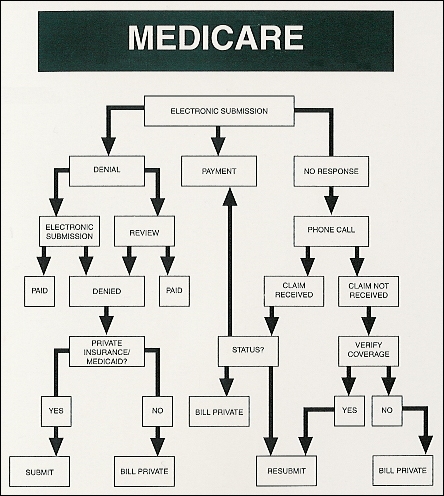
If you’re on Medicare, your doctors will usually bill Medicare for any care you obtain. Medicare will then pay its rate directly to your doctor. Your doctor will only charge you for any copay, deductible, or coinsurance you owe.
What are the requirements for Medicare billing?
- The regular physician is unavailable to provide the service.
- The beneficiary has arranged or seeks to receive the services from the regular physician.
- The locum tenens is NOT an employee of the regular physician.
- The regular physician pays the locum tenens physician on a per diem or fee-for-service basis.
How do I become a Medicare Biller?
What Is an Insurance Biller?
- Get Trained. Formal training in insurance billing is available at vocational schools and community colleges in the form of diploma, certificate and associate's degree programs.
- Obtain Certification. Licensure is not required for insurance billers; however, obtaining professional certification is highly recommended.
- Acquire Work Experience. ...
What is the Medicare process and how does it work?
The amount you must pay for health care or prescriptions before Original Medicare, your prescription drug plan, or your other insurance begins to pay. ) before Medicare pays its share. Then, Medicare pays its share, and you pay your share (. An amount you may be required to pay as your share of the cost for services after you pay any deductibles.
How to bill Medicare as a provider?
Providers that bill institutional claims are also permitted to submit claims electronically via direct data entry (DDE) screens. How Electronic Claims Submission Works: The claim is electronically transmitted from the provider's computer to the MAC.

What is the billing process for Medicare?
Billing for Medicare When a claim is sent to Medicare, it's processed by a Medicare Administrative Contractor (MAC). The MAC evaluates (or adjudicates) each claim sent to Medicare, and processes the claim. This process usually takes around 30 days.
Does Medicare pay all your bills?
En español | Medicare covers some but not all of your health care costs. Depending on which plan you choose, you may have to share in the cost of your care by paying premiums, deductibles, copayments and coinsurance. The amount of some of these payments can change from year to year.
Do doctors bill Medicare directly?
Payment for Medicare-covered services is based on the Medicare Physicians' Fee Schedule, not the amount a provider chooses to bill for the service. Participating providers receive 100 percent of the Medicare Allowed Amount directly from Medicare.
How are Medicare premiums billed?
All Medicare bills are due on the 25th of the month. In most cases, your premium is due the same month that you get the bill. Example of our billing timeline. For your payment to be on time, we must get your payment by the due date on your bill.
Does Medicare pay 100 percent of hospital bills?
According to the Centers for Medicare and Medicaid Services (CMS), more than 60 million people are covered by Medicare. Although Medicare covers most medically necessary inpatient and outpatient health expenses, Medicare reimbursement sometimes does not pay 100% of your medical costs.
What will Medicare not pay for?
In general, Original Medicare does not cover: Long-term care (such as extended nursing home stays or custodial care) Hearing aids. Most vision care, notably eyeglasses and contacts. Most dental care, notably dentures.
Do doctors lose money on Medicare patients?
Summarizing, we do find corroborative evidence (admittedly based on physician self-reports) that both Medicare and Medicaid pay significantly less (e.g., 30-50 percent) than the physician's usual fee for office and inpatient visits as well as for surgical and diagnostic procedures.
How do doctors get reimbursed from Medicare?
Traditional Medicare reimbursements Instead, the law states that providers must send the claim directly to Medicare. Medicare then reimburses the medical costs directly to the service provider. Usually, the insured person will not have to pay the bill for medical services upfront and then file for reimbursement.
How long does it take for Medicare to pay a claim?
For clean claims that are submitted electronically, they are generally paid within 14 calendar days by Medicare. The processing time for clean paper claims is a bit longer, usually around 30 days.
How much does Social Security take out for Medicare each month?
In 2021, based on the average social security benefit of $1,514, a beneficiary paid around 9.8 percent of their income for the Part B premium. Next year, that figure will increase to 10.6 percent.
Why is my Medicare bill so high?
Medicare Part B covers doctor visits, and other outpatient services, such as lab tests and diagnostic screenings. CMS officials gave three reasons for the historically high premium increase: Rising prices to deliver health care to Medicare enrollees and increased use of the health care system.
How often do I pay my Medicare Part B premium?
each monthYou pay a premium each month for Part B. Your Part B premium will be automatically deducted from your benefit payment if you get benefits from one of these: Social Security. Railroad Retirement Board.
How does Medicare work?
How Medicare Billing Works. Medicare was designed in 1965 as a single payer health system that is publicly funded. The funds to pay for Medicare services are collected from employers and self-employed individuals. The Federal Insurance Contributions Act taxes employers and employees a total of 2.9% of an individual’s income.
Why do doctors bill Medicare for services that were not rendered?
Because there is no direct oversight of Medicare’s billing system doctors, sometimes in concert with patients, bill Medicare for services that were not rendered in order to get a larger reimbursement.
What is single payer health care?
In a single payer health system, providers receive payment for services rendered from a general pool of funds that everyone contributes to through taxes. The Medicare program has established a long list of services they will cover and the fee that Medicare will pay to a provider for a service provided to a beneficiary.
How much does Medicare pay for non-participating providers?
Non-participating Medicare providers will receive 80% of the Medicare determined fee and are allowed to bill 15% or more of the remaining amount to the beneficiary. Medicare billing works differently ...
How much did Medicare cost in 2008?
As of 2008 Medicare cost the American public $386 billion which was roughly 13% of the total federal budget. While Medicare is project to take up only 12.5% of the federal budget in 2010, costs will rise to $452 billion.
How much does the Federal Insurance Contributions Act tax?
The Federal Insurance Contributions Act taxes employers and employees a total of 2.9% of an individual’s income. Employees pay 1.45% and employers pay a matching 1.45% tax. Self employed individuals must pay the entire 2.9% tax themselves to contribute to the Medicare program.
Is Medicare billing wheel chairs fraudulent?
Other fraudulent schemes include billing Medicare for durable medical goods such as wheel chairs multiple times for just one chair, and never even delivering the wheel chair. Medicare billing has become a hot button topic in the United States. A lack of oversight on billing combined with ever increasing costs for medical services is causing ...
What is a medical biller?
In general, the medical biller creates claims like they would for Part A or B of Medicare or for a private, third-party payer. The claim must contain the proper information about the place of service, the NPI, the procedures performed and the diagnoses listed. The claim must also, of course, list the price of the procedures.
What form do you need to bill Medicare?
If a biller has to use manual forms to bill Medicare, a few complications can arise. For instance, billing for Part A requires a UB-04 form (which is also known as a CMS-1450). Part B, on the other hand, requires a CMS-1500. For the most part, however, billers will enter the proper information into a software program and then use ...
What is 3.06 Medicare?
3.06: Medicare, Medicaid and Billing. Like billing to a private third-party payer, billers must send claims to Medicare and Medicaid. These claims are very similar to the claims you’d send to a private third-party payer, with a few notable exceptions.
How long does it take for Medicare to process a claim?
The MAC evaluates (or adjudicates) each claim sent to Medicare, and processes the claim. This process usually takes around 30 days .
Is it harder to bill for medicaid or Medicare?
Billing for Medicaid. Creating claims for Medicaid can be even more difficult than creating claims for Medicare. Because Medicaid varies state-by-state, so do its regulations and billing requirements. As such, the claim forms and formats the biller must use will change by state. It’s up to the biller to check with their state’s Medicaid program ...
Can you bill Medicare for a patient with Part C?
Because Part C is actually a private insurance plan paid for, in part, by the federal government, billers are not allowed to bill Medicare for services delivered to a patient who has Part C coverage. Only those providers who are licensed to bill for Part D may bill Medicare for vaccines or prescription drugs provided under Part D.
Do you have to go through a clearinghouse for Medicare and Medicaid?
Since these two government programs are high-volume payers, billers send claims directly to Medicare and Medicaid. That means billers do not need to go through a clearinghouse for these claims, and it also means that the onus for “clean” claims is on the biller.
How much more can a provider bill than Medicare?
However, for alternative procedures, the provider can bill up to 15 percent more than the Medicare approved amount, and the bill is sent directly to the patient who will seek reimbursement from Medicare.
How long does it take for Medicare to process a claim?
They obtain claims from medical billing officials after a Medicare recipient has received care at a participating facility. This process generally takes around 30 days.
What is a Part B claim?
Part B. For Part B services that cover outpatient procedures and testing, reimbursement depends on whether or not the provider accepts Medicare assignment.
What is a CMS-1500?
Part B claims are filed using the CMS-1500 form. This is the standardized claim for that is used by healthcare providers that contract with Medicare. For providers that do not accept assignment for the specific procedure, Medicare will pay the patient directly for the reimbursement amount.
Is Medicare Part C billed directly?
Medicare Part C is also known as Medicare Advantage. These plans are offered through private insurers, so the billing is not filed directly though Medicare.
Can you opt out of Medicare?
Some providers may completely opt out of Medicare, meaning that they are not able to bill Medicare for any services. This means that the patient is responsible for paying for all costs out of pocket. In addition, there is no limit to the amount that the provider can charge for a procedure.
Is Medicare a federal or state insurance?
Medicare is a federally funded health insurance option, and since Medicare is responsible for reimbursing all participating healthcare facilities, the billing process is very particular.
How does Medicare work with other insurance?
When there's more than one payer, "coordination of benefits" rules decide which one pays first. The "primary payer" pays what it owes on your bills first, and then sends the rest to the "secondary payer" (supplemental payer) ...
How long does it take for Medicare to pay a claim?
If the insurance company doesn't pay the claim promptly (usually within 120 days), your doctor or other provider may bill Medicare. Medicare may make a conditional payment to pay the bill, and then later recover any payments the primary payer should have made. If Medicare makes a. conditional payment.
How many employees does a spouse have to have to be on Medicare?
Your spouse’s employer must have 20 or more employees, unless the employer has less than 20 employees, but is part of a multi-employer plan or multiple employer plan. If the group health plan didn’t pay all of your bill, the doctor or health care provider should send the bill to Medicare for secondary payment.
When does Medicare pay for COBRA?
When you’re eligible for or entitled to Medicare due to End-Stage Renal Disease (ESRD), during a coordination period of up to 30 months, COBRA pays first. Medicare pays second, to the extent COBRA coverage overlaps the first 30 months of Medicare eligibility or entitlement based on ESRD.
What is the phone number for Medicare?
It may include the rules about who pays first. You can also call the Benefits Coordination & Recovery Center (BCRC) at 1-855-798-2627 (TTY: 1-855-797-2627).
What happens when there is more than one payer?
When there's more than one payer, "coordination of benefits" rules decide which one pays first. The "primary payer" pays what it owes on your bills first, and then sends the rest to the "secondary payer" (supplemental payer) to pay. In some rare cases, there may also be a third payer.
What is a health care provider?
Tell your doctor and other. health care provider. A person or organization that's licensed to give health care. Doctors, nurses, and hospitals are examples of health care providers. about any changes in your insurance or coverage when you get care.
How to start the medical billing process for Medicaid?
You will start the medical billing process for Medicaid by filling out a state claim form for the services and procedures covered. Most state Medicaid claim forms will be divided into main two parts: information regarding the patient and/or the insured person and information regarding the healthcare provider.
What form do you need to bill Medicare?
If a biller has to use manual forms to bill Medicare, a few complications can arise. For instance, billing for Part A requires a UB-04 form (which is also known as a CMS-1450). Part B, on the other hand, requires a CMS-1500. For the most part, however, billers will enter the proper information into a software program and then use ...
What happens if a provider doesn't provide an ABN?
If the provider doesn’t offer the ABN or the patient doesn’t sign the notice before services are rendered, the patient doesn’t have to pay for that service. When billing for traditional Medicare (Parts A and B), billers will follow the same protocol as for private, third-party payers, and input patient information, NPI numbers, procedure codes, ...
What is an ABN in Medicare?
A provider who furnishes a service that Medicare probably won’t cover can ask the patient to sign an advanced beneficiary notice (ABN). By signing an ABN, the patient agrees to be financially responsible for the service if Medicare denies payment.
Is Medicaid more complicated than Medicare?
BILLING FOR MEDICAID. Medicaid programs differ from state to state medical billing for Medicaid is much more complicated than Medicare. Some citizens eligible for care in one state may not be eligible for care in another state, or they may receive more or fewer benefits depending on the state in which they receive care.
Can Medicare bill for Part D?
Only those providers who are licensed to bill for Part D may bill Medicare for vaccines or prescription drugs provided under Part D. If the provider is not a licensed Part D provider, the biller must assign that total directly to the patient (or the patient’s secondary insurance, if they have it, and if it covers that procedure or prescription).
Does Medicare have a claim processing system?
In addition, its claims processing system is highly refined. Any claim that is submitted with errors or without the correct information does not process.
How does Original Medicare work?
Original Medicare covers most, but not all of the costs for approved health care services and supplies. After you meet your deductible, you pay your share of costs for services and supplies as you get them.
How does Medicare Advantage work?
Medicare Advantage bundles your Part A, Part B, and usually Part D coverage into one plan. Plans may offer some extra benefits that Original Medicare doesn’t cover — like vision, hearing, and dental services.
When do hospitals report Medicare beneficiaries?
If the beneficiary is a dependent under his/her spouse's group health insurance and the spouse retired prior to the beneficiary's Medicare Part A entitlement date, hospitals report the beneficiary's Medicare entitlement date as his/her retirement date.
What is secondary payer?
Medicare is the Secondary Payer when Beneficiaries are: 1 Treated for a work-related injury or illness. Medicare may pay conditionally for services received for a work-related illness or injury in cases where payment from the state workers’ compensation (WC) insurance is not expected within 120 days. This conditional payment is subject to recovery by Medicare after a WC settlement has been reached. If WC denies a claim or a portion of a claim, the claim can be filed with Medicare for consideration of payment. 2 Treated for an illness or injury caused by an accident, and liability and/or no-fault insurance will cover the medical expenses as the primary payer. 3 Covered under their own employer’s or a spouse’s employer’s group health plan (GHP). 4 Disabled with coverage under a large group health plan (LGHP). 5 Afflicted with permanent kidney failure (End-Stage Renal Disease) and are within the 30-month coordination period. See ESRD link in the Related Links section below for more information. Note: For more information on when Medicare is the Secondary Payer, click the Medicare Secondary Payer link in the Related Links section below.
Does Medicare pay for black lung?
Federal Black Lung Benefits - Medicare does not pay for services covered under the Federal Black Lung Program. However, if a Medicare-eligible patient has an illness or injury not related to black lung, the patient may submit a claim to Medicare. For further information, contact the Federal Black Lung Program at 1-800-638-7072.
Does Medicare pay for the same services as the VA?
Veteran’s Administration (VA) Benefits - Medicare does not pay for the same services covered by VA benefits.
Is Medicare a primary or secondary payer?
Providers must determine if Medicare is the primary or secondary payer; therefore, the beneficiary must be queried about other possible coverage that may be primary to Medicare. Failure to maintain a system of identifying other payers is viewed as a violation of the provider agreement with Medicare.
How long does it take for Medicare to process a claim?
Medicare claims to providers take about 30 days to process. The provider usually gets direct payment from Medicare. What is the Medicare Reimbursement fee schedule? The fee schedule is a list of how Medicare is going to pay doctors. The list goes over Medicare’s fee maximums for doctors, ambulance, and more.
What happens if you see a doctor in your insurance network?
If you see a doctor in your plan’s network, your doctor will handle the claims process. Your doctor will only charge you for deductibles, copayments, or coinsurance. However, the situation is different if you see a doctor who is not in your plan’s network.
Does Medicare cover out of network doctors?
Coverage for out-of-network doctors depends on your Medicare Advantage plan. Many HMO plans do not cover non-emergency out-of-network care, while PPO plans might. If you obtain out of network care, you may have to pay for it up-front and then submit a claim to your insurance company.
Do participating doctors accept Medicare?
Most healthcare doctors are “participating providers” that accept Medicare assignment. They have agreed to accept Medicare’s rates as full payment for their services. If you see a participating doctor, they handle Medicare billing, and you don’t have to file any claim forms.
Do you have to pay for Medicare up front?
But in a few situations, you may have to pay for your care up-front and file a claim asking Medicare to reimburse you. The claims process is simple, but you will need an itemized receipt from your provider.
Do you have to ask for reimbursement from Medicare?
If you are in a Medicare Advantage plan, you will never have to ask for reimbursement from Medicare. Medicare pays Advantage companies to handle the claims. In some cases, you may need to ask the company to reimburse you. If you see a doctor in your plan’s network, your doctor will handle the claims process.
Can a doctor ask for a full bill?
In certain situations, your doctor may ask you to pay the full cost of your care–either up-front or in a bill; this might happen if your doctor doesn’t participate in Medicare. If your doctor doesn’t bill Medicare directly, you can file a claim asking Medicare to reimburse you for costs that you had to pay.
