How many days will Medicare pay 100% of the covered costs of care in a skilled nursing care facility?
100 daysMedicare covers care in a SNF up to 100 days in a benefit period if you continue to meet Medicare's requirements.
What pays for most long term care?
Long-term care services are financed primarily by public dollars, with the largest share financed through Medicaid, the federal/state health program for low- income individuals.
What will Medicare not pay for?
Generally, Original Medicare does not cover dental work and routine vision or hearing care. Original Medicare won't pay for routine dental care, visits, cleanings, fillings dentures or most tooth extractions. The same holds true for routine vision checks. Eyeglasses and contact lenses aren't generally covered.
What is the approximate average length of stay for a resident in a nursing home in the US?
Across the board, the average stay in a nursing home is 835 days, according to the National Care Planning Council. (For residents who have been discharged- which includes those who received short-term rehab care- the average stay in a nursing home is 270 days, or 8.9 months.)
Does Medicare Pay For Long Term Home Care?
Medicare benefits for home care are limited. If you are home bound, Medicare will pay for some home health services ordered by your doctor, such as...
Does Medicare Pay For Long Term Assisted Living?
No. Assisted living facilities provide help with day to day activities, and this is not covered by Medicare.
Does Medicare Pay For Long Term Nursing Care?
Medicare pays for skilled care in a long-term facility for up to 100 days after you have been discharged from a hospital stay lasting at least thre...
Does Medicare Pay For Long Term Memory Care?
Like long term nursing home care, long term memory care is custodial care not covered by Medicare. You can find more information on long term memor...
Does Medicare Pay For Long Term Acute Care?
Medicare pays for acute care in a long-term care hospital, using the same rules that apply to any other hospital stay. Long term care hospitals foc...
How long does it take to get Medicare long term care?
Medicare long term care eligibility is attainable under the following conditions when hospitalized: You must be an inpatient at an approved hospital for at least three days. After being admitted to a Medicare-certified nursing facility within 30 days of your inpatient hospital visit. You must require additional therapy such as physical ...
How long does Medicare pay for physical therapy?
Medicare long term eligibility starts after meeting these requirements and pays for a maximum of 100 days during each benefit period.
How long does it take to qualify for Medicare?
Medicare long term care eligibility is attainable under the following conditions when hospitalized: 1 You must be an inpatient at an approved hospital for at least three days 2 After being admitted to a Medicare-certified nursing facility within 30 days of your inpatient hospital visit 3 You must require additional therapy such as physical or occupational 4 Your condition medically demands skilled nursing services
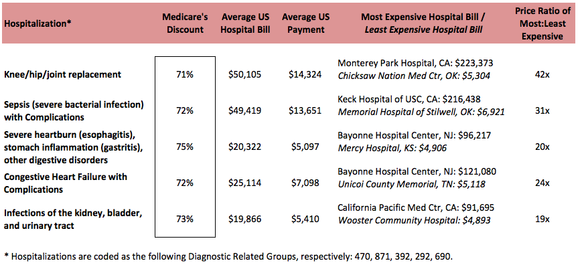
How much does a nursing home cost?
A private nursing home room costs over $250 per day or $8,000 a month. You can imagine how financially exhausting this may become – and fast if you’re unprepared. However, proper long-term care insurance must meet your healthcare needs.
What are the benefits of Medicare Advantage?
Advantage plans are extending coverage even further; benefits may include personal care, meal delivery, transportation, and adult day care services. One rule of thumb Medicare and long-term care remains consistent, even with the new benefit options. Medicare nor Medicare Advantage plans include the cost of room and board or assistance ...
What states have long term care partnerships?
Four original states pioneered the Long Term Care Partnership Program; terms are different in California, Connecticut, New York, and Indiana. The program is protection for your lifestyle, income, and assets. Although conventional long-term care insurance is the only type to qualify for Partnership asset protection, without long-term care insurance, ...
Does Medicare pay for hospice?
After meeting requirements, Medicare may pay for a short-term stay in a skilled nursing facility. Part A always pays for hospice care if you’re not looking for further treatment and have a terminal illness. Custodial care may not be part of your coverage.
What percentage of people turn 65 need long term care?
52% of people turning 65 will need some form of long-term care in their lifetimes. Does your Medicare plan include long-term care? Compare Medicare plans in your area. Some Medicare Advantage plans may cover certain long-term care and at-home care services, such as home-delivered meals, grab bars for home bathrooms and other additional benefits.
What is Medicare Part A?
Medicare Part A provides hospital insurance and covers care received in a long-term care hospital (LTCH). You may qualify for this type of care if you meet the following two requirements:
How much is the Medicare deductible for 2020?
The 2020 Medicare Part A deductible is $1,408 per benefit period.
What is SNF in Medicare?
Your SNF is certified by Medicare. You need this care for a hospital-related health condition or a condition that started while you were in an SNF for a hospital-related condition. You will also need to meet your Part A deductible for each benefit period before Medicare Part A begins paying for your SNF care.
How much is Part A coinsurance?
After you meet the Part A deductible, you are responsible for Part A coinsurance payments of $352 per day (in 2020) for days 61-90 of your inpatient stay in each benefit period, and $704 per day for days 91 and beyond in each benefit period until you exhaust your 60 lifetime reserve days.
Does Medicare cover home health care?
A doctor certifies that you are homebound. You typically have no Medicare costs for home health care services , and you typically pay 20 percent of the Medicare-approved amount for qualified durable medical equipment (DME) you may require while receiving home health care.
Does Medicare cover nursing home care?
Many Medicare Advantage plans also cover prescription drugs , and some plans may also provide coverage for: Although Original Medicare does not cover long-term custodial care (including nursing home care), Medicare Part A and Part B may help cover other specialized types of care for limited periods of time:
What is Medicaid for low income?
Medicaid pays for health care services for those individuals with low income and assets who may incur very high medical bills.
How long does a person live with hospice?
You have elected to no longer seek a cure. Your life expectancy is six months or less. Hospice care may be received in your home, in a nursing home, or a hospice care facility. Short-term hospital stays and inpatient care may also be approved for Medicare payment (for caregiver respite).
What is a Medicaid certified nursing home?
Medicaid certified nursing homes deliver specific medically indicated care , known as Nursing Facility Services , including: Medicaid coverage for Nursing Facility Services only applies to services provided in a nursing home licensed and certified as a Medicaid Nursing Facility (NF).
How long can you stay in an SNF?
If your stay in an SNF exceeds 100 days, or your ability to pay co-pays ends before the 100th day is reached, you may no longer be eligible to stay in the Medicare-certified SNF under Medicare coverage.
What does the VA pay for?
The VA may also pay for long-term care services required by veterans who do not have service-related disabilities but are incapable of paying for essential care. In these cases, services may require a sliding scale co-pay based on patient income level.
Can you recover Medicaid for nursing home?
If you received Medicaid coverage for long-term care services, the state can choose to recoup Medicaid costs. Federal law provides states with the ability to recover any or all costs incurred by Medicaid for long-term care services, including nursing home, home, or community-based services.
Does Medicare pay for physical therapy?
Provided you meet the above conditions, Medicare will pay a portion of the costs during each benefit period for a limited number of days.
What is long term care?
Long-term care, often called custodial care, is a range of services and support to meet health or personal care needs over an extended period of time. This is non-medical care provided by non-licensed caregivers.
How many years of nursing home care is needed at 65?
20% of those turning 65 will need care for longer than five years. About 35% of people who reach age 65 are expected to enter a nursing home at least once in their lifetime.
What is considered qualified medical expenses?
According to the IRS, qualified medical expenses “also include amounts paid for qualified long-term care services and limited amounts paid for any qualified long-term care insurance contract.”. Qualified long-term care services include maintenance and personal care services that a chronically ill individual requires.
What is a combination life insurance?
Combination or hybrid products–life insurance with a long-term care rider. Consumers tend to worry that they will lose the money they spend on long-term care insurance if they don’t use it. In recent years, insurance companies have taken steps to ease these concerns.
Why don't people qualify for medicaid?
Those who don’t qualify for Medicaid because their assets are too high have to pay for long-term care. Then, once their assets are low enough, they can qualify for Medicaid coverage. Every state has its own enrollment process, qualification criteria and policies.
How many people are expected to enter nursing homes at 65?
About 35% of people who reach age 65 are expected to enter a nursing home at least once in their lifetime. The need for long-term care comes into play when the aging process begins to take effect and one loses the ability to perform activities of daily living (ADL).
Why is a person in a nursing home?
The person is in a nursing home because she is not safe at home and needs help with ADL. It doesn’t take a nurse to bathe a person in her home. Contrast that to skilled care. The person who had a stroke goes to a nursing home for rehabilitation.
What is the difference between private pay and Medicaid?
Understanding the Difference Between Private Pay and Medicaid Reimbursement. Private pay is the amount that individuals who receive no public assistance pay for a nursing home. The “Medicaid reimbursement rate” is the amount a state Medicaid program pays the same nursing home for the same room.
How much does a nursing home cost in 2021?
At the time of writing (Jan. 2021) , the nationwide average daily cost for a shared room is $255.
How long does it take to get a free medicaid test?
Our website provides a free Medicaid eligibility test here. The test takes approximately 3 minutes to complete and is non-binding. Medicare and Medicaid. Medicare pays for nursing home care for its beneficiaries but only pays the full amount for 20 days. For the 80 days following, Medicare will pay for 80% of the cost.
Does Medicaid pay for nursing home care?
Medicaid will pay 100% of the cost of nursing home care for its beneficiaries. However, to be eligible for Medicaid nursing home care, the patient must have very limited income and very few financial assets (ballpark limits are assets valued under $2,000 and monthly income under $2,382). Medicaid eligibility criteria is state-specific.
Does Medicaid pay for shared rooms?
Unless there is a medical need for a private room in a nursing home, Medicaid will pay for a shared room only. Some states allow “family supplementation” which allows family members to supplement the payment in order to upgrade their loved one to a private room.