If you use oxygen tanks or cylinders that need delivery of gaseous or liquid oxygen contents, Medicare will continue to pay each month for the delivery of contents after the 36-month rental period, which means that you will pay 20% of the Medicare-approved amount for these deliveries.
Full Answer
Does Medicare cover continuous positive airway pressure?
Medicare pays the supplier to rent a CPAP machine for 13 months if you’ve been using it without interruption. After Medicare makes rental payments for 13 continuous months, you’ll own the machine. Medicare will only cover your durable medical equipment (DME) if your doctors and suppliers are enrolled in Medicare.
Does Medicare cover air-fluidized beds?
Medicare Part B (Medical Insurance) Part B covers certain doctors' services, outpatient care, medical supplies, and preventive services. covers air-fluidized beds and other support surfaces as durable medical equipment (DME) that your doctor prescribes for use in your home.
Does Medicare pay for oxygen and humidifiers?
You pay 20% of the. Medicare-Approved Amount. If you have Medicare and use oxygen, you’ll rent oxygen equipment from a supplier for 36 months. After 36 months, your supplier must continue to provide oxygen equipment and related supplies for an additional 24 months.
How long does Medicare pay for oxygen rental?
May 28, 2019 · If you have Medicare and you’re diagnosed with obstructive sleep apnea, you may be eligible to receive Continuous Positive Airway Pressure (CPAP) therapy for a three-month trial period. With Medicare Part B, you’ll pay 20% of the Medicare-approved amount for the CPAP machine rental and supplies, after reaching the Medicare Part B deductible. You must get the …

How often can you get a new CPAP machine under Medicare?
every five yearsMedicare will usually cover the cost of a new CPAP machine every five years. If you had a machine before enrolling in Medicare, Medicare may cover some of the costs for a replacement CPAP machine rental and accessories if you meet certain requirements.
How Long Will Medicare pay for CPAP supplies?
for 13 monthsMedicare pays the supplier to rent a CPAP machine for 13 months if you've been using it without interruption. After Medicare makes rental payments for 13 continuous months, you'll own the machine.
What is a qualifying diagnosis for oxygen?
Qualification for receiving oxygen at rest If your patient has an arterial oxygen saturation SaO2(2 is subscript)≤88% or partial pressure of oxygen Po2(2 is subscript)≤55 mm Hg at rest, no further testing is required.
Does AARP cover portable oxygen?
Oxygen Concentrator Store is proud to offer AARP members a $50 discount* off new portable oxygen concentrators, as well as other oxygen therapy products. This special AARP member discount* is available at our retail location or our online store.
Does Medicare pay for BiPAP machines?
Medicare will also cover different types of PAP machines, such as BiPAP or APAP, and even alternative treatment options like oral appliances and mouthguards. However, this coverage does require that you meet certain requirements and follow certain guidelines. What Does Part A or Part B Mean?Aug 13, 2021
How much does a CPAP machine cost with Medicare?
Cost of a CPAP Machine with MedicareAverage cost of a CPAP machineMedicare coverageTotal cost to you$85080%$373Sep 15, 2021
Are oximeters covered by Medicare?
Medicare does not cover pulse oximeters. Some private insurance plans do cover pulse oximetry services.May 26, 2020
What is a home oxygen evaluation?
A home oxygen assessment includes monitoring oxygen levels on room air, a possible arterial blood gas (if oxygen levels low), as well as the possibility of a walking oxygen level test. Preparation: Please notify the respiratory therapist if you are on and anti-coagulation medication (blood thinners).
Does Medicare pay for pulse oximeter 2020?
Medicare will allow payment for oximetry when accompanied by an appropriate ICD-9-CM code for a pulmonary disease(s) which is commonly associated with oxygen desaturation. Routine use of oximetry is non-covered.
Does Medicare pay for pulse oximeter 2021?
Does Medicare Cover Oxygen Therapy? Yes, oxygen therapy, as well as oxygen therapy tank accessories, are covered under Part B. Oxygen equipment and all accessories are Durable Medical Equipment. Part B covers the rental and use of DME for beneficiaries to use within their homes.
Does Medicare cover oxygen for pneumonia?
A chronic lung condition or another disease must be among Medicare's select group of diagnoses. Many beneficiaries with non-chronic lung diseases, such as pneumonia, do seek assistance breathing with oxygen but these beneficiaries are not covered.
Will Medicare pay for a cane and a walker at the same time?
Usually, Medicare Part B covers 80% of allowable charges for walking canes and walkers; you pay 20% plus any remaining Part B deductible. A Medicare Supplement Insurance plan may be able to cover your 20% coinsurance for your walking cane, and other out-of-pocket costs not covered by Medicare Part A and Part B.Jul 25, 2021
What percentage of Medicare payment does a supplier pay for assignment?
If your supplier accepts Assignment you pay 20% of the Medicare-approved amount, and the Part B Deductible applies. Medicare pays for different kinds of DME in different ways. Depending on the type of equipment:
What is Medicare approved amount?
Medicare-Approved Amount. In Original Medicare, this is the amount a doctor or supplier that accepts assignment can be paid. It may be less than the actual amount a doctor or supplier charges. Medicare pays part of this amount and you’re responsible for the difference. , and the Part B.
Does Medicare cover DME equipment?
You may be able to choose whether to rent or buy the equipment. Medicare will only cover your DME if your doctors and DME suppliers are enrolled in Medicare. Doctors and suppliers have to meet strict standards to enroll and stay enrolled in Medicare.
Do DME providers have to be enrolled in Medicare?
Make sure your doctors and DME suppliers are enrolled in Medicare. It’s important to ask your suppliers if they participate in Medicare before you get DME. If suppliers are participating suppliers, they must accept assignment (which means, they can charge you only the coinsurance and Part B deductible for the Medicare‑approved amount). ...
How long does Medicare provide oxygen?
If you have Medicare and use oxygen, you’ll rent oxygen equipment from a supplier for 36 months. After 36 months, your supplier must continue to provide oxygen equipment and related supplies for an additional 24 months. Your supplier must provide equipment and supplies for up to a total of 5 years, as long as you have a medical need for oxygen.
How much does Medicare pay for oxygen tanks?
If you use oxygen tanks or cylinders that need delivery of gaseous or liquid oxygen contents, Medicare will continue to pay each month for the delivery of contents after the 36-month rental period, which means that you will pay 20% of the Medicare-approved amount for these deliveries.
What is Part B for medical equipment?
Oxygen equipment & accessories. Part B covers certain doctors' services, outpatient care, medical supplies, and preventive services. covers the rental of oxygen equipment and accessories as durable medical equipment (DME) that your doctor prescribes for use in your home. Medicare will help pay for oxygen equipment, ...
What is Medicare approved amount?
Medicare-Approved Amount. In Original Medicare, this is the amount a doctor or supplier that accepts assignment can be paid. It may be less than the actual amount a doctor or supplier charges. Medicare pays part of this amount and you’re responsible for the difference. , and the Part B deductible applies.
How long does a supplier own equipment?
The supplier owns the equipment during the entire 5-year period . If your medical need continues past the 5-year period, your supplier no longer has to continue providing your oxygen and oxygen equipment, and you may choose to get replacement equipment from any supplier.
Does Medicare pay for oxygen?
Medicare will help pay for oxygen equipment, contents and supplies for the delivery of oxygen when all of these conditions are met: Your doctor says you have a severe lung disease or you’re not getting enough oxygen. Your health might improve with oxygen therapy.
Does Medicare cover oxygen equipment?
If you meet the conditions above, Medicare oxygen equipment coverage includes: Systems that provide oxygen. Containers that store oxygen. Tubing and related oxygen accessories for the delivery of oxygen and oxygen contents. Medicare may also pay for a humidifier when it's used with your oxygen machine.
How long does Medicare pay for a CPAP machine?
Medicare pays the supplier to rent the CPAP machine for up to 13 months, and after that, the CPAP machine is considered yours.
What is the Medicare Part B deductible?
As mentioned, with Medicare Part B, you will be responsible for paying 20% of the Medicare-approved amount to rent a CPAP device and necessary parts or accessories, and the Part B deductible applies.
How long is a CPAP trial?
If you have Medicare and you’re diagnosed with obstructive sleep apnea, you may be eligible to receive Continuous Positive Airway Pressure (CPAP) therapy for a three-month trial period. With Medicare Part B, you’ll pay 20% of the Medicare-approved amount for the CPAP machine rental and supplies, after reaching ...
Is a CPAP machine covered by Medicare?
If you already owned a CPAP machine before getting Medicare, some costs related to it may be covered by Medicare if you meet specific qualifications.
Does Medicare cover CPAP?
You must get the CPAP equipment from a Medicare-assigned supplier for Medicare to cover it. If your health-care provider decides that the sleep apnea therapy is helping, you may continue to be covered under Medicare for a longer period.
Can you stop breathing while sleeping?
Sleep apnea might be your diagnosis if you momentarily stop breathing while you sleep — sometimes many times per night, according to the U.S. Food and Drug Administration. Find affordable Medicare plans in your area. Find Plans. Find Medicare plans in your area. Find Plans.
Does Medicare require CPAP machines?
may be affected by the Medicare Competitive Bidding Program, which requires beneficiaries with Original Medicare to get durable medical equipment, such as the CPAP machine, from Medicare contracted suppliers in order to be covered by the Medicare program.
What is hyperbaric oxygen therapy?
Hyperbaric oxygen (HBO) therapy is used to help patients recover from a range of medical conditions. The treatments take place in a multi-person chamber or individual unit. During the treatment, air pressure is increased to three times higher than normal, allowing your lungs to gather more oxygen.
Does Medicare Advantage include oxygen therapy?
Medicare Advantage plans include the same benefits as Original Medicare Part A and Part B, but many offer additional benefits. If you are enrolled in a MA plan, check with your plan for exact costs for hyperbaric oxygen therapy. Related articles: What is Medicare Parts A & B.
How long does it take to use CPAP for Medicare?
How does Medicare define CPAP compliance or adherence? Medicare defines adherence as using the device more than 4 hours per night for 70% of nights (that’s 21 nights) during a consecutive 30 day period any time in the first three months of initial usage.
How much does Medicare pay for a PAP?
Medicare will pay 80% of the Medicare-approved amount for a PAP device after you’ve met your Part B deductible (learn about this and other insurance terms here ). If you have a secondary insurance, they may pick up the remaining 20% (read our post about how much sleep studies cost here ).
How long does a bi level CPAP trial last?
If the patient switches to a bi-level device within the 3-month trial, the length of the trial is not changed as long as there are at least 30 days remaining. If less than 30 days remain of the trial period, re-evaluation must occur before the 120th day (following the same criteria as CPAP adherence).
How many events per hour is AHI?
AHI or RDI > 15 events per hour with a minimum of 30 events or. AHI or RDI > 5 to14 events per hour with a minimum of 10 events recorded and documentation of: Excessive daytime sleepiness, impaired cognition, mood disorders or insomnia; or. Hypertension, ischemic heart disease or history of stroke.
When does Medicare continue to cover PAP?
If you are successful with the 3-month trial of PAP, Medicare may continue coverage if the following criteria are met: Clinical re-evaluation between the 31st and 91st day after starting therapy, to include: Treating physician documents that the patient is benefiting from therapy; and.
Does Medicare cover bi level respiratory assist?
Medicare will cover a bi-level respiratory assist device without backup (this is what they call a bi-level or BiPAP) for patients with obstructive sleep apnea if the patient meets the criteria for PAP therapy (outlined above) and:
Does Medicare require proof of usage?
Many other insurance companies are now following Medicare’s lead and requiring proof of usage before continuing to pay for the machine. Learn more about that here. If adherence to therapy is not documented within the first three months, the patient fails the trial period.
Does Medicare require a prescription for a nebulizer?
The prescription must include any supplies you need for using the machine. Orders must also state the condition requiring ne bulizer use and list the medications for use in conjunction with the nebulizer.
Can a nebulizer help with asthma?
People with asthma or chronic obstructive pulmonary disease may find relief from a nebulizer. Many doctors favor this method for treating asthma and other respiratory ailments. Nebulizers convert liquid medication into an inhalable mist. But, they often provide quick relief from breathing difficulties.
What is original Medicare?
Your costs in Original Medicare. In Original Medicare, this is the amount a doctor or supplier that accepts assignment can be paid. It may be less than the actual amount a doctor or supplier charges. Medicare pays part of this amount and you’re responsible for the difference.
What does a foot doctor cover?
covers podiatrist (foot doctor), foot exams or treatment if you have diabetes-related nerve damage or need. medically necessary. Health care services or supplies needed to diagnose or treat an illness, injury, condition, disease, or its symptoms and that meet accepted standards of medicine.
What is medically necessary?
medically necessary. Health care services or supplies needed to diagnose or treat an illness, injury, condition, disease, or its symptoms and that meet accepted standards of medicine. treatment your doctor provides, and the Part B. deductible.
How much is Medicare Part A 2020?
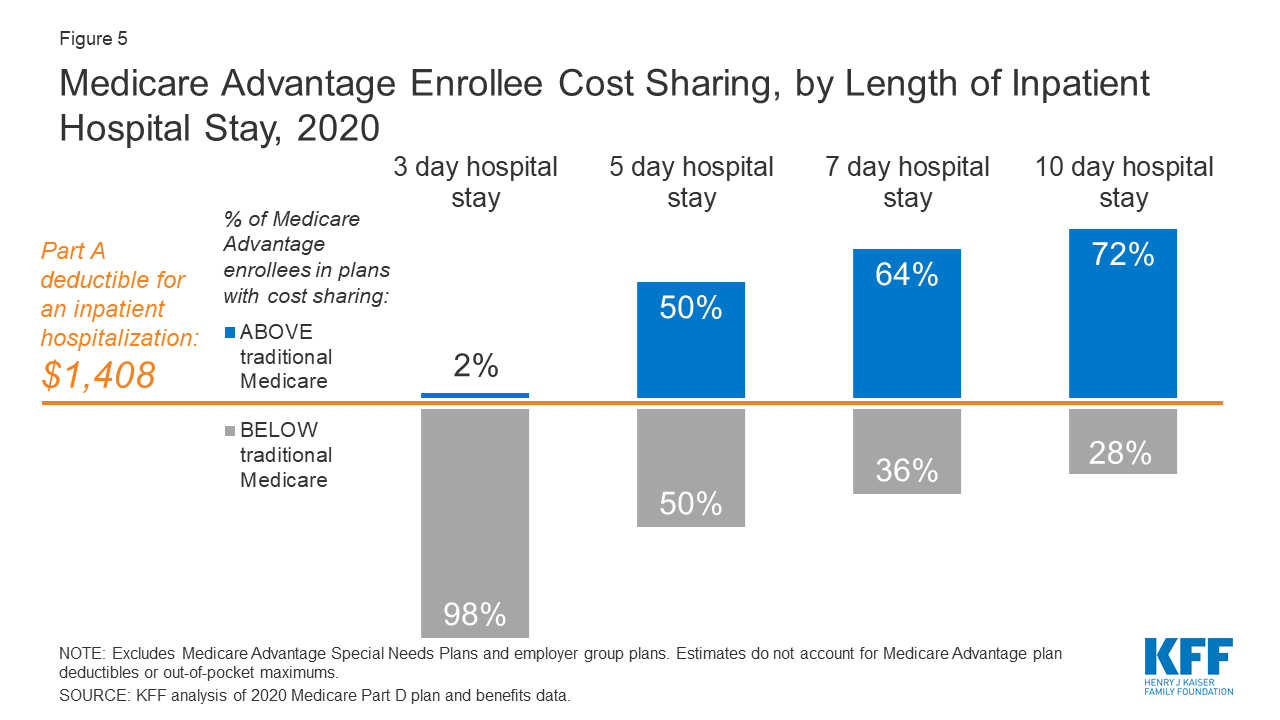
Beneficiaries who are admitted to a hospital for treatment of COVID-19 would be subject to the Medicare Part A deductible of $1,408 per benefit period in 2020 ($1,484 in 2021). Part A also requires daily copayments for extended inpatient hospital and SNF stays. For extended hospital stays, beneficiaries would pay a $352 copayment per day ...
How many people are covered by Medicare in 2020?
Published: Dec 04, 2020. More than 60 million people ages 65 and older and younger adults with long-term disabilities are covered by Medicare. Due to their older age and higher likelihood of having serious medical conditions than younger adults, virtually all Medicare beneficiaries are at greater risk of becoming seriously ill if they are infected ...
What is the Cares Act?
A separate provision in the CARES Act allows federally qualified health centers and rural health clinics to provide telehealth services to Medicare beneficiaries during the COVID-19 emergency period.
What is the deductible for telehealth?
Medicare covers all types of telehealth services under Part B, so beneficiaries in traditional Medicare who use these benefits are subject to the Part B deductible of $198 in 2020 and 20 percent coinsurance.
Does Medicare cover inpatient hospital stays?
Medicare covers inpatient hospital stays, skilled nursing facility (SNF) stays, some home health visits, and hospice care under Part A. If an inpatient hospitalization is required for treatment of COVID-19, this treatment will be covered for Medicare beneficiaries, including beneficiaries in traditional Medicare and those in Medicare Advantage ...
Does Medicare cover long term care?
Beneficiaries who need post-acute care following a hospitalization have coverage of SNF stays, but Medicare does not cover long-term services and supports, such as extended stays in a nursing home. Medicare covers outpatient services, including physician visits, physician-administered and infusion drugs, emergency ambulance transportation, ...
Is there a requirement for a 3 day prior hospitalization for a skilled nursing facility?
In response to the national emergency declaration related to the coronavirus pandemic, CMS is waiving the requirement for a 3-day prior hospitalization for coverage of a skilled nursing facility (SNF) for those Medicare beneficiaries who need to be transferred as a result of the effect of a disaster or emergency.
