Do you qualify for a special enrollment period?
Jun 01, 2020 · A Special Enrollment Period is a time that you are allowed to sign up for a health insurance plan outside the traditional enrollment periods. In most cases, you are eligible to sign up for Medicare coverage during your Initial Enrollment Period, which generally occurs when a person reaches the age of 65, or qualify under the age of 65 with certain disabilities.
What are Medicare Special Enrollment periods (SEPs)?
Jun 07, 2021 · Special Enrollment Period (SEP) If you are age 65 or older, you or your spouse are still working and you are covered under a group health plan based on that current employment, you may not need to apply for Medicare medical insurance (Part B) at age 65. You may qualify for a "Special Enrollment Period" (SEP) that will let you sign up for Part B: During any month you …
Do you qualify for Medicare Special Enrollment for Original Medicare?
Nov 24, 2021 · If you did not enroll in Medicare when you turned 65 because you were still employed and were covered by your employer’s health insurance plan, you will be granted a Special Enrollment Period. This allows you to enroll in Medicare once you leave your employer coverage, even if you work past the age of 65, the qualifying age for Medicare.
What is a Tricare special enrollment period?

Which of the following is a qualifying life event for a Medicare Advantage Special Enrollment Period?
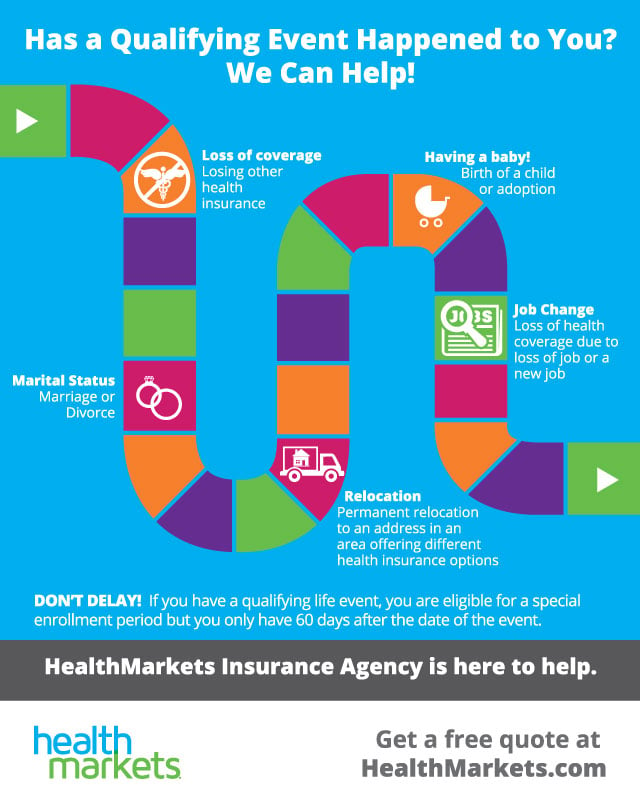
You qualify for a Special Enrollment Period if you've had certain life events, including losing health coverage, moving, getting married, having a baby, or adopting a child, or if your household income is below a certain amount.
What is an SEP for Medicare?
You can make changes to your Medicare Advantage and Medicare prescription drug coverage when certain events happen in your life, like if you move or you lose other insurance coverage. These chances to make changes are called Special Enrollment Periods (SEPs).
What is the special enrollment period for Medicare Part B?
8 monthsWhat is the Medicare Part B special enrollment period (SEP)? The Medicare Part B SEP allows you to delay taking Part B if you have coverage through your own or a spouse's current job. You usually have 8 months from when employment ends to enroll in Part B.Mar 7, 2020
What qualifies as a life changing event for Medicare?
A change in your situation — like getting married, having a baby, or losing health coverage — that can make you eligible for a Special Enrollment Period, allowing you to enroll in health insurance outside the yearly Open Enrollment Period.
Are you automatically enrolled in Medicare if you are on Social Security?
Yes. If you are receiving benefits, the Social Security Administration will automatically sign you up at age 65 for parts A and B of Medicare. (Medicare is operated by the federal Centers for Medicare & Medicaid Services, but Social Security handles enrollment.)
What is the difference between Medicare IEP and Icep?
The ICEP is a Medicare Advantage enrollment period as defined in Chapter 2 of the Medicare Managed Care Manual. The IEP is a drug benefit enrollment period as defined in Chapter 3 of the Medicare Prescription Drug Benefit Manual.
Can I switch from Medicare Advantage to original Medicare?
Yes, you can elect to switch to traditional Medicare from your Medicare Advantage plan during the Medicare Open Enrollment period, which runs from October 15 to December 7 each year. Your coverage under traditional Medicare will begin January 1 of the following year.
How do you pay for Medicare Part B if you are not collecting Social Security?
If you have Medicare Part B but you are not receiving Social Security or Railroad Retirement Board benefits yet, you will get a bill called a “Notice of Medicare Premium Payment Due” (CMS-500). You will need to make arrangements to pay this bill every month.
Does Medicare coverage start the month you turn 65?
For most people, Medicare coverage starts the first day of the month you turn 65. Some people delay enrollment and remain on an employer plan. Others may take premium-free Part A and delay Part B. If someone is on Social Security Disability for 24 months, they qualify for Medicare.
What is a qualifying event?
A qualifying event is a change in life circumstances that allows you to alter an existing health insurance policy, or sign up for a new one, outside of open enrollment periods. Without a qualifying event, you would need to wait until the next open enrollment period before making any changes.
What is considered a life changing event for Social Security?
A beneficiary who has experienced a life-changing event that caused a significant reduction in MAGI may request SSA to make a new initial determination using a more recent tax year than the tax year used previously. A life changing event can be one or more of the following eight events: Death of Spouse. Marriage.Nov 30, 2010
Can you switch Medicare plans anytime?
If you're covered by both Medicare and Medicaid, you can switch plans at any time during the year. This applies to Medicare Advantage as well as Medicare Part D.
What is a special enrollment period?
A Special Enrollment Period is a time that you are allowed to sign up for a health insurance plan outside the traditional enrollment periods. In most cases, you are eligible to sign up for Medicare coverage during your Initial Enrollment Period, which generally occurs when a person reaches the age of 65, or qualify under the age ...
How long can you be in foster care after birth?
In this situation, you are eligible to receive coverage the same day that you apply. You can enroll in care up to 60 days following the event. Divorce, legal separation, and lost health insurance because of it.
How long does it take to change health insurance after getting married?
If this is the case, you must select a plan by the last day of the month within 60 days of the marriage. Coverage will then begin the first day of the following month.
How old do you have to be to get Medicare?
If you are age 65 or older, you or your spouse are still working and you are covered under a group health plan based on that current employment, you may not need to apply for Medicare medical insurance (Part B) at age 65. You may qualify for a "Special Enrollment Period" (SEP) that will let you sign up for Part B: 1 During any month you remain covered under the group health plan and your, or your spouse's, current employment continues; or 2 In the eight-month period that begins with the month after your group health plan coverage or the current employment it is based on ends, whichever comes first.#N#Exception: If your group health plan coverage or the employment it is based on ends during your initial enrollment period for Medicare Part B, you do not qualify for a SEP. Your initial enrollment period starts three months before the month you attain age 65 and ends three months after the month you turn 65. 3 If your group health plan coverage is based on severance or retirement pay and the job your coverage is based on ended in the last eight months.
When does the enrollment period start for a group health plan?
Your initial enrollment period starts three months before the month you attain age 65 and ends three months after the month you turn 65. If your group health plan coverage is based on severance or retirement pay and the job your coverage is based on ended in the last eight months.
What is a SEP in health insurance?
You may qualify for a "Special Enrollment Period" (SEP) that will let you sign up for Part B: During any month you remain covered under the group health plan and your, or your spouse's, current employment continues; or.
Can I get a SEP if I have Social Security?
If you have that type of coverage, you will not be eligible for a SEP when it ends. To avoid paying a higher premium, make sure you sign up for Medicare when you are first eligible. People who receive Social Security disability benefits and are covered under a group health plan from either their own or a family member's current employment also have ...
What is a special enrollment period?
A Special Enrollment Period (SEP) is an enrollment period that takes place outside of the annual Medicare enrollment periods, such as the annual Open Enrollment Period. They are granted to people who were prevented from enrolling in Medicare during the regular enrollment period for a number of specific reasons.
When is the open enrollment period for Medicare?
Learn more and use this guide to help you sign up for Medicare. Open Enrollment: The fall Medicare Open Enrollment Period has officially begun and lasts from October 15 to December 7, 2020. You may be able to enroll in ...
How long do you have to disenroll from Medicare Advantage?
If you enrolled in a Medicare Advantage plan when you first became eligible for Medicare, you have 12 months to disenroll from the plan and transition back to Original Medicare.
What happens if you don't enroll in Medicare at 65?
If you did not enroll in Medicare when you turned 65 because you were still employed and were covered by your employer’s health insurance plan, you will be granted a Special Enrollment Period.
How long does Medicare Advantage coverage last?
If you had a Medicare Advantage plan with prescription drug coverage which met Medicare’s standards of “creditable” coverage and you were to lose that coverage through no fault of your own, you may enroll in a new Medicare Advantage plan with creditable drug coverage beginning the month you received notice of your coverage change and lasting for two months after the loss of coverage (or two months after receiving the notice, whichever is later).
How often can you change your Medicare Advantage plan?
If you move into, out of, or currently reside in a facility of special care such as a skilled nursing home or long-term care hospital, you may enroll in, disenroll from, or change a Medicare Advantage plan one time per month.
What to do if you don't fit into Medicare?
If your circumstances do not fit into any of the Special Enrollment Periods described above, you may ask the Centers for Medicare and Medicaid Services (CMS) for your own Special Enrollment Period based on your situation.
