
| If you sign up: | Coverage starts: |
|---|---|
| Before the month you turn 65 | The month you turn 65 |
| The month you turn 65 | The next month |
| 1 month after you turn 65 | 2 months after you sign up |
| 2 or 3 months after you turn 65 | 3 months after you sign up |
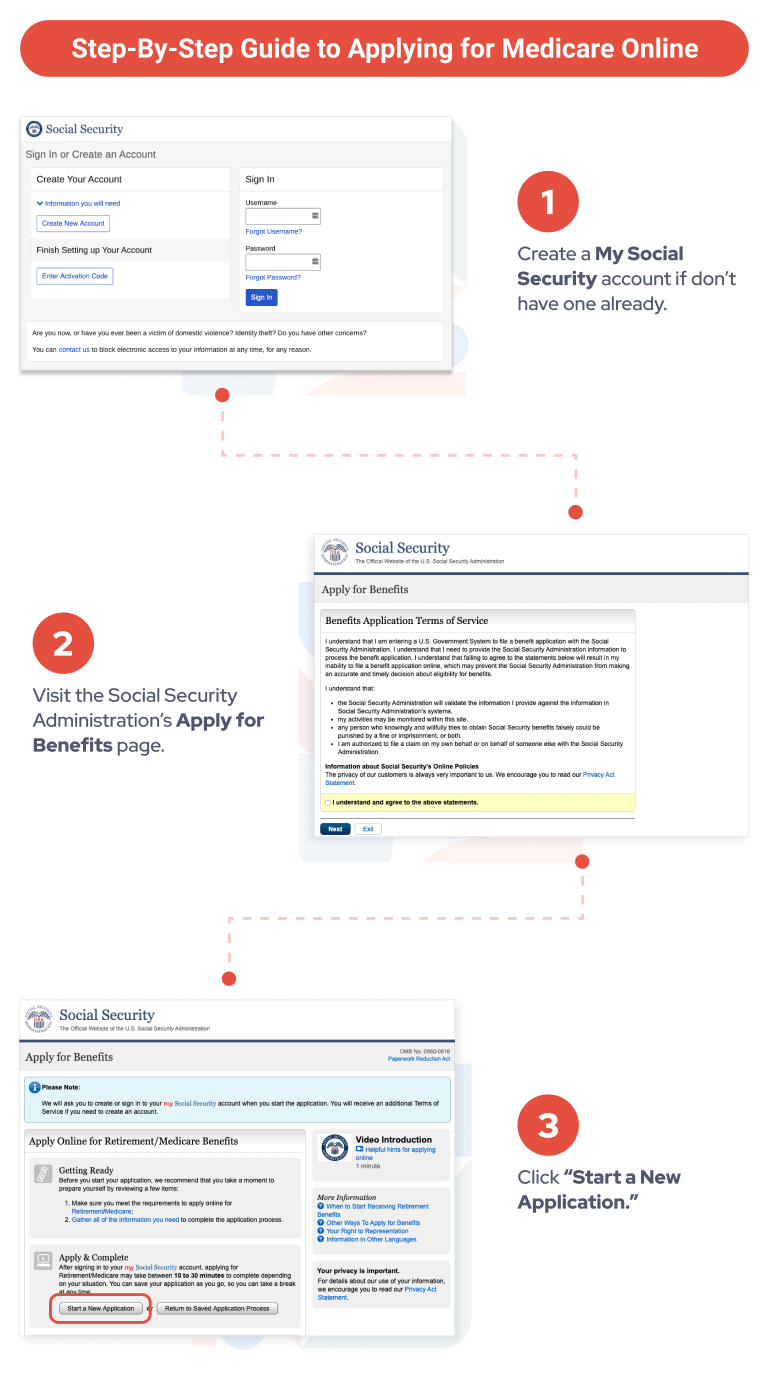
How do I get Started with Medicare?
- Diagnostic and laboratory tests, such as X-rays and blood work
- Medical equipment, such as wheelchairs and hospital beds
- Orthotics (devices that support joints) and prosthetics (artificial body parts)
- Mental health care
- Ambulance services
- Preventive benefits
What month does Medicare start?
Medicare will start 3 months after you sign up: After that time, you can usually only apply during the General Election Period (1/1-3/31) Medicare will start July 1st. NOTE: If you have a qualifying event to enroll in Part B after 65, you will be able to start Medicare right away, and not have to wait until the General Election Period.
When will my Medicare coverage start?
Your Medicare coverage generally starts on the first day of your birthday month. If your birthday falls on the first day of the month, your Medicare coverage starts the first day of the previous month. If you qualify for Medicare because of a disability or illness, in most cases your IEP is also seven months.
When does Medicare enrollment begin?
Usually, a person is eligible to enroll with Medicare when they turn 65. The Initial Enrollment Period (IEP) begins 3 months before a person’s birth month, continues through this month, and ends 3 months after it. Individuals are eligible for Medicare during the IEP, even if they continue working.
How often do Medicare days reset?
The annual deductible will reset each January 1st. How long is each benefit period for Medicare? Each benefit period for Part A starts the day you are hospitalized and ends when you are out for 60 days consecutively.
Does Medicare reset every year?
Your Medicare deductible resets on January 1 of each year. The Medicare deductible is based on each calendar year, meaning that it lasts from January 1-December 31, and then it resets for the new year.
When Medicare runs out what happens?
For days 21–100, Medicare pays all but a daily coinsurance for covered services. You pay a daily coinsurance. For days beyond 100, Medicare pays nothing. You pay the full cost for covered services.
What does Medicare consider a calendar year?
The Medicare Part D plan year runs from January 1st through December 31st of each year, so the plan year runs for a calendar year rather than 365 days from the date of your initial enrollment (or Initial Enrollment Period).
Does Medicare renew automatically?
Medicare cards are valid for 5 years. We'll send you a new card before your old one expires. You don't have to do anything unless your address has changed. If it has, update your details so the card gets to you.
Do Medicare benefits run out?
In general, there's no upper dollar limit on Medicare benefits. As long as you're using medical services that Medicare covers—and provided that they're medically necessary—you can continue to use as many as you need, regardless of how much they cost, in any given year or over the rest of your lifetime.
What is the 3 day rule for Medicare?
The 3-day rule requires the patient have a medically necessary 3-consecutive-day inpatient hospital stay. The 3-consecutive-day count doesn't include the discharge day or pre-admission time spent in the Emergency Room (ER) or outpatient observation.
Where do the elderly live when they have no money?
Low-income seniors over the age of 62 may qualify to live in subsidized housing via HUD's Section 202 program, which covers both independent and assisted living environments. Established in 1959, Section 202 is the only HUD program that provides housing exclusively for seniors.
Is Medicare going away in 2026?
This large and growing income stream can cover things like medical insurance premiums should Medicare truly become insolvent in 2026.
What will Medicare cost in 2023?
CMS finalizes 8.5% rate hike for Medicare Advantage, Part D plans in 2023. The Biden administration finalized an 8.5% increase in rates to Medicare Part D and Medicare Advantage plans, slightly above the 7.98% proposed earlier this year.
What is the difference between plan year and calendar year?
A calendar year deductible, which is what most health plans operate on, begins on January 1st and ends on December 31st. Calendar-year deductibles reset every January 1st. A plan year deductible resets on the renewal date of your company's plan.
How many days are in a Medicare benefit period?
60 daysA benefit period begins the day you're admitted as an inpatient in a hospital or SNF. The benefit period ends when you haven't gotten any inpatient hospital care (or skilled care in a SNF) for 60 days in a row. If you go into a hospital or a SNF after one benefit period has ended, a new benefit period begins.
When does Medicare start?
For most people, Medicare coverage starts the first day of the month you turn 65. Some people delay enrollment and remain on an employer plan. Others may take premium-free Part A and delay Part B. If someone is on Social Security Disability for 24 months, they qualify for Medicare. Those with End-Stage Renal Disease will be immediately eligiblee ...
When do you sign up for unemployment benefits?
It includes your birth month, and it ends three months after your birth month. If you want your benefits to start at the beginning of the month, you turn 65, be sure to sign up at least a month before your birthday. ...
Can you get Medicare if you have ALS?
Those with End-Stage Renal Disease will be immediately eligiblee for Medicare with a diagnosis. When Medicare starts is different for each beneficiary. People with disabilities, ALS, or End-Stage Renal Disease may be eligible for Medicare before they’re 65. If you qualify for Medicare because of a disability, there is no minimum age ...
Is group coverage better than Medicare?
In this scenario, delaying enrollment would make sense, especially if the coverage is better than Medicare. Although, group coverage better than Medicare isn’t the typical scenario. Many people work for small employers;
Can you have Cobra if you don't have Medicare?
So, if you don’t have Medicare, and you only have the group plan, the employer plan won’t pay until your Medicare is active. Further, COBRA is NOT creditable coverage for Medicare. When you delay Part B without creditable coverage, a late enrollment penalty could be coming your way.
When does Medicare open enrollment end?
The Medicare Advantage Open Enrollment Period starts January 1 and ends March 31 every year. During this period, you can switch Medicare Advantage plans or leave a Medicare Advantage plan and return to Original Medicare.
How long does Medicare initial enrollment last?
Your Initial Enrollment period lasts for seven months : It begins three months before you turn 65.
How long does Medicare last?
It includes your birth month. It extends for another three months after your birth month. If you are under 65 and qualify for Medicare due to dis ability, the 7-month period is based around your 25th month of disability benefits.
What happens if you don't sign up for Medicare?
If you don't sign up during your Initial Enrollment Period and if you aren't eligible for a Special Enrollment Period , the next time you can enroll in Medicare is during the Medicare General Enrollment Period.
When is the best time to enroll in Medicare Supplement?
If you have Original Medicare and would like to enroll in a Medicare Supplement Insurance plan (also called Medigap), the best time to sign up is during your six-month Medigap Open Enrollment Period .
How long does it take to switch back to Medicare?
If you sign up for a Medicare Advantage plan during your Initial Enrollment Period, you can change to another Medicare Advantage plan or switch back to Original Medicare within the first 3 months that you have Medicare.
Can you qualify for a special enrollment period?
Depending on your circumstances, you may also qualify for a Special Enrollment Period (SEP). Medicare Special Enrollment Periods can happen at any time during the year. You may qualify for a Special Enrollment Period for a number of reasons, which can include:
Introduction
Are you planning on retiring soon? Then you may want to know: when does Medicare coverage start?
Does Medicare start on my 65th birthday?
You are eligible for Medicare if you are an American (or a US resident for five years) aged 65 and above, or if you are under 65 and have been receiving disability benefits for at least 24 months.
When does Medicare kick in for Original Medicare?
When your coverage under Original Medicare begins, you will have Part A (Hospital) and Part B (Medical) benefits.
When does coverage start under a Medigap plan?
A Medigap plan will help in paying the out-of-pocket costs that you are required to pay under Original Medicare.
What month does Medicare start if I choose a Medicare Advantage plan?
Many seniors enroll in Medicare Advantage (or Part C) plans, in part because of the additional benefits these plans offer. These are the enrollment periods:
When does Medicare coverage start for Part D plans?
You may need a standalone prescription drug plan (PDP) under traditional Medicare. You can enroll during these enrollment periods:
At what age does Medicare start if I continue working?
Most seniors are covered by premium-free Part A if they have contributed Medicare taxes for ten years.
How does Medicare benefit period work?
How Do Medicare Benefit Periods Work? It’s important to understand the difference between Medicare’ s benefit period from the calendar year. A benefit period begins the day you’re admitted to the hospital or skilled nursing facility. In this case, it only applies to Medicare Part A and resets ...
How long does Medicare cover inpatient care?
Part A covers inpatient hospital care, skilled long-term facility, and more, for up to 90 days. But if you ever need to extend your hospital stay, Medicare will cover 60 additional days, called lifetime reserve days. For instance, if your hospital stay lasts over 120 days, you will have used 30 lifetime reserve days.
How long does Medicare Part A deductible last?
In this case, it only applies to Medicare Part A and resets (ends) after the beneficiary is out of the hospital for 60 consecutive days. There are instances in which you can have multiple benefit periods within a calendar year. This means you’ll end up paying a Part A deductible more than once in 12 months.
What is the deductible for Medicare 2021?
Yearly Medicare Deductibles. The calendar-year deductible is what you must pay before Medicare pays its portion, but you will still have coverage until you reach your deductible. In 2021, the deductible for Part A costs $1,484, while Part B’s deductible is $203.
How many Medigap plans are there?
One way to avoid paying for deductibles is by purchasing Medicare Supplement, also called a Medigap plan. There are 12 Medigap plans, letters A-N. Each plan varies by price and benefits. All Medigap plans, with the exception of Plan A, cover the Part A deductible.
Do Medicare Advantage plans have a benefit period?
The Medicare Advantage plans that use benefit periods are typically for skilled nursing facility stays. A large majority of Medicare Advantage plans do not use benefit periods for hospital stays. Most beneficiaries pay a copayment for the first few days. Afterward, you’re required to pay the full amount for each day.
Does Medigap cover Part A?
All Medigap plans, with the exception of Plan A, cover the Part A deductible. Letter plans K, L, & M cover a percentage of the Part A deductible. Only Medigap plans C and F cover the deductible under Part B.
How long does it take for Medicare Part A to renew?
After 60 days Medicare Part A benefits “renew” in that the beneficiary will receive all benefits as if benefits had not been previously received (with the exception of “lifetime reserve days” which do not “renew” and do not apply at all to Skilled Nursing Facility benefits). New deductibles and co-pays will also apply.
What is a benefit period?
What is a “Benefit Period”? A Benefit Period begins the day (overnight) the beneficiary is admitted to a hospital as a Medicare patient and ends when they been out of the hospital or have not received Medicare Skilled Nursing Facility care for at least 60 days in a row.
How long does a skilled nursing facility benefit last?
Remember that just because there is a potential 100 day Skilled Nursing Facility benefit per benefit period it does not mean the beneficiary “automatically” will receive the full 100 days. To continue to receive Medicare Skilled Nursing Facility benefits during the covered 100 days the patient: 1.
How many overnights do you need to be admitted to a skilled nursing facility?
Medicare covers Skilled Nursing Facility care if the following conditions are met: 1. Patient must have spent three overnights as an admitted hospital patient (be wary of “observation” stays in hospital…they do not count toward the three day requirement). 2. Be admitted to a Medicare participating facility. 3.
Does Medicare cover skilled nursing?
Below is a summary of Medicare Skilled Nursing Facility benefits:#N#Medicare covers Skilled Nursing services ONLY. Medicare will not, under any circumstances, pay for Intermediate or Custodial nursing facility care.#N#Medicare Skilled Nursing Facility benefits fall under Medicare Part A.#N#Skilled Nursing and Rehabilitative services are defined as:#N#1. Medically necessary.#N#2. Ordered by a physician.#N#3. Performed by skilled personnel (i.e,, physical therapist, respiratory therapist, occupational therapist, etc.).#N#Medicare covers Skilled Nursing Facility care if the following conditions are met:#N#1. Patient must have spent three overnights as an admitted hospital patient (be wary of “observation” stays in hospital…they do not count toward the three day requirement).#N#2. Be admitted to a Medicare participating facility.#N#3. Be admitted within 30 days of hospital discharge.#N#4. Be admitted for the same condition for which they were hospitalized.#N#If the above conditions are met then for each Benefit Period:#N#1. Medicare will pay all charges for the first 20 days.#N#2. Medicare will pay all charges except for a $161 per day co-pay for the next 80 days (2016). This co-pay may be covered by Medicare supplement or other private insurance.#N#3. Medicare Skilled Nursing Facility benefits end after 100 days of care per Benefit Period.#N#What is a “Benefit Period”?#N#A Benefit Period begins the day (overnight) the beneficiary is admitted to a hospital as a Medicare patient and ends when they been out of the hospital or have not received Medicare Skilled Nursing Facility care for at least 60 days in a row.#N#In other words, Benefit Periods are separated by 60 days during which the Medicare beneficiary has not received care in a hospital or Skilled Nursing Facility.#N#After 60 days Medicare Part A benefits “renew” in that the beneficiary will receive all benefits as if benefits had not been previously received (with the exception of “lifetime reserve days” which do not “renew” and do not apply at all to Skilled Nursing Facility benefits). New deductibles and co-pays will also apply. So, too, will the beneficiary have to again meet the hospital stay requirement.#N#Remember that just because there is a potential 100 day Skilled Nursing Facility benefit per benefit period it does not mean the beneficiary “automatically” will receive the full 100 days.#N#To continue to receive Medicare Skilled Nursing Facility benefits during the covered 100 days the patient:#N#1. Must be able to participate in prescribed therapies.#N#2. Must be willing to participate in prescribed therapies.#N#3. Must be “progressing” in treatment.#N#If the patient stabilizes or “plateaus” in treatment, they may no longer qualify for skilled services and Medicare benefits will terminate…even if the patient is not capable of caring for themselves or they have not received 100 days of coverage.#N#This is where Medicaid comes in as the payee of last resort for nursing home care other than skilled or when Medicare skilled benefits are exhausted.#N#Caveat: The above is applicable to “Original” Medicare. If a beneficiary is covered under a Medicare Advantage Plan (Medicare Part C) actual benefits may vary in terms of co-pays and coverages. Contracts and benefits vary. Consult the contract for details.
When does Medicare deductible reset?
Your Medicare deductible resets on January 1 of each year. The Medicare deductible is based on each calendar year, meaning that it lasts from January 1-December 31, and then it resets for the new year.
How many Medicare Supplement Plans are there?
There is a way to avoid paying Medicare deductibles, which is to have a Medicare Supplement – also called a Medigap plan. There are 11 total Medicare Supplement plans, and each one varies in terms of price and benefits. The 3 most popular plans are Plan F, Plan G, and Plan N, because they provide the most coverage.
How much is Medicare Part A deductible?
This year, the Medicare Part A deductible is $1,408, and the Medicare Part B deductible is $198. So, if you’re on Medicare, you would need to meet these deductibles before Medicare starts covering your medical bills.
Does Medicare Supplement pay for deductible?
However, many of the Medicare Supplement plans help pay for your Medicare deductibles. If you’re on a Medicare Advantage plan, your deductible will vary depending on where you live and which plan you’re enrolled in. Your agent will be able to confirm your plan’s benefits.
What is Medicare benefit period?
Medicare benefit periods mostly pertain to Part A , which is the part of original Medicare that covers hospital and skilled nursing facility care. Medicare defines benefit periods to help you identify your portion of the costs. This amount is based on the length of your stay.
How long does Medicare Advantage last?
Takeaway. Medicare benefit periods usually involve Part A (hospital care). A period begins with an inpatient stay and ends after you’ve been out of the facility for at least 60 days.
How much coinsurance do you pay for inpatient care?
Days 1 through 60. For the first 60 days that you’re an inpatient, you’ll pay $0 coinsurance during this benefit period. Days 61 through 90. During this period, you’ll pay a $371 daily coinsurance cost for your care. Day 91 and up. After 90 days, you’ll start to use your lifetime reserve days.
How long does Medicare benefit last after discharge?
Then, when you haven’t been in the hospital or a skilled nursing facility for at least 60 days after being discharged, the benefit period ends. Keep reading to learn more about Medicare benefit periods and how they affect the amount you’ll pay for inpatient care. Share on Pinterest.
What facilities does Medicare Part A cover?
Some of the facilities that Medicare Part A benefits apply to include: hospital. acute care or inpatient rehabilitation facility. skilled nursing facility. hospice. If you have Medicare Advantage (Part C) instead of original Medicare, your benefit periods may differ from those in Medicare Part A.
How much is Medicare deductible for 2021?
Here’s what you’ll pay in 2021: Initial deductible. Your deductible during each benefit period is $1,484. After you pay this amount, Medicare starts covering the costs. Days 1 through 60.
How long can you be out of an inpatient facility?
When you’ve been out of an inpatient facility for at least 60 days , you’ll start a new benefit period. An unlimited number of benefit periods can occur within a year and within your lifetime. Medicare Advantage policies have different rules entirely for their benefit periods and costs.