to formally disagree with this decision and encourage Medicare to change it. This process is called a Medicare appeal.
Why do you appeal Medicare?
Reasons for appeal. Appeals process. Takeaway. You’ll receive a notice when Medicare makes any decisions about your coverage. You can appeal a decision Medicare makes about your coverage or price for coverage. Your appeal should explain why you don’t agree with Medicare’s decision. It helps to provide evidence that supports your appeals case ...
What if my plan won't cover a drug I think I need?
You have the right to do all of these (even before you buy a certain drug):
What happens if a pharmacy can't fill a prescription?
If your network pharmacy can't fill a prescription, the pharmacist will show you a notice that explains how to contact your Medicare drug plan so you can make your request.
What is formulary in medical terms?
formulary. A list of prescription drugs covered by a prescription drug plan or another insurance plan offering prescription drug benefits. Also called a drug list. .
What is EOC in Medicare?
Medicare prescription drug coverage appeals. Your plan will send you information that explains your rights called an " Evidence of Coverage " (EOC). Call your plan if you have questions about your EOC. You have the right to ask your plan to provide or pay for a drug you think should be covered, provided, or continued.
What is coverage determination?
A coverage determination is the first decision made by your Medicare drug plan (not the pharmacy) about your. benefits. The health care items or services covered under a health insurance plan. Covered benefits and excluded services are defined in the health insurance plan's coverage documents. , including these: Whether a certain drug is covered.
How many levels of appeals are there for Medicare?
Your Medicare drug plan will send you a written decision. If you disagree with this decision, you have the right to appeal. The appeals process has 5 levels. If you disagree with the decision made at any level of the process, you can generally go to the next level.
What are the levels of appeal?
At each level, you'll get instructions in the decision letter on how to move to the next level of appeal. Level 1: Redetermination from your plan. Level 2: Review by an Independent Review Entity (IRE) Level 3: Decision by the Office of Medicare Hearings and Appeals (OMHA) Level 4: Review by the Medicare Appeals Council ( Appeals Council) ...
What is a level 2 appeal?
The Level 2 appeal is called a "reconsideration".
How long does it take to get a Part D reconsideration?
If your request is expedited, the IRE has 72 hours to notify you of its decision.
How long do you have to appeal a level 3 Medicare claim?
You have 60 days after receiving the Level 2 decision to request a Level 3 hearing in writing. Please note that the Office of Medicare Hearings and Appeals is responsible only for the Level 3 claims appeals and certain Medicare entitlement appeals and Part B premium appeals.
What does the IRE take into consideration?
The IRE will take into consideration the views of your prescribing physician.
How long does it take to get a response to an appeal?
In most cases, you will receive notice (called "Notice of Reconsideration Determination") of the IRE's decision within 7 days after submitting your request for a reconsideration .
Is OMHA responsible for levels 1 and 2?
OMHA is not responsible for levels 1, 2, 4, and 5 of the appeals process. OMHA provides additional information on other levels of appeals to help you understand the appeals process in a broad context. Content created by Office of Medicare Hearings and Appeals (OMHA) Content last reviewed on January 9, 2020.
Who conducts level 2 appeals?
An Independent Review Entity (IRE), retained by CMS, will conduct the Level 2 appeal.
Medicare Prescription Drug Appeals & Grievances
December 2021: CMS has developed frequently asked questions (FAQs) and model dismissal notices based on recent regulatory changes in CMS-4190-F2 related to dismissals of Part C organization determinations and reconsiderations and Part D coverage determinations and redeterminations, effective January 1, 2022.
Web Based Training Course Available for Part D
The course covers requirements for Part D coverage determinations, appeals, and grievances. Complete details and a link to the training module can be found on the "Training" page (link on the left navigation menu on this page).
How many levels of appeal are there in Medicare?
There are five successive levels of appeal in the Medicare Part D program. A decision may be appealed to the next level of appeal when the lower appeal entity issues a decision that is unfavorable to the enrollee. Each unfavorable decision will contain the information needed to file an appeal request. Use the navigation tool on the left side of ...
When can a decision be appealed?
A decision may be appealed to the next level of appeal when the lower appeal entity issues a decision that is unfavorable to the enrollee. Each unfavorable decision will contain the information needed to file an appeal request.
What is level 1 appeal?
Level 1 Appeals: Medicare Prescription Drug Plan (Part D) You may file an appeal if you are in a Medicare Prescription Drug Plan and you have received a coverage determination from your drug plan sponsor with which you do not agree.
How long does it take for a drug plan to redetermine?
For an expedited redetermination, the plan has 72 hours to notify you of its decision.
How long does it take to appeal a Medicare prescription?
You must file your appeal in writing within 60 days, unless your drug plan accepts requests by telephone. Contact your Medicare Prescription Drug Plan or check your plan materials about the appropriate process for submitting a request for redetermination.
How long does it take to get a response from a drug plan?
When You Will Get a Response. Once your drug plan sponsor has received your request, it has seven (7) days (standard request) to notify you of its decision. If your prescription drug plan sponsor is unable to complete its decision within the required time frame, it is required to forward your appeal to Level 2.
Is OMHA responsible for levels 1 and 2?
OMHA is not responsible for levels 1, 2, 4, and 5 of the appeals process. OMHA provides additional information on other levels of appeals to help you understand the appeals process in a broad context. Content created by Office of Medicare Hearings and Appeals (OMHA) Content last reviewed on August 5, 2016.
