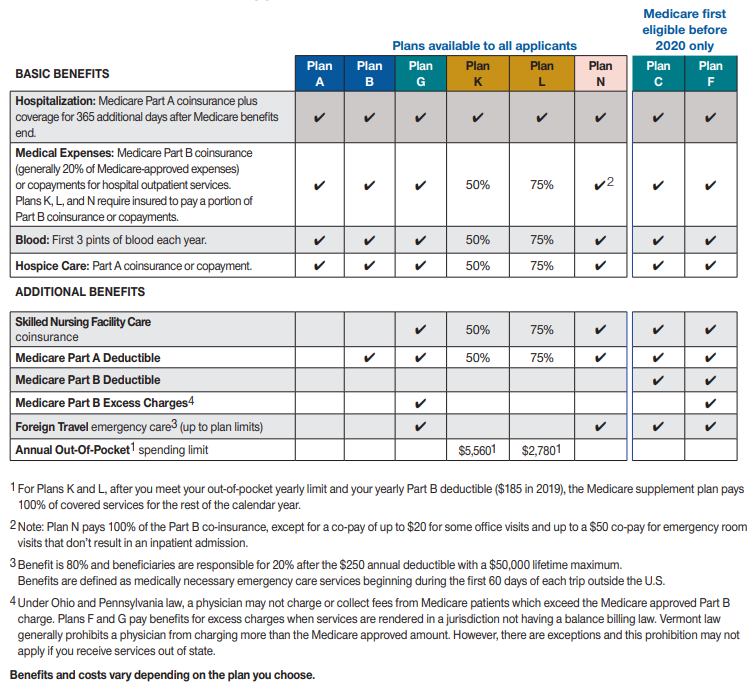
If you’re enrolled in a Medicare plan, you may have come across the term “Medicare-approved amount.” The Medicare-approved amount is the amount that Medicare pays your provider for your medical services. Since Medicare Part A has its own pricing structure in place, this approved amount generally refers to most Medicare Part B services.
What are the guidelines for Medicare?
or other qualified health care professional, per calendar month, with the following required elements: multiple (two or more) chronic conditions expected to last at least 12 months, or until the death of the patient chronic conditions place the patient at significant risk of death, acute exacerbation/ decompensation, or functional decline …
What is allowed amount insurance?
Allowed Amount on a Health Insurance Statement
- Allowed Amount With In-Network Care. If you used a provider that’s in-network with your health plan, the allowed amount is the discounted price your managed care health plan negotiated in ...
- Allowed Amount With Out-Of-Network Care. ...
- Summary. ...
- A Word From Verywell. ...
What are the administrative costs of Medicare?
administrative expenses per member: for every year, as a percentage of reported benefits per beneficiary, reported administrative expenses of medicare abd (mean [sd], $147.13
14.28] per member,...
What is Medicare Advantage plan and cost?
Medicare Advantage plans & Medicare Cost plans are health plans that are provided by private insurance companies. Learn more about Medicare Advantage plans & Medicare Cost plans and understand the type of coverage each provides. Speak with a Licensed Insurance Agent. 1-844-847-2659, TTY Users 711 Mon - Fri, 8am - 8pm ET .
What does the Medicare-approved amount mean?
The approved amount, also known as the Medicare-approved amount, is the fee that Medicare sets as how much a provider or supplier should be paid for a particular service or item. Original Medicare also calls this assignment. See also: Take Assignment, Participating Provider, and Non-Participating Provider.
What is Medicare-approved amount for doctor visit?
Medicare's approved amount for the service is $100. A doctor who accepts assignment agrees to the $100 as full payment for that service. The doctor bills Medicare who pays him or her 80% or $80, and you are responsible for the 20% coinsurance (after you have paid the Part B annual deductible).
Why is Medicare-approved amount different than Medicare paid?
The Medicare-approved amount is the amount of money that Medicare has agreed to pay for your services. This amount can differ depending on what services you're seeking, and who you are seeking them from. Using a Medicare participating provider can help to lower your out-of-pocket Medicare costs.
What is above Medicare-approved amounts?
Doctors who accept assignment have agreed to accept the Medicare-approved amount as their full payment. A doctor who doesn't accept assignment may charge you up to 15 percent more than the Medicare-approved amount. This overage is known as a Part B excess charge.
Does Medicare pay 100 percent of hospital bills?
According to the Centers for Medicare and Medicaid Services (CMS), more than 60 million people are covered by Medicare. Although Medicare covers most medically necessary inpatient and outpatient health expenses, Medicare reimbursement sometimes does not pay 100% of your medical costs.
Does Medicare Part B cover 100 percent?
Since you are not covered at 100% by Original Medicare, these Medicare Supplement plans help you create individualized full coverage benefits while still utilizing Original Medicare benefits. Medicare Supplement plans can cover the Medicare Part B coinsurance, so you are not left covering this out-of-pocket cost.
What is the difference between the Medicare approved amount for a service or supply and the actual charge?
BILLED CHARGE The amount of money a physician or supplier charges for a specific medical service or supply. Since Medicare and insurance companies usually negotiate lower rates for members, the actual charge is often greater than the "approved amount" that you and Medicare actually pay.
What does the allowed amount mean?
The maximum amount a plan will pay for a covered health care service. May also be called “eligible expense,” “payment allowance,” or “negotiated rate.” If your provider charges more than the plan's allowed amount, you may have to pay the difference. (
Can a Medicare patient pay out of pocket?
Keep in mind, though, that regardless of your relationship with Medicare, Medicare patients can always pay out-of-pocket for services that Medicare never covers, including wellness services.
What states do not charge Medicare excess?
Eight States Prohibit Medicare Excess ChargesConnecticut,Massachusetts,Minnesota,New York,Ohio,Pennsylvania,Rhode Island, and.Vermont.
How can I avoid excess Medicare charges?
How can you avoid Medicare Part B excess charges? The easiest way to avoid facing Medicare Part B excess charges is to limit yourself to visiting providers and medical suppliers who accept Medicare assignment. As mentioned above, most providers and physicians accept Medicare assignment.
Why do doctors not like Medicare Advantage plans?
If they don't say under budget, they end up losing money. Meaning, you may not receive the full extent of care. Thus, many doctors will likely tell you they do not like Medicare Advantage plans because private insurance companies make it difficult for them to get paid for their services.
What is Medicare approved amount?
The Medicare-approved amount is the total payment that Medicare has agreed to pay a health care provider for a service or item. Learn more your potential Medicare costs. The Medicare-approved amount is the amount of money that Medicare will pay a health care provider for a medical service or item.
How much can a provider charge for not accepting Medicare?
By law, a provider who does not accept Medicare assignment can only charge you up to 15 percent over the Medicare-approved amount. Let’s consider an example: You’ve been feeling some pain in your shoulder, so you make an appointment with your primary care doctor.
What is Medicare Supplement Insurance?
Some Medicare Supplement Insurance plans (also called Medigap) provide coverage for the Medicare Part B excess charges that may result when a health care provider does not accept Medicare assignment.
What is Medicare Part B excess charge?
What are Medicare Part B excess charges? You are responsible for paying any remaining difference between the Medicare-approved amount and the amount that your provider charges. This difference in cost is called a Medicare Part B excess charge. By law, a provider who does not accept Medicare assignment can only charge you up to 15 percent over ...
What does it mean when a doctor accepts Medicare assignment?
If a doctor or supplier accepts Medicare assignment, this means that they agree to accept the Medicare-approved amount for a service or item as payment in full. The Medicare-approved amount could potentially be less than the actual amount a doctor or supplier charges, depending on whether or not they accept Medicare assignment.
How much does Medicare pay for a doctor appointment?
Typically, you will pay 20 percent of the Medicare-approved amount, and Medicare will pay the remaining 80 percent .
Does Medicare cover a primary care appointment?
This appointment will be covered by Medicare Part B, and you have already satisfied your annual Part B deductible. Your primary care doctor accepts Medicare assignment, which means they have agreed to accept Medicare as full payment for their services. Because you have met your deductible for the year, you will split the Medicare-approved amount ...
What is Medicare approved amount?
The Medicare-approved amount, or “allowed amount,” is the amount that Medicare reimburses health care providers for the services they deliver. Learn more about the Medicare-approved amount and how it affects your Medicare costs. There’s a lot of terminology for Medicare beneficiaries to learn, and among them is “Medicare-approved amount” ...
What does Medicare cover?
The Medicare-approved amount applies mostly to services covered by Medicare Part B, which covers outpatient services like doctor’s appointments, and it also covers durable medical equipment (DME) such as wheelchairs and blood sugar test strips.
How much does Medicare coinsurance increase?
The higher the Medicare-approved amount, the higher your coinsurance billed amount will likely be. If the Medicare-approved amount for the X-rays in the example above was $250 instead of $200, that would increase the total cost of the visit to $400, which would also increase the cost of your coinsurance payment to $80 (20% of $400).
How much is coinsurance for Medicare Part B?
Medicare Part B typically requires a coinsurance payment of 20% of the Medicare-approved amount for covered care after you meet your annual Part B deductible. Using the example above, your 20% coinsurance payment for your visit to the health clinic would likely be $70 (20% of $350).
What is an excess charge for Medicare?
These providers reserve the right to charge up to 15% more than the Medicare-approved amount in what is known as an “excess charge.”
How much does Medicare pay for X-rays?
The X-rays may have a Medicare-approved amount of $200. And the brace itself might have a Medicare-approved amount of $50. (Note: these costs are hypothetical and are not based on actual Medicare costs for the services or items mentioned.) Based on the above costs, the health clinic would be allowed by Medicare to charge $350 total for ...
What is a participating provider?
Participating provider. A participating provider “accepts Medicare assignment,” meaning they agree to accept the Medicare-approved amount as full payment for their service or item. They bill Medicare using what are called CPT codes .
What is Medicare approved amount?
The Medicare-approved amount is the amount that Medicare pays to a healthcare provider or medical supplier who accepts assignment for Medicare-covered services. If a person visits a healthcare provider or supplier who does not accept assignment, they may have to pay an additional amount for the services or items.
How much is the deductible for Medicare?
They must also meet the annual deductible of $203 before Medicare funds any treatment. If a person chooses to go to a nonparticipating healthcare provider, they may have to pay an additional amount for the services or items. For example: A person visits their Medicare-participating doctor about a pain in their ankle.
How much is Medicare Part B deductible 2021?
A person pays a percentage of the Medicare-approved amount after they have paid their Medicare Part B annual deductible, which is $203 in 2021. The amount varies depending on several factors, including whether the healthcare provider is participating in the Medicare program.
How much can a non-participating provider charge for Medicare?
A nonparticipating provider can charge up to 15% more than the Medicare-approved amount, although there is a limit to the charges. A person is then responsible for the difference in cost between the amount that their healthcare provider charges and the Medicare-approved amount. The cost difference is called the Medicare Part B excess charge.
How much is Medicare Part A in 2021?
Medicare Part A has an annual deductible, which is $1,484 in 2021, and a fee schedule for hospitalization. Medicare pays approved costs above a person’s coinsurance amount. These apply as follows for each benefit period in 2021: $0 coinsurance for days 1–60. $371 coinsurance per day for days 61–90.
What is the Medicare Part B copayment?
For Medicare Part B, this comes to 20%. Copayment: This is a fixed dollar amount that an insured person pays when receiving certain treatments. For Medicare, this usually applies to prescription drugs.
Do providers charge for Medicare deductible?
Healthcare providers and suppliers agree to charge a person for only the Medicare deductible and coinsurance amount. They may also wait for Medicare to pay its share before asking for the remaining payment from the person who received the service or item.
How much does Medicare pay for outpatient therapy?
After your deductible is met, you typically pay 20% of the Medicare-approved amount for most doctor services (including most doctor services while you're a hospital inpatient), outpatient therapy, and Durable Medical Equipment (DME) Part C premium. The Part C monthly Premium varies by plan.
What is Medicare Advantage Plan?
A Medicare Advantage Plan (Part C) (like an HMO or PPO) or another Medicare health plan that offers Medicare prescription drug coverage. Creditable prescription drug coverage. In general, you'll have to pay this penalty for as long as you have a Medicare drug plan.
How much is coinsurance for days 91 and beyond?
Days 91 and beyond: $742 coinsurance per each "lifetime reserve day" after day 90 for each benefit period (up to 60 days over your lifetime). Beyond Lifetime reserve days : All costs. Note. You pay for private-duty nursing, a television, or a phone in your room.
How much is coinsurance for 61-90?
Days 61-90: $371 coinsurance per day of each benefit period. Days 91 and beyond: $742 coinsurance per each "lifetime reserve day" after day 90 for each benefit period (up to 60 days over your lifetime) Beyond lifetime reserve days: all costs. Part B premium.
What happens if you don't buy Medicare?
If you don't buy it when you're first eligible, your monthly premium may go up 10%. (You'll have to pay the higher premium for twice the number of years you could have had Part A, but didn't sign up.) Part A costs if you have Original Medicare. Note.
Do you pay more for outpatient services in a hospital?
For services that can also be provided in a doctor’s office, you may pay more for outpatient services you get in a hospital than you’ll pay for the same care in a doctor’s office . However, the hospital outpatient Copayment for the service is capped at the inpatient deductible amount.
Does Medicare cover room and board?
Medicare doesn't cover room and board when you get hospice care in your home or another facility where you live (like a nursing home). $1,484 Deductible for each Benefit period . Days 1–60: $0 Coinsurance for each benefit period. Days 61–90: $371 coinsurance per day of each benefit period.
Medicare Allowed Amount Definition
Maximum amount on which payment is based for covered health care services. This may be called “eligible expense,” “payment allowance” or “negotiated rate.” If your provider charges more than the medicare allowed amount, patient no need to pay that amount when they are participating with Medicare insurance.
Medicare Maximum Allowable Reimbursements
Unless otherwise indicated, for these Rules, the Medicare procedures and guidelines are effective upon adoption and implementation by the CMS. The particular procedure or guideline to be used is that which is in effect on the date the service is rendered.