Medicare and Medicaid: Dual eligibility
- Eligibility for Medicare. The usual way to qualify for Medicare is to be 65 years of age. ...
- Eligibility for Medicaid. Eligibility for Medicaid depends on the region where a person lives, as some states have different criteria for qualification.
- Dual eligibility. ...
- Geographical variations. ...
- Summary. ...
Full Answer
Does Someone on Medicaid automatically qualify for Medicare?
Feb 11, 2022 · Persons who are eligible for both Medicare and Medicaid are called “dual eligibles”, or sometimes, Medicare-Medicaid enrollees. To be considered dually eligible, persons must be enrolled in Medicare Part A (hospital insurance), and / or Medicare Part B (medical insurance).
How much can you make to qualify for Medicare?
You can see if you qualify for Medicaid 2 ways: Visit your state's Medicaid website. Use the drop-down menu at the top of this page to pick your state. You can apply right now and find out if you qualify. If you qualify, coverage can begin immediately. Fill out an application in the Health Insurance Marketplace. When you finish the application, we'll tell you which programs you and …
How does Medicare compare to Medicaid?
Nov 18, 2021 · If you qualify for both Medicare and Medicaid, you can have them both simultaneously. When you have both it means that you are unlikely to have any out-of-pocket medical expenses. Around 20 percent of Medicare beneficiaries are also eligible for Medicaid. They are called dual-eligible.
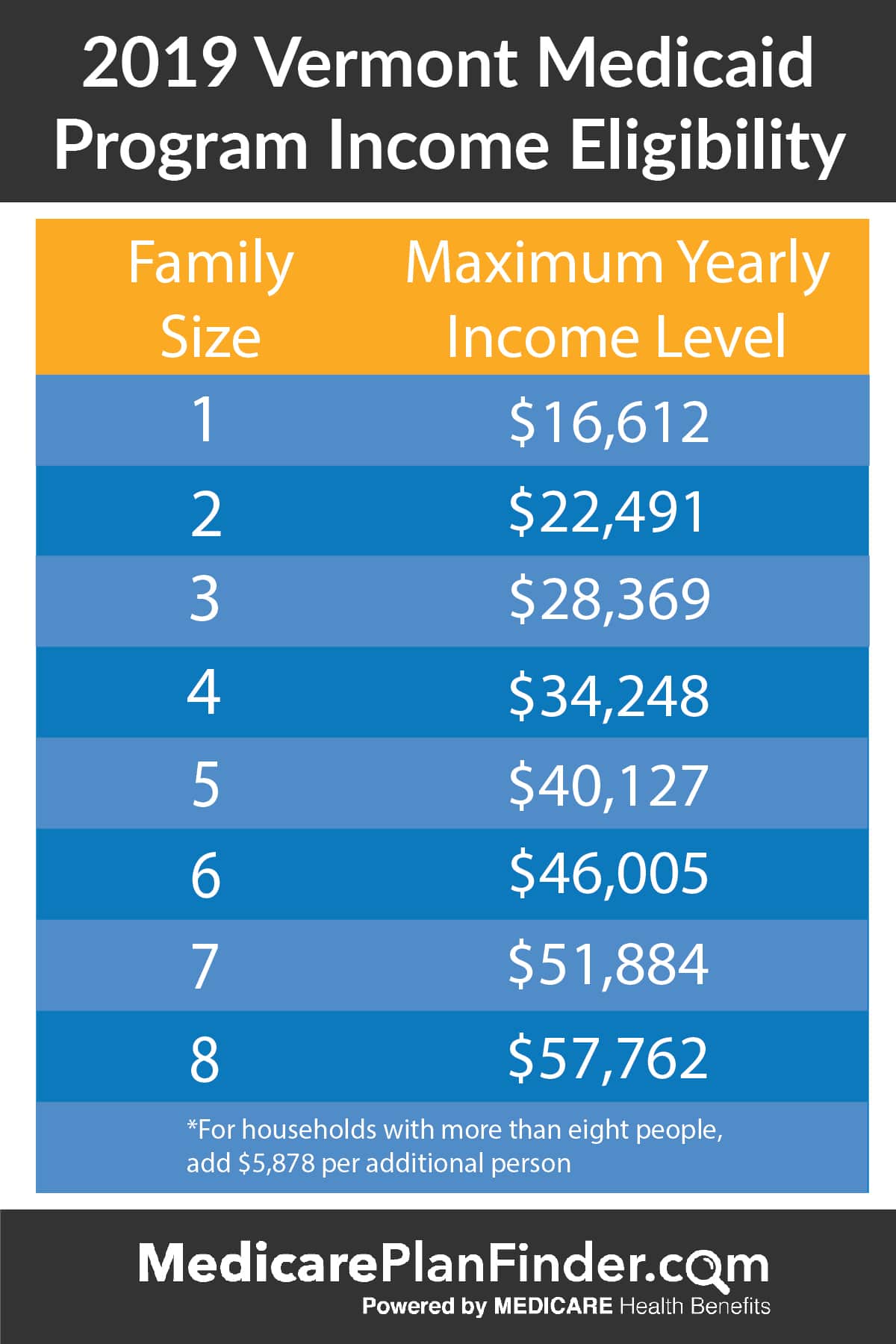
What's the income level requirement to qualify for Medicaid?
Beneficiaries qualify for full Medicaid benefits if their incomes and assets are even lower (but the exact amounts vary by state). Many seniors who live in nursing homes are dual eligible: they qualify for Medicare based on their age, and Medicaid because of their financial circumstances.
What is medicaid?
Medicaid is a joint federal and state program that: 1 Helps with medical costs for some people with limited income and resources 2 Offers benefits not normally covered by Medicare, like nursing home care and personal care services
What is original Medicare?
Original Medicare. Original Medicare is a fee-for-service health plan that has two parts: Part A (Hospital Insurance) and Part B (Medical Insurance). After you pay a deductible, Medicare pays its share of the Medicare-approved amount, and you pay your share (coinsurance and deductibles). or a.
What is extra help?
And, you'll automatically qualify for. Extra Help. A Medicare program to help people with limited income and resources pay Medicare prescription drug program costs, like premiums, deductibles, and coinsurance. paying for your.
Does Medicare cover prescription drugs?
. Medicaid may still cover some drugs and other care that Medicare doesn’t cover.
Does medicaid pay first?
Medicaid programs vary from state to state, but most health care costs are covered if you qualify for both Medicare and Medicaid. pays second. Medicaid never pays first for services covered by Medicare. It only pays after Medicare, employer group health plans, and/or Medicare Supplement (Medigap) Insurance have paid.
Does Medicare have demonstration plans?
Medicare is working with some states and health plans to offer demonstration plans for certain people who have both Medicare and Medicaid and make it easier for them to get the services they need. They’re called Medicare-Medicaid Plans. These plans include drug coverage and are only in certain states.
Can you get medicaid if you have too much income?
Even if you have too much income to qualify, some states let you "spend down" to become eligible for Medicaid. The "spend down" process lets you subtract your medical expenses from your income to become eligible for Medicaid. In this case, you're eligible for Medicaid because you're considered "medically needy."
Who are the dual-eligible recipients?
People who are dual-eligible for Medicare and Medicaid are referred to as dual-eligible beneficiaries. Moreover, each state determines Medicaid coverage, and as a result, Medicaid benefits may differ.
Medicare Ineligibility
The Medicare eligibility requirement is that you must be 65 years old or older. If you or your spouse are 65 years old or older and have paid enough Medicare taxes through previous employment, you or your spouse may be eligible for premium-free Part A of the Medicare program (hospital coverage).
Medicaid Ineligibility
Medicaid eligibility varies depending on where a person resides, as various states have different qualifications.
Dual eligibility
A person must qualify for either partial-dual or full-dual coverage to be eligible for both Medicare and Medicaid.
Variations in geography
Medicaid benefits and coverage vary from one state to the next, and there are differences between them. Depending on the state, Medicaid coverage may be available to those who earn more than the standard income limits.
Medicare Part D Extra Assistance Program
Aside from Medicaid, many other programs assist with medical expenses, and government sponsors them. Extra Help, a program that assists Medicare Part D enrollees with their prescription drug costs, can be applied for by a qualified individual.
Summary
A person’s health and income level may qualify them for both Medicare and Medicaid.
What is dual eligible for Medicare?
Eligibility for the Medicare Savings Programs, through which Medicaid pays Medicare premiums, deductibles, and/or coinsurance costs for beneficiaries eligible for both programs (often referred to as dual eligibles) is determined using SSI methodologies..
What is Medicaid coverage?
Medicaid is the single largest source of health coverage in the United States. To participate in Medicaid, federal law requires states to cover certain groups of individuals. Low-income families, qualified pregnant women and children, and individuals receiving Supplemental Security Income (SSI) are examples of mandatory eligibility groups (PDF, ...
How many people are covered by medicaid?
Medicaid is a joint federal and state program that, together with the Children’s Health Insurance Program (CHIP), provides health coverage to over 72.5 million Americans, including children, pregnant women, parents, seniors, and individuals with disabilities. Medicaid is the single largest source of health coverage in the United States.
What is MAGI for Medicaid?
MAGI is the basis for determining Medicaid income eligibility for most children, pregnant women, parents, and adults. The MAGI-based methodology considers taxable income and tax filing relationships to determine financial eligibility for Medicaid. MAGI replaced the former process for calculating Medicaid eligibility, ...
How long does medicaid last?
Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
Do you have to be a resident to get medicaid?
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
Can you get medicaid if you are medically needy?
Medically Needy. States have the option to establish a “medically needy program” for individuals with significant health needs whose income is too high to otherwise qualify for Medicaid under other eligibility groups. Medically needy individuals can still become eligible by “spending down” the amount of income that is above a state's medically ...
What is the difference between Medicare and Medicaid?
The benefit is the plan will have very low copays and very few additional fees. Medicare is for those aged 65 and older or those with disabilities or specific medical conditions. Medicaid is for people of any age, with or without medical conditions, so long as they meet the state’s economic conditions.
What is Medicare for 65?
Medicare coverage is for adults 65 and older and those with certain qualifying medical conditions or disabilities. To qualify, you would need proof of age, proof of income (to determine how much your deductible is), residency or citizenship documentation, and more. Since Medicare is a government insurance program, ...
How are Medicare premiums paid?
Premiums are typically paid on a monthly basis. In the federal Medicare program, there are four different types of premiums. ... , deductibles, copays, and more. Medicaid assists with these costs, but you may be required to use an approved Medicaid health plan.
Does Medicare cover skilled nursing?
Medicare covers most of the costs associated with skilled nursing after an inpatient stays in the hospital. If you have both Medicare and Medicaid, a stay at a skilled nursing facility will cost very little. After inpatient treatment, many patients need more outpatient care in the home setting.
What is Medicare Advantage?
Medicare Advantage (MA), also known as Medicare Part C, are health plans from private insurance companies that are available to people eligible for Original Medicare ( Medicare Part A and Medicare Part B).... . Some smaller, rural counties may not have SNP plans but will have a local Medicaid plan.
What is deductible insurance?
A deductible is an amount a beneficiary must pay for their health care expenses before the health insurance policy begins to pay its share. ... Coinsurance is a percentage of the total you are required to pay for a medical service. ... , and copays, are the beneficiary’s responsibility.
Is Medicaid a federal or state program?
While Medicaid is both a state and federal program, it is administered at the state level and each state has its own rules and benefits. All Medicaid programs must follow the same federal guidelines while being directed and managed at the local state level.
What is dual eligible Medicare?
Beneficiaries with Medicare and Medicaid are known as dual eligibles – and account for about 20 percent of Medicare beneficiaries (12.1 million people). Dual eligibles are categorized based on whether they receive partial or full Medicaid benefits. Full-benefit dual eligibles have comprehensive Medicaid coverage, ...
What is a dual eligible special needs plan?
If you are dual eligible, you are can enroll in a dual eligible special needs plan (D-SNP) that covers both Medicare and Medicaid benefits. These plans may also pay for expenses that Medicare and Medicaid don’t over individually, including over-the-counter items, hearing aids, and vision or dental care. Beneficiaries who are dual eligible can ...
Is Medicare the same as Medicaid?
The federal government oversees Medicare eligi bility – meaning it is the same in each state. But states set their own eligibility rules for Medicaid and the MSPs (within federal guidelines) – and income limits for these programs vary widely.
Does Medicare cover long term care?
But this is not the case for things Medicare doesn’t cover, like long-term care . If Medicaid is covering a beneficiary’s long-term care, Medicare will still be the primary payer for any Medicare-covered services – like skilled nursing care or physical therapy.
Do seniors qualify for medicaid?
Many seniors who live in nursing homes are dual eligible: they qualify for Medicare based on their age, and Medicaid because of their financial circumstances.
Who is Josh Schultz?
Josh Schultz has a strong background in Medicare and the Affordable Care Act. He coordinated a Medicare ombudsman contract at the Medicare Rights Center in New York City, and represented clients in extensive Medicare claims and appeals.
What is dual eligible for medicaid?
Qualifications for Medicaid vary by state, but, generally, people who qualify for full dual eligible coverage are recipients of Supplemental Security Income (SSI). The SSI program provides cash assistance to people who are aged, blind, or disabled to help them meet basic food and housing needs.
What is Medicaid managed care?
Medicaid managed care is similar to Medicare Advantage, in that states contract with private insurance health plans to manage and deliver the care. In some states, the Medicaid managed care plan is responsible for coordinating the Medicare and Medicaid services and payments.
What is dual eligible?
The term “full dual eligible” refers to individuals who are enrolled in Medicare and receive full Medicaid benefits. Individuals who receive assistance from Medicaid to pay for Medicare premiums or cost sharing* are known as “partial dual eligible.”.
What is Medicare Advantage?
Medicare Advantage plans are private insurance health plans that provide all Part A and Part B services. Many also offer prescription drug coverage and other supplemental benefits. Similar to how Medicaid works with Original Medicare, Medicaid wraps around the services provided by the Medicare Advantage plan andserves as a payer of last resort.
Is Medicaid a payer of last resort?
Medicaid is known as the “payer of last resort.”. As a result, any health care services that a dual eligible beneficiary receives are paid first by Medicare, and then by Medicaid.
Does Medicare cover Part A and Part B?
Some Medicare beneficiaries may choose to receive their services through the Original Medicare Program. In this case, they receive the Part A and Part B services directly through a plan administered by the federal government, which pays providers on a fee-for-service (FFS) basis. In this case, Medicaid would “wrap around” Medicare coverage by paying for services not covered by Medicare or by covering premium and cost-sharing payments, depending on whether the beneficiary is a full or partial dual eligible.
What is a PACE plan?
Similar to D-SNPs, PACE plans provide medical and social services to frail and elderly individuals (most of whom are dual eligible). PACE operates through a “health home”-type model, where an interdisciplinary team of health care physicians and other providers work together to provide coordinated care to the patient. PACE plans also focus on helping enrollees receive care in their homes or in the community, with the goal of avoiding placement in nursing homes or other long-term care institutions.

Who Are The Dual-Eligible Recipients?
Medicare Ineligibility
- The Medicare eligibility requirement is that you must be 65 years old or older. If you or your spouse are 65 years old or older and have paid enough Medicare taxes through previous employment, you or your spouse may be eligible for premium-free Part A of the Medicare program (hospital coverage). They may also be eligible for Medicare Part B, covering doctor visits and var…
Medicaid Ineligibility
- Medicaid eligibility varies depending on where a person resides, as various states have different qualifications. Every year, Medicaid rules may change. The Federal Poverty Level (FPL), which the Department of Health and Human Services (HHS) determines every year, is used to determine a person’s eligibility for a variety of government benefits. In addition to the 48 contiguous states a…
Dual Eligibility
- A person must qualify for either partial-dual or full-dual coverage to be eligible for both Medicare and Medicaid. The amount of Medicaid assistance a person receives determines their eligibility for partial-dual coverage. The following are some examples of various coverage: 1. The premium for Part A (if applicable) 2. The premium for Part B 3. Coinsurances 4. Copayments 5. Deductible…
Variations in Geography
- Medicaid benefits and coverage vary from one state to the next, and there are differences between them. Depending on the state, Medicaid coverage may be available to those who earn more than the standard income limits. The Medicaid website can assist a person in determining which services are available to them in their area based on their geographic location.
Medicare Part D Extra Assistance Program
- Aside from Medicaid, many other programs assist with medical expenses, and government sponsors them. Extra Help, a program that assists Medicare Part D enrollees with their prescription drug costs, can be applied for by a qualified individual. To be eligible for Extra Help, a person’s combined investments, real estate property, and savings must total no more than $29,1…
Summary
- A person’s health and income level may qualify them for both Medicare and Medicaid. Meanwhile, Medicare will generally cover healthcare costs initially, and Medicaid assists with out-of-pocket and non-covered expenses. Medicaid eligibility varies by state, as well as the income level restrictions.
Determining Eligibility For Medicaid
- Financial Eligibility
The Affordable Care Act established a new methodology for determining income eligibility for Medicaid, which is based on Modified Adjusted Gross Income (MAGI). MAGI is used to determine financial eligibility for Medicaid, CHIP, and premium tax credits and cost sharing reductions avail… - Non-Financial Eligibility
To be eligible for Medicaid, individuals must also meet certain non-financial eligibility criteria. Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, suc…
Medically Needy
- States have the option to establish a “medically needy program” for individuals with significant health needs whose income is too high to otherwise qualify for Medicaid under other eligibility groups. Medically needy individuals can still become eligible by “spending down” the amount of income that is above a state's medically needy income standard. Individuals spend down by incu…
Appeals
- States must provide individuals the opportunity to request a fair hearing regarding a denial, an action taken by the state agency that he or she believes was erroneous, or if the state has not acted with reasonable promptness. States have options for how to structure their appeals processes. Appeals may be conducted by the Medicaid agency or delegated to the Exchange or …
Related Topics
- Spousal Impoverishment: Protects the spouse of a Medicaid applicant or beneficiary who needs coverage for long-term services and supports (LTSS), in either an institution or a home or other community-based setting, from becoming impoverished in order for the spouse in need of LTSS to attain Medicaid coverage for such services. Treatment of Trusts: When an individual, his or her s…