Crossover is the transfer of processed claim data from Medicare operations to Medicaid
Medicaid
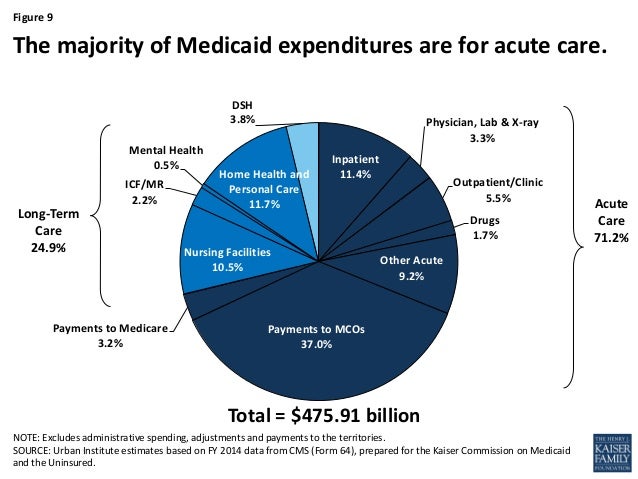
Medicaid in the United States is a federal and state program that helps with medical costs for some people with limited income and resources. Medicaid also offers benefits not normally covered by Medicare, including nursing home care and personal care services. The Health Insurance As…
How to set up Medicare crossover?
Medicare crossover means a claim involving a client who is eligible for both Medicare benefits and Medicaid. Sample 1 Based on 2 documents Examples of Medicare crossover in a sentence MHD developed an easy to use, web-based tool to adjust incorrectly billed and/or paid Medicaid and Medicare crossover claims.
What does crossover mean in medical insurance terms?
Apr 08, 2016 · The crossover process allows providers to submit a single claim for individuals dually eligible for Medicare and Medicaid, or qualified Medicare beneficiaries eligible for Medicaid payment of coinsurance and deductible to a Medicare fiscal intermediary, and also have it processed for Medicaid reimbursement.
How does the Medicare crossover claim system work?
What is meant by the crossover payment? When Medicaid providers submit claims to Medicare for Medicare/Medicaid beneficiaries, Medicare will pay the claim, apply a deductible/coinsurance or co-pay amount and then automatically forward the claim to Medicaid. Providers will NO longer need to bill Medicaid
How does Medicare Crossover claims?
Part 1 – Medicare/Medi-Cal Crossover Claims Overview Page updated: August 2020 Automatic Crossover Claims Medicare uses a consolidated Coordination of Benefits Contractor (COBC) to automatically cross over to Medi-Cal claims billed to any Medicare contractor for Medicare/Medi-Cal eligible recipients.

What does Medicare crossover mean?
A crossover claim is a claim for a recipient who is eligible for both Medicare and Medicaid, where Medicare pays a portion of the claim, and Medicaid is billed for any remaining deductible and/or coinsurance.Jan 18, 2021
When would you do a crossover claim?
In health insurance, a "crossover claim" occurs when a person eligible for Medicare and Medicaid receives health care services covered by both programs. The crossover claims process is designed to ensure the bill gets paid properly, and doesn't get paid twice.
What is a Medicare crossover only provider?
Crossover Only providers are those providers who are enrolled in Medicare, not enrolled in Medi-Cal, and provide services to dual-eligible beneficiaries. Dual-eligible beneficiaries are those beneficiaries who are eligible for coverage by Medicare (either Medicare Part A, Part B or both) and Medi-Cal.
Is a Medicare Medigap claim called a crossover claim?
Providers deal, primarily, with Medicare, and the Medigap company pays claims electronically through the “crossover”.May 11, 2017
Does Medicare crossover to AARP?
Things to remember: When Medicare does not crossover your claims to the AARP Medicare Supplement Plans, you will need to make sure this CO253 adjustment is applied before you electronically submit to AARP as a secondary payer.Mar 2, 2022
Does Medicare forward claims to secondary insurance?
If a Medicare member has secondary insurance coverage through one of our plans (such as the Federal Employee Program, Medex, a group policy, or coverage through a vendor), Medicare generally forwards claims to us for processing.
What is it commonly called when Medicare electronically forwards secondary claim information?
A. The Electronic Remittance Advice (ERA), or 835, is the electronic transaction which provides claims payment information in the HIPAA mandated ACSX12 005010X221A1 format.
How do I submit a void claim to Medicare?
The fastest way to cancel a claim is to call Medicare at 800-MEDICARE (800-633-4227). Tell the representative you need to cancel a claim you filed yourself. You might get transferred to a specialist or to your state's Medicare claims department.Jun 17, 2020
What is the difference between Medicare and Medicaid?
Medicare is a federal program that provides health coverage if you are 65+ or under 65 and have a disability, no matter your income. Medicaid is a state and federal program that provides health coverage if you have a very low income.
How does Medicare and Medigap work together?
Medigap pays for some of the bills left over by Medicare's coverage gaps – and it all happens automatically. Medicare and Medigap work together smoothly to pay for your medical bills. It's done automatically and usually without any input from you; that's how Medigap policies work.
Is Medigap primary or secondary?
secondaryMedigap policies are secondary insurance for Medicare. Because Medicare pays first, it is primary. But, Medicare doesn't pay for everything. So, a Supplemental policy is beneficial to have in place to protect you from unexpected medical costs.Oct 7, 2021
What is the purpose of the AOB form?
What is the purpose of AOB form? An Assignment of Benefits, or an AOB, is a document signed by a policyholder that allows a third party, such as a water extraction company, a roofer, or a plumber, to “stand in the shoes” of the insured and seek payment directly from the policyholder's insurance company.
What is Medicare Part A?
Medicare divides its services into Part A and Part B. Part A covers institutional services and Part B covers non-institutional services. Recipients may be covered for Part A only, Part B only or both.
When will Medicare replace HIC?
Beginning April 1, 2018 , the Health Insurance Claim (HIC) number traditionally appearing on Medicare cards is being replaced by a non-Social Security Number based Medicare Beneficiary Identifier (MBI) number. Updated Medicare cards with MBIs will be phased into use through December 31, 2019. Therefore, the term HIC will be phased out of the Medi-Cal provider manuals, as appropriate. Removal of references to HIC does not preclude providers from processing transactions using HIC numbers. Providers can continue to process both HIC and MBI numbers, as appropriate, from April 1, 2018 through December 31, 2019. Providers should refer to the CMS website for detailed information.
What is Medi-Cal eligibility verification?
The Medi-Cal eligibility verification system indicates a recipient’s Medicare coverage when a provider submits a Medi-Cal eligibility inquiry. One of the following messages will be returned if a recipient is eligible for Medicare:
Is Medicare covered by Medicare?
Most medical supplies are not covered by Medicare and can be billed directly to Medi-Cal. However, the medical supplies listed in the Medical Supplies: Medicare-Covered Services section of the appropriate Part 2 manual are covered by Medicare and must be billed to Medicare prior to billing Medi-Cal.
Do you have to bill Medicare before you use Medi-Cal?
If a recipient has Medicare Part A coverage only, and a provider is billing for Part A covered services, the provider must bill Medicare prior to billing Medi- Cal. However, if billing for Part
Can you bill Medicare for coinsurance?
Providers who accept persons eligible for both Medicare and Medi-Cal as recipients cannot bill them for the Medicare deductible and coinsurance amounts. These amounts can be billed only to Medi-Cal. (Refer to Welfare and Institutions Code [W&I Code], Section 14019.4.) However, providers should bill recipients for any Medi-Cal Share of Cost (SOC). Note: Providers are strongly advised to wait until they receive the Medicare payment before collecting SOC to avoid collecting amounts greater than the Medicare deductible and/or coinsurance.
Does California pay Medicare Part B?
California has a buy-in agreement with the federal government whereby the Department of Health Care Services (DHCS) pays the Medicare Part B premiums on behalf of all individuals eligible for Medi-Cal. These individuals are therefore protected by federal Medicaid rules that preclude providers from charging recipients any sums in addition to payments made to the provider.
What is a crossover claim?
In health insurance, a "crossover claim" occurs when a person eligible for Medicare and Medicaid receives health care services covered by both programs. The crossover claims process is designed to ensure the bill gets paid properly, and doesn't get paid twice. Advertisement.
Who sets rules for crossover claims?
Rules for crossover claims are set by the federal Centers for Medicare & Medicaid Services. Health-care providers submit all crossover claims to Medicare. Medicare assesses the claim, pays its portion of the bill, and then submits the remaining claim to Medicaid.
Is Medicare a federal program?
Medicare is a federal program that provides health care coverage to people age 65 and older, as well as disabled adults. Medicaid is a combined federal-state program that covers low-income people regardless of age. Because of overlaps in eligibility, some people may be covered by both programs.