Yes, you can have both Medicare and Medicaid Medicaid in the United States is a federal and state program that helps with medical costs for some people with limited income and resources. Medicaid also offers benefits not normally covered by Medicare, including nursing home care and personal care services. The Health Insurance As…Medicaid
Can I have Medicare and Medicaid?
In some cases, it’s possible for someone to have both Medicare AND Medicaid. In order to enroll in both programs, the individual must meet the eligibility requirements for both programs.
How do I qualify for Medicare and Medicaid?
You can qualify for Medicare insurance in three ways: You’ll also need to be an American citizen or permanent legal resident to receive insurance from Medicare. Learn more about Medicare eligibility. If you think you might be eligible, find out about Medicare Open Enrollment. Recipients have several choices for Medicaid health plans.
How many people are eligible for Medicare and Medicaid?
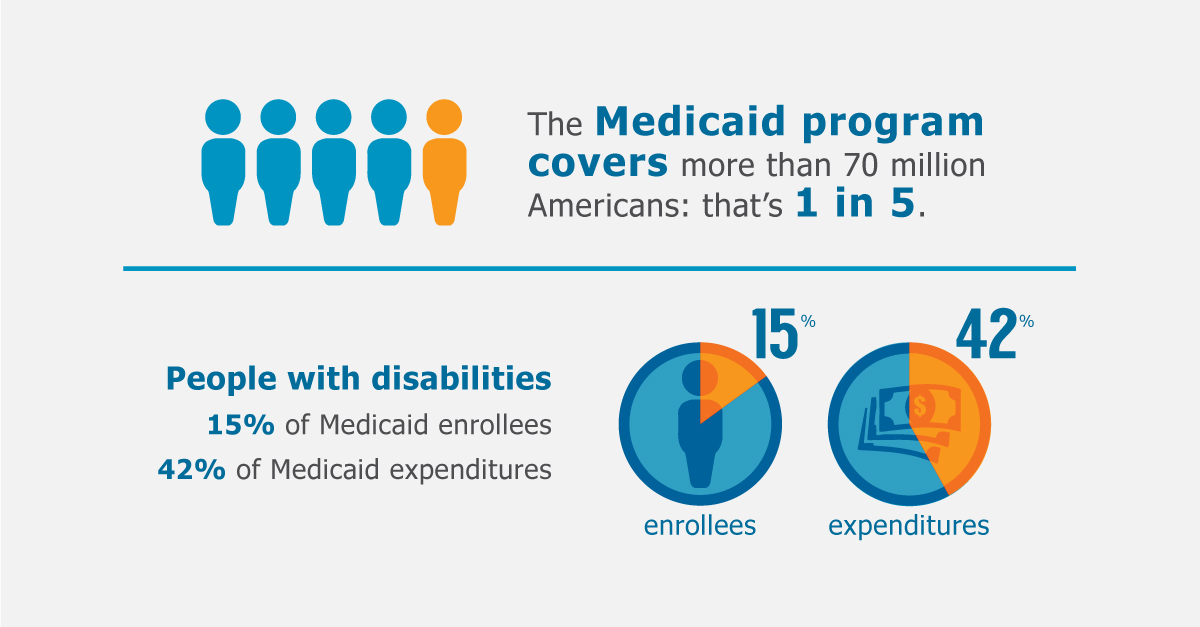
Medicaid also provides coverage to 4.8 million people with disabilities who are enrolled in Medicare. In total, 12 million people are "dually eligible" and enrolled in both Medicaid and Medicare, composing more than 15% of all Medicaid enrollees.
How does Medicaid work with Medicare?
Medicaid, via Medicare Savings Programs, also helps to cover the costs of Medicare premiums, deductibles, and co-payments. Medicaid provides a wide variety of long-term care benefits and supports to allow persons to age at home or in their community.

Is Medicare same thing as Medicaid?
The difference between Medicaid and Medicare is that Medicaid is managed by states and is based on income. Medicare is managed by the federal government and is mainly based on age. But there are special circumstances, like certain disabilities, that may allow younger people to get Medicare.
How do I know if I have Medicare?
You will know if you have Original Medicare or a Medicare Advantage plan by checking your enrollment status. Your enrollment status shows the name of your plan, what type of coverage you have, and how long you've had it. You can check your status online at www.mymedicare.gov or call Medicare at 1-800-633-4227.
Do I automatically get Medicare when I turn 65?
Yes. If you are receiving benefits, the Social Security Administration will automatically sign you up at age 65 for parts A and B of Medicare. (Medicare is operated by the federal Centers for Medicare & Medicaid Services, but Social Security handles enrollment.)
Do you automatically get Medicare with Social Security?
You automatically get Medicare because you're getting benefits from Social Security (or the Railroad Retirement Board). Part B covers certain doctors' services, outpatient care, medical supplies, and preventive services.
What is Medicaid in the US?
Medicaid is a health program provided by individual state governments to people who meet at least one of the income or disability requirements. Nobody is automatically enrolled in Medicaid. To receive it, you must apply through your state’s Medicaid office.
What are the two types of medicaid?
There are two basic types of Medicaid: Fee-For-Service and Managed Medicaid. Fee-For-Service – Medicaid pays doctors, hospitals, and other healthcare providers for the individual services or products received by the Medicaid member. Managed Medicaid (Managed Care Plan) – The state contracts with a private insurance company to manage ...
What is QMB in Medicare?
Qualified Medicare Beneficiary Only (QMB) is a Medicaid-funded program that provides financial assistance to cover Medicare Part A and Part B premiums. It also covers Medicare deductibles, coinsurances, and copays.
What is managed care plan?
Managed Medicaid (Managed Care Plan) – The state contracts with a private insurance company to manage and administer Medicaid benefits. Member benefits will be similar to fee-for-service, but could vary depending on the plan.
How do I know if I have medicaid?
The best way to know which one you have is to call the number on the back of your insurance card.
How many parts are there in Medicare?
About Medicare. Medicare is a national health program provided by the US government. It’s divided into 4 parts: Part A, Part B, Part C, and Part D. Every American who paid into Medicare is automatically enrolled in Part A and Part B when they turn 65. People under 65 with certain disabilities may also apply to enroll.
What is Medicare Part A?
Parts of Medicare. Part A – Covers time spent in a health facility such as a hospital, hospice care, or home health agency. Part B – Covers health expenses such as doctor visits, surgery, medical supplies, lab work, and test screenings. Part C – A combination of Part A and B that can also include dental, vision, prescriptions, ...
Which pays first, Medicare or Medicaid?
Medicare pays first, and. Medicaid. A joint federal and state program that helps with medical costs for some people with limited income and resources. Medicaid programs vary from state to state, but most health care costs are covered if you qualify for both Medicare and Medicaid. pays second.
What is original Medicare?
Original Medicare. Original Medicare is a fee-for-service health plan that has two parts: Part A (Hospital Insurance) and Part B (Medical Insurance). After you pay a deductible, Medicare pays its share of the Medicare-approved amount, and you pay your share (coinsurance and deductibles). or a.
Does Medicare have demonstration plans?
Medicare is working with some states and health plans to offer demonstration plans for certain people who have both Medicare and Medicaid and make it easier for them to get the services they need. They’re called Medicare-Medicaid Plans. These plans include drug coverage and are only in certain states.
Does Medicare Advantage cover hospice?
Medicare Advantage Plans provide all of your Part A and Part B benefits, excluding hospice. Medicare Advantage Plans include: Most Medicare Advantage Plans offer prescription drug coverage. . If you have Medicare and full Medicaid, you'll get your Part D prescription drugs through Medicare.
Can you get medicaid if you have too much income?
Even if you have too much income to qualify, some states let you "spend down" to become eligible for Medicaid. The "spend down" process lets you subtract your medical expenses from your income to become eligible for Medicaid. In this case, you're eligible for Medicaid because you're considered "medically needy."
Can you spend down on medicaid?
Medicaid spenddown. Even if you have too much income to qualify, some states let you "spend down" to become eligible for Medicaid . The "spend down" process lets you subtract your medical expenses from your income to become eligible for Medicaid.
Does Medicare cover prescription drugs?
. Medicaid may still cover some drugs and other care that Medicare doesn’t cover.
How many people are covered by medicaid?
Medicaid also provides coverage to 4.8 million people with disabilities who are enrolled in Medicare.
Can you be covered by Medicare and Medicaid?
Individuals who are enrolled in both Medicaid and Medicare, by federal statute, can be covered for both optional and mandatory categories.
Can Medicare help with out of pocket medical expenses?
Medicare enrollees who have limited income and resources may get help paying for their premiums and out-of-pocket medical expenses from Medicaid (e.g. MSPs, QMBs, SLBs, and QIs).
What is Medicaid in healthcare?
Medicaid is a collection of state-run programs that gives low-income Americans access to affordable care. While their names sound similar, and they both help people pay for health care, Medicare and Medicaid have different eligibility requirements, coverages, and costs. Understanding which you need and how you might qualify for these ...
What is Medicare Part A?
Medicare coverage. Recipients have several choices for Medicaid health plans. Original Medicare consists of Medicare Part A (hospital insurance) and Part B (medical insurance) and provides the basis for all other types of Medicare health insurance plans. Part A covers hospital stays, hospice care, skilled nursing care, and some home health care.
What is dual eligible Medicare?
People who receive both Medicare and Medicaid benefits, usually low-income seniors, are called dual eligible. Many insurance companies provide Medicare Advantage plans, called D-SNPs (Special Needs Plans for Dual Eligible), for people in this situation. If you have both types of benefits, Medicare will pay first.
What are the two government programs that Americans can use to pay for their health care?
Americans have two government programs to turn to when paying their health care costs: Medicare and Medicaid. Medicare is a national health insurance program designed to help people 65 and older and those with disabilities pay their medical bills. Medicaid is a collection of state-run programs that gives low-income Americans access ...
What are mandatory benefits for a nurse practitioner?
Those mandatory benefits include coverage for the following services: Hospital, nursing facility, and home health care. Physician care and lab tests. Family planning, freestanding birth-center, and nurse midwife, services. Certified family and pediatric care by a nurse practitioner.
Does Medicare Advantage cover dental?
Often, Medicare Advantage plans also include coverage for dental work, vision care, hearing aids, and the SilverSneakers fitness program. Medicare Advantage, Medigap, and Part D plans are all provided by private insurance companies but must follow federal guidelines for mandatory benefits and coverage.
Do you have to pay a separate deductible for Medicare?
In addition to a monthly premium, you might have to meet a separate deductible for each plan you have, as well as other costs such as coinsurance and copayments. Learn more about Medicare premiums and deductibles.
What is Medicare and Medicaid?
Differentiating Medicare and Medicaid. Persons who are eligible for both Medicare and Medicaid are called “dual eligibles”, or sometimes, Medicare-Medicaid enrollees. Since it can be easy to confuse the two terms, Medicare and Medicaid, it is important to differentiate between them. While Medicare is a federal health insurance program ...
How to apply for medicaid?
How to Apply. To apply for Medicare, contact your local Social Security Administration (SSA) office. To apply for Medicaid, contact your state’s Medicaid agency. Learn about the long-term care Medicaid application process. Prior to applying, one may wish to take a non-binding Medicaid eligibility test.
How much does Medicare Part B cost?
For Medicare Part B (medical insurance), enrollees pay a monthly premium of $148.50 in addition to an annual deductible of $203. In order to enroll in a Medicare Advantage (MA) plan, one must be enrolled in Medicare Parts A and B. The monthly premium varies by plan, but is approximately $33 / month.
What is dual eligible?
Definition: Dual Eligible. To be considered dually eligible, persons must be enrolled in Medicare Part A, which is hospital insurance, and / or Medicare Part B, which is medical insurance. As an alternative to Original Medicare (Part A and Part B), persons may opt for Medicare Part C, which is also known as Medicare Advantage.
What is the income limit for Medicaid in 2021?
In most cases, as of 2021, the individual income limit for institutional Medicaid (nursing home Medicaid) and Home and Community Based Services (HCBS) via a Medicaid Waiver is $2,382 / month. The asset limit is generally $2,000 for a single applicant.
How old do you have to be to qualify for medicare?
Citizens or legal residents residing in the U.S. for a minimum of 5 years immediately preceding application for Medicare. Applicants must also be at least 65 years old. For persons who are disabled or have been diagnosed with end-stage renal disease or Lou Gehrig’s disease (amyotrophic lateral sclerosis), there is no age requirement. Eligibility for Medicare is not income based. Therefore, there are no income and asset limits.
Does Medicare cover out-of-pocket expenses?
Persons who are enrolled in both Medicaid and Medicare may receive greater healthcare coverage and have lower out-of-pocket costs. For Medicare covered expenses, such as medical and hospitalization, Medicare is always the first payer (primary payer). If Medicare does not cover the full cost, Medicaid (the secondary payer) will cover the remaining cost, given they are Medicaid covered expenses. Medicaid does cover some expenses that Medicare does not, such as personal care assistance in the home and community and long-term skilled nursing home care (Medicare limits nursing home care to 100 days). The one exception, as mentioned above, is that some Medicare Advantage plans cover the cost of some long term care services and supports. Medicaid, via Medicare Savings Programs, also helps to cover the costs of Medicare premiums, deductibles, and co-payments.