Medicaid
Medicaid in the United States is a federal and state program that helps with medical costs for some people with limited income and resources. Medicaid also offers benefits not normally covered by Medicare, including nursing home care and personal care services. The Health Insurance As…
Full Answer
How does Medicaid work with Medicare?
Feb 11, 2022 · While MSPs do not provide the same coverage, they do provide assistance paying for Medicare premiums. They may also cover Medicare deductibles and co-payments. Benefits of Dual Eligibility. Persons who are enrolled in both Medicaid and Medicare may receive greater healthcare coverage and have lower out-of-pocket costs. For Medicare covered expenses, such …
Is Medicare and Medicaid the same thing in every state?
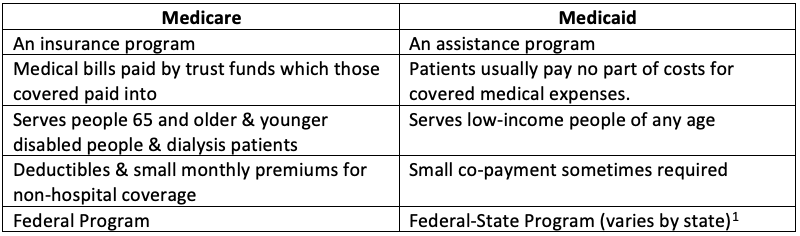
For more information regarding Medicare and its components, please go to http://www.medicare.gov. Medicaid. Medicaid is an assistance program. It serves low-income people of every age. Patients usually pay no part of costs for covered medical expenses. A small co-payment is sometimes required. Medicaid is a federal-state program.
What is the difference between Medicare and Medicaid eligibility?
Medicaid and Medicare. ... An official website of the United States government. The .gov means it’s official. Federal government websites always use a .gov or .mil domain. Before sharing sensitive information online, make sure you’re on a .gov or .mil site by inspecting your browser’s address (or “location”) bar. ...
Is it common for Medicare beneficiaries to receive Medicaid benefits?
As long as your income falls under the limits for Medicaid eligibility in your state, you will receive both types of coverage. More than 8 million people have both Medicare and Medicaid. In this situation, Medicare becomes your primary insurance and settles your medical bills first; and Medicaid become secondary, paying for services that Medicare doesn’t cover and also paying …
When the patient is covered by both Medicare and Medicaid what would be the order of reimbursement?
What is the difference in Medicare and Medicaid?
Do Medicare benefits differ by state?
What is the highest income to qualify for Medicaid?
The Federal Poverty Level is determined by the size of a family for the lower 48 states and the District of Columbia. For example, in 2022 it is $13,590 for a single adult person, $27,750 for a family of four and $46,630 for a family of eight.Mar 26, 2022
What are the disadvantages of Medicaid?
- Lower reimbursements and reduced revenue. Every medical practice needs to make a profit to stay in business, but medical practices that have a large Medicaid patient base tend to be less profitable. ...
- Administrative overhead. ...
- Extensive patient base. ...
- Medicaid can help get new practices established.
Can a person have Medicare and Medicaid at the same time?
How do you qualify to get 144 back from Medicare?
- Are enrolled in Part A and Part B.
- Do not rely on government or other assistance for your Part B premium.
- Live in the zip code service area of a plan that offers this program.
- Enroll in an MA plan that provides a giveback benefit.
Is Medicare covered in all states?
Who qualifies for Medicare premium refund?
How much money can you have in the bank on Medicaid?
How can I be eligible for Medicaid?
Does Medicare coverage start the month you turn 65?
Is Medicaid a federal or state program?
This is because, as mentioned previously, Medicaid is a federal and state program. While the parameters of the program are federally set, each state can set their own rules within these guidelines. Even within the same state, there are a variety of pathways to Medicaid that have their own eligibility requirements.
Does Medicaid cover nursing home care?
Medicaid also pays for nursing home care, and often limited personal care assistance in one’s home. While some states offer long-term care and supports in the home and community thorough their state Medicaid program, many states offer these supports via 1915 (c) Medicaid waivers.
What is Medicare dual eligible?
Persons who are eligible for both Medicare and Medicaid are called “dual eligibles”, or sometimes, Medicare-Medicaid enrollees. Since it can be easy to confuse the two terms, Medicare and Medicaid, it is important to differentiate between them. While Medicare is a federal health insurance program for seniors and disabled persons, Medicaid is a state and federal medical assistance program for financially needy persons of all ages. Both programs offer a variety of benefits, including physician visits and hospitalization, but only Medicaid provides long-term nursing home care. Particularly relevant for the purposes of this article, Medicaid also pays for long-term care and supports in home and community based settings, which may include one’s home, an adult foster care home, or an assisted living residence. That said, in 2019, Medicare Advantage plans (Medicare Part C) began offering some long-term home and community based benefits.
What is Medicare Part A and Part B?
To be considered dually eligible, persons must be enrolled in Medicare Part A, which is hospital insurance, and / or Medicare Part B, which is medical insurance. As an alternative to Original Medicare (Part A and Part B), persons may opt for Medicare Part C, which is also known as Medicare Advantage.
Does Medicare cover out-of-pocket expenses?
Persons who are enrolled in both Medicaid and Medicare may receive greater healthcare coverage and have lower out-of-pocket costs. For Medicare covered expenses, such as medical and hospitalization, Medicare is always the first payer (primary payer). If Medicare does not cover the full cost, Medicaid (the secondary payer) will cover the remaining cost, given they are Medicaid covered expenses. Medicaid does cover some expenses that Medicare does not, such as personal care assistance in the home and community and long-term skilled nursing home care (Medicare limits nursing home care to 100 days). The one exception, as mentioned above, is that some Medicare Advantage plans cover the cost of some long term care services and supports. Medicaid, via Medicare Savings Programs, also helps to cover the costs of Medicare premiums, deductibles, and co-payments.
Is Medicare the primary or secondary payer?
For Medicare covered expenses, such as medical and hospitalization, Medicare is always the first payer (primary payer). If Medicare does not cover the full cost, Medicaid (the secondary payer) will cover the remaining cost, given they are Medicaid covered expenses.
Does Medicare provide long term care?
Long-Term Care Benefits. Medicaid provides a wide variety of long-term care benefits and supports to allow persons to age at home or in their community. Medicare does not provide these benefits, but some Medicare Advantage began offering various long term home and community based services in 2019. Benefits for long term care may include ...
Is Medicare a federal program?
Small monthly premiums are required for non-hospital coverage. Medicare is a federal program. It is basically the same everywhere in the United States and is run by the Centers for Medicare & Medicaid Services, an agency of the federal government.
What is Medicare insurance?
Medicare. Medicare is an insurance program. Medical bills are paid from trust funds which those covered have paid into. It serves people over 65 primarily, whatever their income; and serves younger disabled people and dialysis patients. Patients pay part of costs through deductibles for hospital and other costs.
Does Medicaid require income?
Certain Medicaid eligibility groups do not require a determination of income by the Medicaid agency. This coverage may be based on enrollment in another program, such as SSI or the breast and cervical cancer treatment and prevention program.
What is Medicaid coverage?
Medicaid is the single largest source of health coverage in the United States. To participate in Medicaid, federal law requires states to cover certain groups of individuals. Low-income families, qualified pregnant women and children, and individuals receiving Supplemental Security Income (SSI) are examples of mandatory eligibility groups (PDF, ...
How many people are covered by medicaid?
Medicaid is a joint federal and state program that, together with the Children’s Health Insurance Program (CHIP), provides health coverage to over 72.5 million Americans, including children, pregnant women, parents, seniors, and individuals with disabilities. Medicaid is the single largest source of health coverage in the United States.
What is MAGI for Medicaid?
MAGI is the basis for determining Medicaid income eligibility for most children, pregnant women, parents, and adults. The MAGI-based methodology considers taxable income and tax filing relationships to determine financial eligibility for Medicaid. MAGI replaced the former process for calculating Medicaid eligibility, ...
What is dual eligible for Medicare?
Eligibility for the Medicare Savings Programs, through which Medicaid pays Medicare premiums, deductibles, and/or coinsurance costs for beneficiaries eligible for both programs (often referred to as dual eligibles) is determined using SSI methodologies..
Do you have to be a resident to get medicaid?
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
What is a fair hearing?
States must provide individuals the opportunity to request a fair hearing regarding a denial, an action taken by the state agency that he or she believes was erroneous, or if the state has not acted with reasonable promptness. States have options for how to structure their appeals processes.
What is Medicaid coverage?
Medicaid provides health coverage to millions of Americans, including children, pregnant women, parents, seniors and individuals with disabilities. In some states the program covers all low-income adults below a certain income level. Note: Medicaid...
What is California medicaid?
California Medicaid. Medi-Cal is California's Medicaid health care program. This program pays for a variety of medical services for children and adults with limited income and resources. Medi-Cal is supported by Federal and state taxes.
What is Medicaid in Alaska?
Medicaid is a health insurance program for specified low-income target groups in Alaska. Potential recipients include children, pregnant women, the aged, blind, and/or disabled, and people who are eligible to receive Federally assisted income...
What is Arkansas Medicaid?
Medicaid provides health coverage to millions of Americans, including children, pregnant women, parents, seniors and individuals with disabilities. In some states the program covers all low-income adults below a certain income level. Note: Medicaid... Medicaid and Medicare.
What is a medicaid program in California?
This program pays for a variety of medical services for children and adults with limited income and resources. Medi-Cal is supported by Federal and state taxes.
What is Medicaid in Connecticut?
Medicaid provides health coverage to millions of Americans, including children, pregnant women, parents, seniors and individuals with disabilities. In some states the program covers all low-income adults below a certain income level.
What is the health insurance marketplace?
The Health Insurance Marketplace helps you find health coverage that fits your needs and budget. Every health plan in the Marketplace offers the same set of essential health benefits, including doctor visits, preventive care, hospitalization,... Medicaid and Medicare. Children's Health.
How many people have Medicare and Medicaid?
As long as your income falls under the limits for Medicaid eligibility in your state, you will receive both types of coverage. More than 8 million people have both Medicare and Medicaid. In this situation, Medicare becomes your primary insurance and settles your medical bills first; and Medicaid become secondary, ...
Is Medicare a secondary insurance?
In this situation, Medicare becomes your primary insurance and settles your medical bills first; and Medicaid become secondary, paying for services that Medicare doesn’t cover and also paying most of your out-of-pocket expenses in Medicare (premiums, deductibles and copays).
Does Medicare cover medicaid?
If you qualify for a Medicaid program, it may help pay for costs and services that Medicare does not cover.
Does Medicaid cover cost sharing?
If you are enrolled in QMB, you do not pay Medicare cost-sharing, which includes deductibles, coinsurances, and copays.
Is Medicare the same as Medicaid?
The federal government oversees Medicare eligi bility – meaning it is the same in each state. But states set their own eligibility rules for Medicaid and the MSPs (within federal guidelines) – and income limits for these programs vary widely.
Do seniors qualify for medicaid?
Many seniors who live in nursing homes are dual eligible: they qualify for Medicare based on their age, and Medicaid because of their financial circumstances.
What is dual eligible Medicare?
Beneficiaries with Medicare and Medicaid are known as dual eligibles – and account for about 20 percent of Medicare beneficiaries (12.1 million people). Dual eligibles are categorized based on whether they receive partial or full Medicaid benefits. Full-benefit dual eligibles have comprehensive Medicaid coverage, ...
What percentage of Medicare beneficiaries are dual eligible?
Beneficiaries with Medicare and Medicaid are known as dual eligibles – and account for about 20 percent of Medicare beneficiaries (12.1 million people). Dual eligibles are categorized based on whether they receive partial or full Medicaid benefits.
Does Medicare cover long term care?
But this is not the case for things Medicare doesn’t cover, like long-term care . If Medicaid is covering a beneficiary’s long-term care, Medicare will still be the primary payer for any Medicare-covered services – like skilled nursing care or physical therapy.
What is a dual eligible special needs plan?
If you are dual eligible, you are can enroll in a dual eligible special needs plan (D-SNP) that covers both Medicare and Medicaid benefits. These plans may also pay for expenses that Medicare and Medicaid don’t over individually, including over-the-counter items, hearing aids, and vision or dental care. Beneficiaries who are dual eligible can ...
Who is Josh Schultz?
Josh Schultz has a strong background in Medicare and the Affordable Care Act. He coordinated a Medicare ombudsman contract at the Medicare Rights Center in New York City, and represented clients in extensive Medicare claims and appeals.
When will Medicare be updated?
On September 8, 2020, the Centers for Medicare & Medicaid Services (CMS) released an updated version of the Manual for State Payment of Medicare Premiums (formerly called “State Buy-in Manual”). The manual updates information and instructions to states on federal policy, operations, and systems concerning the payment of Medicare Parts A ...
When was the Medicare buy in manual released?
Manual for State Payment of Medicare Premiums (formerly called “State Buy-in Manual”) On September 8, 2020, the Centers for Medicare & Medicaid Services (CMS) released an updated version of the Manual for State Payment of Medicare Premiums (formerly called “State Buy-in Manual”). The manual updates information and instructions to states on federal ...
How many people pay Medicare Part B?
States pay Medicare Part B premiums each month for over 10 million individuals and Part A premium for over 700,000 individuals.
Is United American a Medicare Supplement?
United American has been a prominent Medicare Supplement insurance provider since Medicare began in 1966. Additionally, we’ve been a long-standing participant in the task forces working on Medicare Supplement insurance policy recommendations for the National Association of Insurance Commissioners.
Does Medicare Supplement Insurance cover deductibles?
The purpose of Medicare Supplement Insurance is to cover the cost left by deductibles and coinsurance in Original Medicare, but as full Medicaid coverage should cover the majority of those costs, a Medicare Supplement Insurance policy isn’t necessary. 3.
Is United American Insurance endorsed by the government?
The purpose of this communication is the solicitation of insurance. United American Insurance Company is not connected with, endorsed by, or sponsored by the U.S. government, federal Medicare program, Social Security Administration, or the Department of Health and Human Services. Policies and benefits may vary by state and have some limitations and exclusions. Individual Medicare Supplement insurance policy forms MSA10, MSB10, MSC10, MSD10, MSF10, MSHDF10, MSG10, MSHDG, MSK06R, MSL06R, MSN10 and in WI, MC4810 and MC4810HD, MC4810HDG are available from our Company where state-approved. Some states require these plans be available to persons under age 65 eligible for Medicare due to disability or End Stage Renal disease (ESRD). You may be contacted by an agent or producer representing United American Insurance Company, PO Box 8080, McKinney, TX 75070-8080. OUTLINE OF COVERAGE PROVIDED UPON REQUEST.
Determining Eligibility For Medicaid
- Financial Eligibility
The Affordable Care Act established a new methodology for determining income eligibility for Medicaid, which is based on Modified Adjusted Gross Income (MAGI). MAGI is used to determine financial eligibility for Medicaid, CHIP, and premium tax credits and cost sharing reductions avail… - Non-Financial Eligibility
To be eligible for Medicaid, individuals must also meet certain non-financial eligibility criteria. Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, suc…
Medically Needy
- States have the option to establish a “medically needy program” for individuals with significant health needs whose income is too high to otherwise qualify for Medicaid under other eligibility groups. Medically needy individuals can still become eligible by “spending down” the amount of income that is above a state's medically needy income standard. Individuals spend down by incu…
Appeals
- States must provide individuals the opportunity to request a fair hearing regarding a denial, an action taken by the state agency that he or she believes was erroneous, or if the state has not acted with reasonable promptness. States have options for how to structure their appeals processes. Appeals may be conducted by the Medicaid agency or delegated to the Exchange or …
Related Topics
- Spousal Impoverishment: Protects the spouse of a Medicaid applicant or beneficiary who needs coverage for long-term services and supports (LTSS), in either an institution or a home or other community-based setting, from becoming impoverished in order for the spouse in need of LTSS to attain Medicaid coverage for such services. Treatment of Trusts: When an individual, his or her s…