What is the Medicare-approved amount?
The Medicare-approved amount is the total payment that Medicare has agreed to pay a health care provider for a service or item. Learn more your potential Medicare costs. The Medicare-approved amount is the amount of money that Medicare will pay a health care provider for a medical service or item.
How are Medicare premiums determined?
Medicare premiums are based off how much you earned two years ago. Your modified adjusted gross income will determine what you pay for Medicare coverage.
What is a Medicare-approved provider?
If a provider agrees to accept Medicare assignment (they are called a “Medicare participating provider”), they agree to accept the Medicare-approved amount as payment in full for any service they provide (assuming it is covered by Medicare).
How are Social Security and Medicare qualifications determined?
The formula for determining a person’s qualification for Social Security and Medicare is the same. It is based on income earned and taxes paid for the duration of working life. The annual W-2 Form that U.S. employees receive includes not only year-to-date earnings but also taxes paid toward Social Security and Medicare.

How does Medicare decide how much to pay?
Payment rates for these services are determined based on the relative, average costs of providing each to a Medicare patient, and then adjusted to account for other provider expenses, including malpractice insurance and office-based practice costs.
What does it mean Medicare-approved amount?
The approved amount, also known as the Medicare-approved amount, is the fee that Medicare sets as how much a provider or supplier should be paid for a particular service or item. Original Medicare also calls this assignment. See also: Take Assignment, Participating Provider, and Non-Participating Provider.
Do I have to pay more than the Medicare-approved amount?
If you use a nonparticipating provider, they can charge you the difference between their normal service charges and the Medicare-approved amount. This cost is called an “excess charge” and can only be up to an additional 15 percent of the Medicare-approved amount.
What is the difference between Medicare-approved amount and amount Medicare paid?
Medicare-Approved Amount: This is the amount a provider can be paid for a Medicare service. It may be less than the actual amount the provider charged. Your provider has agreed to accept this amount as full payment for covered services. Medicare usually pays 80% of the Medicare-approved amount.
What does approved amount mean?
Approved Amount means the maximum principal amount of Advances that is permitted to be outstanding under the Credit Line at any time, as specified in writing by the Bank.
What is the difference between the Medicare approved amount for a service or supply and the actual charge?
BILLED CHARGE The amount of money a physician or supplier charges for a specific medical service or supply. Since Medicare and insurance companies usually negotiate lower rates for members, the actual charge is often greater than the "approved amount" that you and Medicare actually pay.
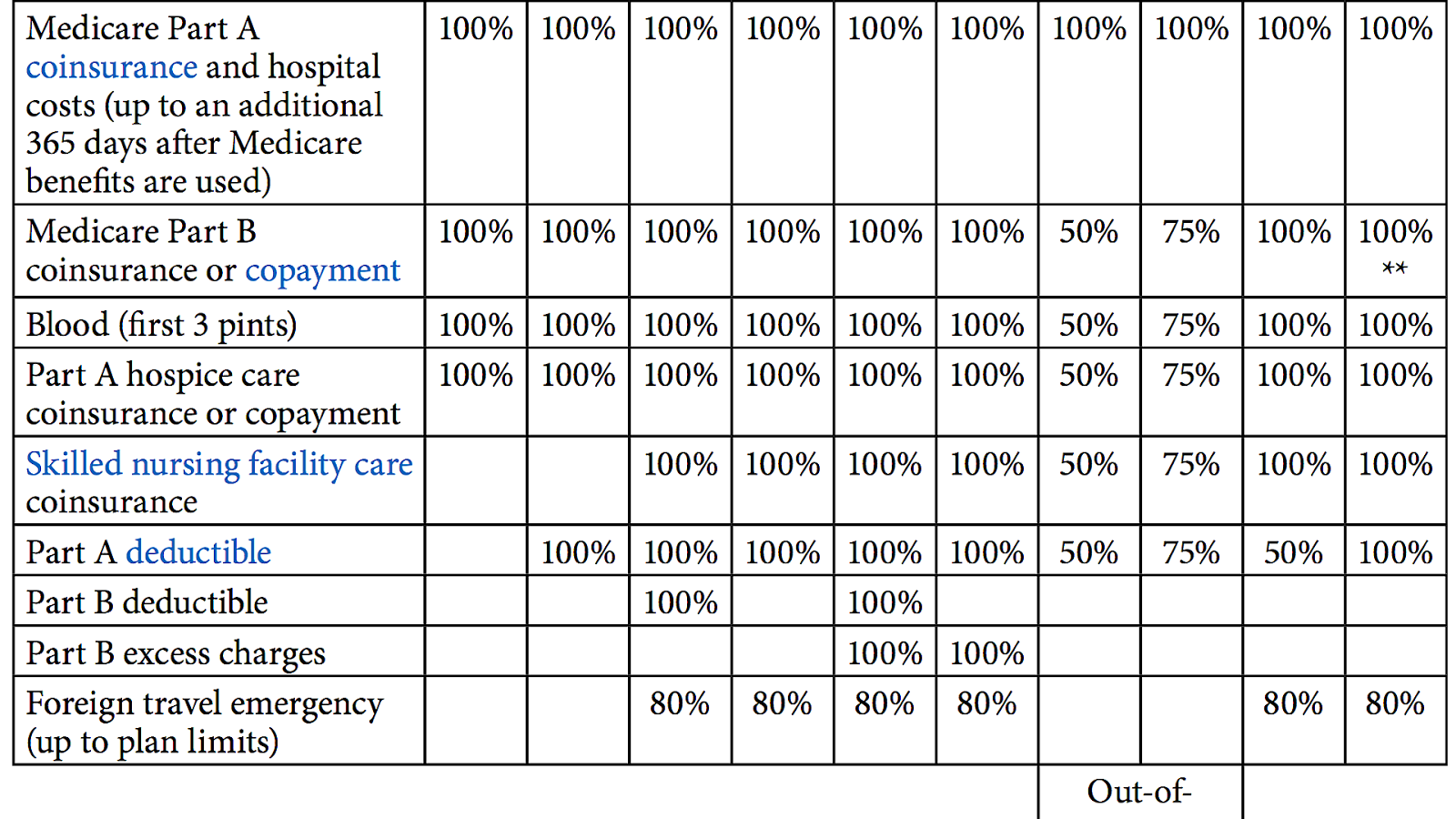
Does Medicare pay 100 percent of hospital bills?
According to the Centers for Medicare and Medicaid Services (CMS), more than 60 million people are covered by Medicare. Although Medicare covers most medically necessary inpatient and outpatient health expenses, Medicare reimbursement sometimes does not pay 100% of your medical costs.
Does Medicare only pay 80%?
Original Medicare only covers 80% of Part B services, which can include everything from preventive care to clinical research, ambulance services, durable medical equipment, surgical second opinions, mental health services and limited outpatient prescription drugs.
Do doctors have to accept what Medicare pays?
Can Doctors Refuse Medicare? The short answer is "yes." Thanks to the federal program's low reimbursement rates, stringent rules, and grueling paperwork process, many doctors are refusing to accept Medicare's payment for services. Medicare typically pays doctors only 80% of what private health insurance pays.
What percentage of the allowed amount is paid by Medicare for medical services?
In Original Medicare, the highest amount of money you can be charged for a covered service by doctors and other health care suppliers who don't accept assignment. The limiting charge is 15% over Medicare's approved amount. The limiting charge only applies to certain services and doesn't apply to supplies or equipment.
What is Medicare approved amount?
The Medicare-approved amount is the total payment that Medicare has agreed to pay a health care provider for a service or item. Learn more your potential Medicare costs. The Medicare-approved amount is the amount of money that Medicare will pay a health care provider for a medical service or item.
How much does Medicare pay for a doctor appointment?
Typically, you will pay 20 percent of the Medicare-approved amount, and Medicare will pay the remaining 80 percent .
What is Medicare Supplement Insurance?
Some Medicare Supplement Insurance plans (also called Medigap) provide coverage for the Medicare Part B excess charges that may result when a health care provider does not accept Medicare assignment.
What is Medicare Part B excess charge?
What are Medicare Part B excess charges? You are responsible for paying any remaining difference between the Medicare-approved amount and the amount that your provider charges. This difference in cost is called a Medicare Part B excess charge. By law, a provider who does not accept Medicare assignment can only charge you up to 15 percent over ...
What is 20 percent coinsurance?
Your 20 percent amount is called Medicare Part B coinsurance. Let’s say your doctor decides to refer you to a specialist to have your shoulder further examined. The specialist you visit agrees to treat Medicare patients but does not agree to accept the Medicare-approved amount as full payment. You still only pay 20 percent ...
How much can a provider charge for not accepting Medicare?
By law, a provider who does not accept Medicare assignment can only charge you up to 15 percent over the Medicare-approved amount. Let’s consider an example: You’ve been feeling some pain in your shoulder, so you make an appointment with your primary care doctor.
Does Medicare cover a primary care appointment?
This appointment will be covered by Medicare Part B, and you have already satisfied your annual Part B deductible. Your primary care doctor accepts Medicare assignment, which means they have agreed to accept Medicare as full payment for their services. Because you have met your deductible for the year, you will split the Medicare-approved amount ...
What does knowing the Medicare approved amount for a particular service or item help you determine?
Knowing the Medicare-approved amount for a particular service or item can help you determine your coinsurance amount and better budget your care.
What is Medicare approved amount?
The Medicare-approved amount, or “allowed amount,” is the amount that Medicare reimburses health care providers for the services they deliver. Learn more about the Medicare-approved amount and how it affects your Medicare costs. There’s a lot of terminology for Medicare beneficiaries to learn, and among them is “Medicare-approved amount” ...
How much does Medicare coinsurance increase?
The higher the Medicare-approved amount, the higher your coinsurance billed amount will likely be. If the Medicare-approved amount for the X-rays in the example above was $250 instead of $200, that would increase the total cost of the visit to $400, which would also increase the cost of your coinsurance payment to $80 (20% of $400).
How much is coinsurance for Medicare Part B?
Medicare Part B typically requires a coinsurance payment of 20% of the Medicare-approved amount for covered care after you meet your annual Part B deductible. Using the example above, your 20% coinsurance payment for your visit to the health clinic would likely be $70 (20% of $350).
What does Medicare cover?
The Medicare-approved amount applies mostly to services covered by Medicare Part B, which covers outpatient services like doctor’s appointments, and it also covers durable medical equipment (DME) such as wheelchairs and blood sugar test strips.
What is an excess charge for Medicare?
These providers reserve the right to charge up to 15% more than the Medicare-approved amount in what is known as an “excess charge.”
How much does Medicare pay for X-rays?
The X-rays may have a Medicare-approved amount of $200. And the brace itself might have a Medicare-approved amount of $50. (Note: these costs are hypothetical and are not based on actual Medicare costs for the services or items mentioned.) Based on the above costs, the health clinic would be allowed by Medicare to charge $350 total for ...
What is Medicare coverage?
Medicare coverage is limited to items and services that are reasonable and necessary for the diagnosis or treatment of an illness or injury (and within the scope of a Medicare benefit category).
How long is the comment period for CMS?
This comment period shall last 30 days, and comments will be reviewed and a final decision issued not later than 60 days after the conclusion of the comment period. A summary of the public comments received and responses to the comments will continue to be included in the final NCD. (§731 (a) (3) (A))
How long does it take to get a decision on an NCD?
For those NCD requests requiring either an external TA and/or MEDCAC review, and in which a clinical trial is not requested, the decision on the request shall be made not later than 9 months after the date the completed request is received; (§731 (a) (2) (B))
How long do you have to be on Medicare to receive Part A?
People under age 65 may receive Part A with no liability for premiums under the following circumstances: Have received Social Security or Railroad Retirement Board disability benefits for two years.
What is the Medicare premium for 2020?
For 2020, the standard monthly rate is $144.60. However, it will be more if you reported above a certain level of modified adjusted gross income on your federal tax return two years ago. Any additional amount charged to you is known as IRMAA, which stands for income-related monthly adjustment amount. Visit Medicare.gov, point to “Your Medicare Costs,” and then click “Part B costs” to see a matrix of premiums corresponding to income ranges across different tax filing statuses.
How many years of work do you need to be eligible for Medicare?
Four is the maximum number of credits a person can earn per year, so it takes at least 10 years or 40 quarters of employment to be eligible for Medicare.
Is Medicare the same for everyone?
Medicare is a federal program that mandates standardization of services nationwide, so many people may assume the premiums would be the same for everyone. In reality, there are variations in the premiums people pay, if they pay any at all.
Can Medicare be charged at 65?
For Part A, most Medicare recipients are not charged any premium at all. Seniors at age 65 are eligible for premium-free Part A if they meet the following criteria: Currently collect retirement benefits from Social Security or the Railroad Retirement Board. Qualify for Social Security or Railroad benefits not yet claimed.
How much does Medicare pay for medical services?
The Medicare reimbursement rates for traditional medical procedures and services are mostly established at 80 percent of the cost for services provided. Some medical providers are reimbursed at different rates. Clinical nurse specialists are paid 85 percent for most of their billed services and clinical social workers are paid 75 percent ...
How much can Medicare increase from current budget?
By Federal statute, the Medicare annual budget request cannot increase more than $20 million from the current budget.
What is Medicare reimbursement rate?
The reimbursement rates are the monetary amounts that Medicare pays to health care providers, hospitals, laboratories, and medical equipment companies for performing certain services and providing medical supplies for individuals enrolled in Medicare insurance. To receive reimbursement payments at the current rates established by Medicare, health care professionals and service companies need to be participants in the Medicare program. While non-participating professionals and companies are able to submit claims and receive reimbursements for their services, their reimbursements will be slightly lower than the rates paid to participants.
What is the Medicare coinsurance?
Today, Medicare enrollees who use the services of participating health care professionals will be responsible for the portion of a billing claim not paid by Medicare. The majority of enrollee responsibility will be 20 percent, often referred to as coinsurance. With clinical nurse specialists that responsibility would be 15 percent and 25 percent for clinical social workers.
How many specialists are on the Medicare committee?
Medicare establishes the reimbursement rates based on recommendations from a select committee of 52 specialists. The committee is composed of 29 medical professionals and 23 others nominated by professional societies.
Why use established rates for health care reimbursements?
Using established rates for health care reimbursements enables the Medicare insurance program to plan and project for their annual budget. The intent is to inform health care providers what payments they will receive for their Medicare patients.
What percentage of Medicare bill is not paid?
The majority of enrollee responsibility will be 20 percent , often referred to as coinsurance.
What is Medicare Advantage?
Essentially: Medicare Advantage – Private plans that replace your Parts A, B, and in most cases, D. Also known as Part C. Medicare Part D – Prescription drug coverage plans, introduced in 2006. Generally, if you’re on Medicare, you aren’t charged a premium for Part A.
How Much Are Medicare Premiums in 2021?
There are six income tiers for Medicare premiums in 2021. As stated earlier, the standard Part B premium amount that most people are expected to pay is $148.50 month. But, if your MAGI exceeds an income bracket — even by just $1 — you are moved to the next tier and will have to pay the higher premium.
Why did Medicare Part B premiums increase in 2021?
That’s because 2021 Medicare Part B premiums increased across the board due to rising healthcare costs. Exactly how much your premiums increased though, isn’t based on your current health or Medicare plan or your income. Rather, it’s the soaring prices of overall healthcare.
How much of Medicare Part B is paid?
But the remaining 25% of Medicare Part B expenses are paid through your premium, which is determined by your income level. Medicare prices are quoted under the assumption you have an average income. If your income level exceeds a certain threshold, you will have to pay more.
Why are Social Security beneficiaries paying less than the full amount?
In 2016, 2017, and 2018, the Social Security COLA amount for most beneficiaries wasn’t enough to cover the full cost of the Part B premium increases, so most enrollees were paying less than the full amount, because they were protected by the hold harmless rule.
How much is Part B 2021?
So most beneficiaries are paying the standard $148.50/month for Part B in 2021. The hold harmless provision does NOT protect you if you are new to Medicare and/or Social Security, not receiving Social Security benefits, or are in a high-income bracket.
What are some changes you may make by choice?
The beginning of the year always brings about change. Some are changes you may make by choice, like deciding to quit smoking or being more active. And others are changes that have been determined for you, like changes to your Medicare monthly premiums.
How is Medicare compensation calculated?
Basically, the relative value of a procedure multiplied by the number of dollars per Relative Value Unit (RVU) is the fee paid by Medicare for the procedure (RVUW physician work, RVUPE practice expense, RVUMP malpractice). The Conversion Factor (CF) is the number of dollars assigned to an RVU. It is calculated by use of a complex formula (Fig 1) that takes into account the overall state of the economy of the United States, the number of Medicare beneficiaries, the amount of money spent in prior years, and changes in the regulations governing covered services. Medicare fees are set according to a relative value scale rather than a free market, payments are made by third parties rather than consumers, and the labor market for physicians is illiquid, so the pricing mechanisms that regulate markets in other parts of the economy are not effective in rationalizing prices. The factors that influence the CF calculation are similar to those that are used in calculating global health care budgets; therefore the principles are durable, even if the precise formula might be altered in the future
What is Medicare negotiated rate?
Maximum amount on which payment is based for covered health care services. This may be called “eligible expense,” “payment allowance” or “negotiated rate.” If your provider charges more than the medicare allowed amount, patient no need to pay that amount when they are participating with Medicare insurance.
How often is the RVU code reviewed?
GPCIsare reviewed every 3 years.
How much does a CPT code 99408 cost?
If a provider assesses, counsels or provides behavioral intervention to a Workers’ Compensation patient for substance and/or alcohol use, or for substance and/or Alcohol use disorder, the provider may charge for the extra time involved using CPT® code 99408 (or CPT® codes 96150-96155, if appropriate) up to a maximum of eighty dollars ($80) in addition to a standard E/M code. An assessment by structured screening must be documented. The code may only be charged if the patient is on a long term (over 90 days) Schedule II medication or a combination of one or more Schedule II, Ill, and/or IV medications. The Medicare allowable fee does not apply to this service. See Rule 0800-02-17-.15.
What is CF in Medicare?
The CF, a national dollar multiplier, is used to “convert” the geographically adjusted RVU to determine the Medicare-allowed payment amount for a particular physician service. The CF is used separately to price facility and nonfacility payment amounts. Facility pricing typically covers services provided to inpatients or in a hospital outpatient clinic setting or other off-site hospital facilities. Nonfacility pricing covers services gen erally provided in a physician office or other freestanding setting such as an Independent Diagnostic Testing Facility.
Does the Allowed amount cover all charges?
Allowed amount may not cover all the provider’s charges. In some cases, subscribers may have to pay the difference.
Is Wisconsin Physicians Service Insurance Corporation a Medicare agency?
This is an advertisement for insurance. Neither Wisconsin Physicians Service Insurance Corporation nor its agents are connected with the federal Medicare program. Our products are not connected with or endorsed by the United States government or the federal Medicare program.