What makes a good Medicaid managed care plan?
Oct 06, 2021 · Medicare managed care plans are an alternative to Original Medicare. Otherwise known as Medicare Advantage plans with many plan types, most are either HMOs or PPOs. Managed-care plans provide benefits for gaps in Parts A and B coverage. These alternative health-care plans make up Part C of Medicare.
What are 3 different types of managed care plans?
Nov 17, 2021 · A Medicare managed care plan is one type of Medicare Advantage plan. The term “managed care plan” generally refers to HMO (health maintenance organization), PPO (preferred provider organization) or POS (point of service) plans. These Medicare Advantage plans offer managed care that is coordinated between health care providers within a network.
What is the purpose of a managed care plan?
Sep 09, 2020 · Medicare care managed care plans are an optional coverage choice for people with Medicare. Managed care plans take the place of your original Medicare coverage. Original Medicare is made up of Part A (hospital insurance) and Part B (medical insurance). Plans are offered by private companies overseen by Medicare.
What is the best health plan for Medicare?
Mar 09, 2022 · The update to the CY 2021 guidance is now available below with the file names: CY2021 MA Enrollment and Disenrollment Guidance and CY2021 Cost Plan Enrollment and Disenrollment Guidance. All enrollments with an effective date on or after January 1, 2021, must be processed in accordance with the revised guidance requirements, including the new ...
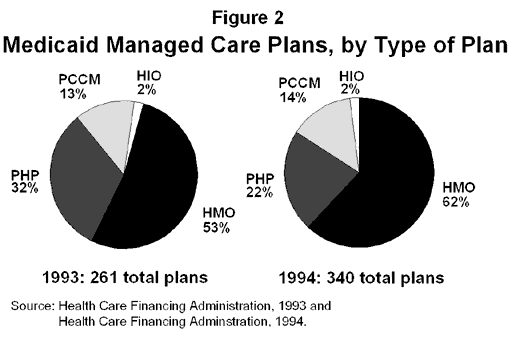
What is the difference between Medicare and Medicare managed care?
Medicare care managed care plans are an optional coverage choice for people with Medicare. Managed care plans take the place of your original Medicare coverage. Original Medicare is made up of Part A (hospital insurance) and Part B (medical insurance). Plans are offered by private companies overseen by Medicare.Sep 9, 2020
What is the difference between Medicare fee for service and Medicare managed care?
Under the FFS model, the state pays providers directly for each covered service received by a Medicaid beneficiary. Under managed care, the state pays a fee to a managed care plan for each person enrolled in the plan.
What is the difference between managed care and PPO?
There are three types of managed care plans: Health Maintenance Organizations (HMO) usually only pay for care within the network. You choose a primary care doctor who coordinates most of your care. Preferred Provider Organizations (PPO) usually pay more if you get care within the network.Sep 20, 2018
What is the purpose of managed care plans?
The purpose of managed care is to enhance the quality of healthcare for all patient populations. Managed care revolves around the collaboration of health insurance plans and healthcare providers. Managed Care includes healthcare plans that are used to manage cost, utilization, and quality.Dec 29, 2020
What are the three main payment mechanisms used in managed care?
What are the three main payment mechanisms managed care uses? In each mechanism who bears the risk. The three main types of payment arrangements with providers are: capitation, discounted fees, and salaries.
What are the 4 types of Medicare?
There are four parts of Medicare: Part A, Part B, Part C, and Part D.Part A provides inpatient/hospital coverage.Part B provides outpatient/medical coverage.Part C offers an alternate way to receive your Medicare benefits (see below for more information).Part D provides prescription drug coverage.
What is an example of a managed care plan?
A good example of a managed care plan is an HMO (Health Maintenance Organization). HMOs closely manage your care. Your cost is lowest with an HMO. You are limited to seeing providers in a small local network, which also helps keep costs low.
What are the benefits of managed care?
What Are the Advantages of Managed Care?It lowers the costs of health care for those who have access. ... People can seek out care from within their network. ... Information moves rapidly within a network. ... It keeps families together. ... There is a certain guarantee of care within the network.More items...•Jun 14, 2017
How does managed care manage costs?
Managed care organizations (MCOs) have the potential to control costs by changing provider incentives away from excessive utilization of resources toward less costly and more effective treatments.
Who Receives Managed Health Care Plan services?
Do I Qualify? Most people 65 and older. Some younger people with disabilities. People with End-Stage Renal Disease (kidney failure requiring dialysis or a transplant).
What is the most common form of managed care?
HMOThe most common type of managed care plan is the HMO. If you enroll in an HMO plan, you'll need to pick a primary care provider who will direct all your healthcare needs and refer you to specialists when appropriate. You are only covered if you go to medical providers and facilities who are in your network.
Which of the following is a disadvantage of managed care?
Benefits of managed care include patients having multiple options for coverage and paying lower costs for prescription drugs. Disadvantages include restrictions on where patients can get services and issues with finding referrals.Oct 20, 2018
What is Medicare managed care?
Medicare care managed care plans are an optional coverage choice for people with Medicare. Managed care plans take the place of your original Medicare coverage. Original Medicare is made up of Part A (hospital insurance) and Part B (medical insurance). Plans are offered by private companies overseen by Medicare.
How much does Medicare cost in 2021?
Most people receive Part A without paying a premium, but the standard Part B premium in 2021 is $148.50. The cost of your managed care plan will be on top of that $148.50.
Does Medicare cover dental care?
For example, original Medicare doesn’t cover routine dental care, but many managed care plans do. Managed care plans sometimes include coverage for Medicare Part D, which is prescription drug coverage. Managed care plans often include this coverage with your plan. This means all your coverage will be under one plan.
What is Medicare Advantage?
Sometimes referred to as Medicare Part C or Medicare Advantage, Medicare managed care plans are offered by private companies. These companies have a contract with Medicare and need to follow set rules and regulations. For example, plans must cover all the same services as original Medicare.
Do you have to be enrolled in Medicare Part A and Part B?
You’ll need to be enrolled in both Medicare Part A and Part B to be eligible for a managed care plan. You can become eligible for parts A and B in a few ways:
What is PFFS in medical?
Private Fee-for-Service (PFFS). A PFFS is a less common type of managed care plan. PFFS plans don’t have networks. Instead, for a present price, you can see any doctor who contracts with Medicare. However, not all providers accept PFFS plans. Special Needs Plan (SNP).
What is a Medigap plan?
A Medigap plan, also known as Medicare supplement insurance, is optional coverage you can add to original Medicare to help cover out-of-pocket costs. Medigap plans can help you pay for things like: coinsurance costs. copayments. deductibles. These aren’t a type of managed care plan.
What is Medicare managed care?
A Medicare managed care plan is a type of Medicare Advantage plan. Learn what managed care plans are and how they could be a good fit for you. A Medicare managed care plan is one type of Medicare Advantage plan. The term “managed care plan” generally refers to HMO (health maintenance organization), PPO (preferred provider organization) ...
What are the different types of Medicare plans?
Types of Medicare managed care plans 1 Health maintenance organization (HMO)#N#In a Medicare HMO plan, you use a primary care physician to coordinate your care, and you receive services from a network of health care providers that partner with your plan. 2 Preferred provider organization (PPO)#N#In a Medicare PPO plan, you may or may not use a primary care physician, and you are typically not required to get a referral to see a specialist. You’ll have a network of providers from which to choose .You will generally can receive at least some coverage when receiving care outside of the network of providers, though your health care services may cost more than if you received them from a provider within your plan network. 3 Point of service (POS)#N#You can use a primary care physician in a Point of Service plan, as you would with an HMO plan. But as with a PPO plan, you can go outside of the plan network and still receive some coverage for services, though you may pay higher out-of-pocket costs than if you selected an in-network provider.
How to contact Medicare Advantage?
For more information about managed care plans or other types of Medicare Advantage plans, including plan benefits, eligibility, enrollment and availability, contact a licensed insurance agent by calling. 1-800-557-6059. 1-800-557-6059 TTY Users: 711 24 hours a day, 7 days a week.
What is a HMO plan?
Health maintenance organization (HMO) In a Medicare HMO plan, you use a primary care physician to coordinate your care, and you receive services from a network of health care providers that partner with your plan. Preferred provider organization (PPO)
Why do you see a primary care physician?
Seeing a primary care physician allows patients to build a rapport with their doctor, and the doctor gets to know the patient’s health history firsthand . When a patient is referred to a specialist, there is communication between the primary care physician and the specialist regarding the patient’s health and treatment.
Who is Christian Worstell?
Christian Worstell is a licensed insurance agent and a Senior Staff Writer for MedicareAdvantage.com. He is passionate about helping people navigate the complexities of Medicare and understand their coverage options. .. Read full bio
What is Medicare Part B?
Medicare Part B covers individual and group therapy services to diagnose and treat mental illness. The Part B coverage usually requires a physician referral for mental health care and is based on a mental health diagnosis.
Does MA have a safety device?
MA plans may choose to offer, as a supplemental benefit, provision of specific non-Medicare-covered safety devices to prevent injuries in the bathroom. In addition to providing and installing appropriate safety devices, the benefit may include an in-home bathroom safety inspection conducted by a qualified health professional, in accordance with applicable state and Federal requirements, to identify the need for safety devices, as well as the applicability to the specific enrollee’s bathroom (e.g., to determine whether a specific safety device can be installed into the bathroom).
What is general nutrition education?
General nutritional education for all enrollees through classes and/or individual counseling may be provided as a supplemental benefit as long as the services are provided by practitioners who are practicing in the state in which s/he is licensed or certified, and are furnishing services within the scope of practice defined by their licensing or certifying state. (i.e., physician, nurse, registered dietician or nutritionist). The number of visits, time limitations, and whether the benefit is for classes and/or individual counseling must be defined in the PBP.
Who must provide acupuncture in MA?
The acupuncture provided by MA plans as a supplemental benefit must be provided by practitioners who are licensed or certified, as applicable, in the state in which they practice and are furnishing services within the scope of practice defined by their licensing or certifying state.
Does MA offer alternative therapies?
MA plans may offer alternative therapies as supplemental benefits. These alternative therapies must be provided by practitioners who are licensed or certified, as applicable, in the state in which they practice and are furnishing services within the scope of practice defined by their licensing or certifying state. MA plans are to provide a description of therapies offered in the PBP Notes section.
What is a non-SNP physical exam?
Non-SNP MA plans may offer as a supplemental benefit a physical exam that provides services beyond those services required to be provided in the Annual Wellness Visit. To be considered an Annual Physical Exam that qualifies as a supplemental benefit by CMS, the exam would be provided by a qualified physician or qualified non-physician practitioner, hereafter referred to as a practitioner. At a minimum, the exam would include a detailed medical/family history and the performance of a detailed head to toe assessment with hands-on examination of all the body systems. For example, the practitioner uses visual inspection, palpation, auscultation and 133 manual examination in his/her full examination to assess overall general health and detect abnormalities or signs that could indicate a disease process that should be addressed. We consider these components minimum elements and not an exhaustive list.
Does MA offer chiropractic care?
MA plans may choose to offer routine chiropractic services as a supplemental benefit as long as the services are provided by a state-licensed chiropractor practicing in the state in which he/she is licensed and is furnishing services within the scope of practice defined by that state’s licensure and practice guidelines. The routine services may include conservative management of neuromusculoskeletal disorders and related functional clinical conditions including, but not limited to, back pain, neck pain and headaches, and the provision of spinal and other therapeutic manipulation/adjustments.
How does managed care work?
The primary way in which managed care plans work is by establishing provider networks. A provider network serves plan members over a certain geographic area in which the health plan is available. The providers in these networks agree to offer their services at reduced costs. Your health plan pays more of the cost of your care if you see providers ...
What is managed care organization?
A managed care organization or MCO is a health care company or a health plan that is focused on managed care as a model to limit costs, while keeping quality of care high.
Why do doctors do regular check ups?
Regular check-ups help doctors identify health problems early, before they become major and costly. No-cost preventive care is a big incentive for plan members to try and maintain good health. Primary Care Providers (PCP): Your health plan may require you to choose a PCP if you don’t already have one.
What are some examples of managed care?
They are examples of managed care: Provider networks: Health insurance companies contract with groups of providers to offer plan members reduced rates on care and services. These networks can include doctors, specialists, hospitals, labs, and other health care facilities. Some health plans require you to use the plan’s provider network ...
Is a PPO more expensive than an HMO?
A PPO also costs a bit more than an HMO for that flexibility. Both types of plans are designed to help keep costs lower and quality high. Managed care is a type of health care model that is commonplace. Most common types of health plans have features of managed care that help keep costs in check and quality of care high.
What is a prior authorization?
Prior authorization: Most managed care plans require you to get approval before you have certain types of procedures or treatments done, or are prescribed certain types of specialty medications. This is called prior authorization, precertification, or preapproval, depending on your insurer. Part of managed care’s goal is to help ensure you are not ...
What is HMO insurance?
Health Maintenance Organization (HMO) manages care by requiring you to see network providers, usually for a much lower monthly premium. HMOs also often require you to see a PCP before going elsewhere, and do not cover you to see providers outside the network. Preventive care is covered at 100%.
Why is Medicaid important?
The Affordable Care Act allows for states to expand Medicaid to more low-income adults, which research shows has increased access to care and reduced mortality among this group. Additionally, states rely on Medicaid to cover treatment in disease outbreaks and crises, such as the Zika virus and the opioid epidemic.
What is comprehensive risk based managed care?
Comprehensive risk-based managed care#N#Of the three main types of Medicaid managed care, the most common is the comprehensive risk-based managed care provided through managed care organizations (MCOs). In 2017, 69 percent of Medicaid enrollees had this type of plan. In this model, states contract with MCOs to provide a full package of benefits to Medicaid enrollees. In turn, states typically pay the MCOs using a capitated payment system, or one where the MCO is paid a fixed monthly rate per enrollee to provide their healthcare services.
How many states have managed care?
Of the 38 states employing managed care, 17 had at least 90 percent of their Medicaid population in MCOs. Managed care organizations are risk-based, meaning they are under contract with states to pay for enrollees’ care even if the costs exceed the capitated rates at which they are reimbursed.
What is limited benefit plan?
Limited benefit plans are similar to MCOs in structure in that states typically contract with a plan and pay based on a capitated payment system. However, limited benefit plans only provide certain Medicaid services such as dental or behavioral health services instead of providing a full range of health services.
How many people are covered by CMS?
Centers for Medicare and Medicaid Services (CMS): Federal agency, in partnership with states, that covers over 100 million people through Medicare, Medicaid, Children’s Health Insurance Program (CHIP) and the Health Insurance Marketplace.
Is Medicaid a partnership?
Medicaid is structured as a partnership between the federal government and individual states and is therefore financed jointly by the two. The federal government reimburses states for the federal share of each state’s program costs and there is no cap or limit on the amount of federal funds a state can receive.
What percentage of federal spending is Medicaid?
Medicaid accounted for 9.5 percent of federal spending in FY2017 and is the third-largest domestic program in the budget, after Social Security and Medicare. It was also the second-largest item in state budgets in 2017.
