What is the maximum income taxed for Medicare?
- When it comes to receiving Medicare benefits, there are no income restrictions.
- You may be asked to pay more money for a premium depending on your income.
- If you have a minimal income, you may be eligible for Medicare premium assistance.
What income is subject to Medicare tax?
Typically, self-employment tax is required if you earned over $400 per year from self-employment. Taxes on self-employment usually require an amount of 92 dollars. Self-employment earnings are subject to a 35% tax. Even if you are receiving social security benefits, you will still be responsible for paying self-employment tax.
What is the lifetime cap on Medicare?
Skilled Nursing Facilities
- Up to 20 days: Medicare pays the full cost
- From day 21-100: you pay a share of the cost ($185.50 coinsurance per day of each benefit period in 2021)
- Beyond 100 days: you pay all costs.
What is the monthly income limit for Medicaid?
What are the income guidelines for Medicaid? Income requirements: For Medicaid coverage a single adult is capped $1,468 per month and families of four can make $3,013 per month. Single aged or disabled adults over 65 have an income cap of $836 and $1,195 for couples.
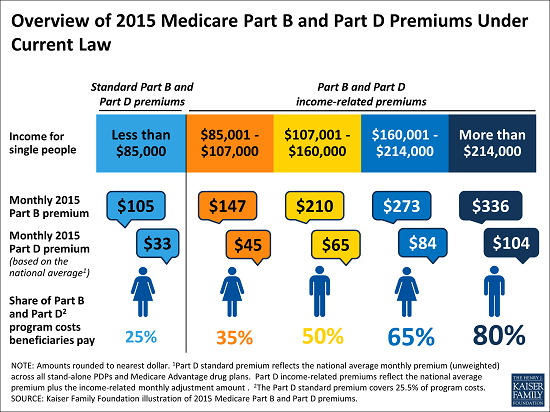
What is the Medicare earnings limit for 2020?
How much will I pay for premiums in 2022?Yearly income in 2020: singleYearly income in 2020: married, joint filing2022 Medicare Part B monthly premium≤ $91,000≤ $182,000$170.10> $91,00–$114,000> $182,000–$228,000$238.10> $114,000–$142,000> $228,000–$284,000$340.20> $142,000–$170,000> $284,000–$340,000$442.302 more rows•Nov 16, 2021
What is the Medicare earnings limit for 2021?
In 2021, the adjustments will kick in for individuals with modified adjusted gross income above $88,000; for married couples who file a joint tax return, that amount is $176,000. For Part D prescription drug coverage, the additional amounts range from $12.30 to $77.10 with the same income thresholds applied.
How much money can you make before your Medicare goes up?
If your MAGI for 2020 was less than or equal to the “higher-income” threshold — $91,000 for an individual taxpayer, $182,000 for a married couple filing jointly — you pay the “standard” Medicare Part B rate for 2022, which is $170.10 a month.
Do 401k withdrawals count as income for Medicare?
The distributions taken from a retirement account such as a traditional IRA, 401(k), 403(b) or 457 Plan are treated as taxable income if the contribution was made with pre-tax dollars, Mott said.
At what age is Social Security no longer taxed?
However once you are at full retirement age (between 65 and 67 years old, depending on your year of birth) your Social Security payments can no longer be withheld if, when combined with your other forms of income, they exceed the maximum threshold.
What are the two Medicare programs that require higher monthly premiums?
Those with higher incomes must pay higher monthly premiums for two Medicare programs. These include Part B , which is the outpatient medical coverage of original Medicare, and Part D , the program that provides prescription drug coverage. This article discusses the parts of Medicare that higher premiums may, or may not, affect.
How does Medicare determine premiums?
To determine the premiums it assigns, Medicare uses someone’s federal tax return from the Internal Revenue Service (IRS). In figuring the premiums of beneficiaries for 2021, Medicare uses tax returns from 2019, which is the most recent year the IRS provides to Social Security. Most of the income thresholds for premium adjustments are subject ...
What is Medicare supplement insurance?
This plan combines the benefits of original Medicare parts A and B into one policy. Medigap, which is Medicare supplement insurance. This plan is available for purchase to a person with original Medicare. Private insurance companies administer both Medicare Advantage and Medigap plans.
How to appeal Medicare premium adjustment?
If an individual does not agree with Medicare’s decision about their income-related premium adjustment, they can file an appeal. To do this, a person may call Social Security at 800-772-1213. A deaf or partially deaf person may call 877-486-2048.
What is the standard rate for Medicare 2021?
The majority of people fall into the income range associated with the standard rate, which in 2021 is $148.50. This amount can change each year.
Does Medicare have to adjust premiums based on income?
Medicare bases the adjustments on a person’s modified adjusted gross income, which is the total of adjusted gross income and tax-exempt interest income.
Can income be high for Medicare?
A person’s income cannot be so high that it disqualifies them for Medicare. Even those who receive very high incomes may enroll. However, individuals with higher incomes pay higher premiums for parts B and D, but Medicare income limits that affect premium rates only affect a small percentage of people.
What is the Medicare Advantage spending limit?
Medicare Advantage (Medicare Part C) plans, however, do feature an annual out-of-pocket spending limit for covered Medicare expenses. While each Medicare Advantage plan carrier is free to set their own out-of-pocket spending limit, by law it must be no greater than $7,550 in 2021. Some plans may set lower maximum out-of-pocket (MOOP) limits.
How many reserve days do you get with Medicare?
Medicare limits you to only 60 of these days to use over the course of your lifetime, and they require a coinsurance payment of $742 per day in 2021. You only get 60 lifetime reserve days, and they do not reset after a benefit period or a calendar year.
What is the Medicare donut hole?
Medicare Part D prescription drug plans feature a temporary coverage gap, or “ donut hole .”. During the Part D donut hole, your drug plan limits how much it will pay for your prescription drug costs. Once you and your plan combine to spend $4,130 on covered drugs in 2021, you will enter the donut hole. Once you enter the donut hole in 2021, you ...
How much is Medicare Part A deductible in 2021?
You are responsible for paying your Part A deductible, however. In 2021, the Medicare Part A deductible is $1,484 per benefit period. During days 61-90, you must pay a $371 per day coinsurance cost (in 2021) after you meet your Part A deductible.
What happens if you spend $6,550 out of pocket in 2021?
After you spend $6,550 out-of-pocket on covered drugs in 2021, you leave the donut hole coverage gap and enter the catastrophic coverage stage. Once you reach this stage, you only pay a small coinsurance or copayment for your covered drugs for the rest of the year.
What is Medicare Part B and Part D?
Medicare Part B (medical insurance) and Part D have income limits that can affect how much you pay for your monthly Part B and/or Part D premium. Higher income earners pay an additional amount, called an IRMAA, or the Income-Related Monthly Adjusted Amount.
What is Medicare Advantage Plan?
When you enroll in a Medicare Advantage plan, it replaces your Original Medicare coverage and offers the same benefits that you get from Medicare Part A and Part B.
How many credits can you earn on Medicare?
Workers are able to earn up to four credits per year. Earning 40 credits qualifies Medicare recipients for Part A with a zero premium.
How does Medicare affect late enrollment?
If you do owe a premium for Part A but delay purchasing the insurance beyond your eligibility date, Medicare can charge up to 10% more for every 12-month cycle you could have been enrolled in Part A had you signed up. This higher premium is imposed for twice the number of years that you failed to register. Part B late enrollment has an even greater impact. The 10% increase for every 12-month period is the same, but the duration in most cases is for as long as you are enrolled in Part B.
What is the premium for Part B?
Part B premium based on annual income. The Part B premium, on the other hand, is based on income. In 2020, the monthly premium starts at $144.60, referred to as the standard premium.
What is Medicare's look back period?
How Medicare defines income. There is a two-year look-back period, meaning that the income range referenced is based on the IRS tax return filed two years ago. In other words, what you pay in 2020 is based on what your yearly income was in 2018. The income that Medicare uses to establish your premium is modified adjusted gross income (MAGI).
4 kinds of Medicare Savings Programs
Select a program name below for details about each Medicare Savings Program. If you have income from working, you still may qualify for these 4 programs even if your income is higher than the income limits listed for each program.
How do I apply for Medicare Savings Programs?
If you answer yes to these 3 questions, call your State Medicaid Program to see if you qualify for a Medicare Savings Program in your state:.
What is Medicare premium based on?
Medicare premiums are based on your modified adjusted gross income, or MAGI. That’s your total adjusted gross income plus tax-exempt interest, as gleaned from the most recent tax data Social Security has from the IRS. To set your Medicare cost for 2021, Social Security likely relied on the tax return you filed in 2020 that details your 2019 ...
What is a hold harmless on Medicare?
If you pay a higher premium, you are not covered by “hold harmless,” the rule that prevents most Social Security recipients from seeing their benefit payment go down if Medicare rates go up. “Hold harmless” only applies to people who pay the standard Part B premium and have it deducted from their Social Security benefit.
What is the Medicare Part B rate for 2021?
If your MAGI for 2019 was less than or equal to the “higher-income” threshold — $88,000 for an individual taxpayer, $176,000 for a married couple filing jointly — you pay the “standard” Medicare Part B rate for 2021, which is $148.50 a month.
Can you ask Social Security to adjust your premium?
You can ask Social Security to adjust your premium if a “life-changing event” caused significant income reduction or financial disruption in the intervening tax year — for example, if your marital status changed , or you lost a job , pension or income-producing property. You’ll find detailed information on the Social Security web page “Medicare ...
Do you pay Medicare Part B if you are a high income beneficiary?
If you are what Social Security considers a “higher-income beneficiary,” you pay more for Medicare Part B, the health-insurance portion of Medicare. (Most enrollees don’t pay for Medicare Part A, which covers hospitalization.) Medicare premiums are based on your modified adjusted gross income, or MAGI. That’s your total adjusted gross income ...
What is the income limit for Medicare Part A?
The income limits are higher (up to $4,339/month for an individual, and $5,833 for a couple in 2020), but the asset limit is lower, at $4,000 for an individual and $6,000 for a couple.
What is extra help for Medicare?
Medicare offers “ Extra Help ” for Medicare enrollees who can’t afford their Part D prescription drug coverage. In 2020, if you’re a single person earning less than $1,615 per month ($2,175 for a couple), with financial resources that don’t exceed $14,610 ($29,160 for a couple), you may be eligible for “Extra Help.”.
How much can a single person earn in 2020?
A single person can qualify in 2020 with an income up to $1,296 per month ($1,744/month for a couple). Qualified Individual Program (QI). Helps to pay premiums for Part B. A single person can qualify in 2020 with an income up to $1,456 per month ($1,960/month for a couple). Qualified Disabled and Working Individuals Program (QDWI).
Does Medicare cover long term care?
Medicare does not cover custodial long-term care, but Medicaid does, if the person has a low income and few assets. Almost two-thirds of the people living in American nursing homes are covered by Medicaid (almost all of them are also covered by Medicare).
Is Medicare a dual program?
Medicare-Medicaid dual eligibility. People who are eligible for MSPs are covered by Medicare, but receive assistance with premiums (and in some cases, cost-sharing) from the Medicaid program. But some low-income Medicare enrollees are eligible for full Medicaid benefits, in addition to Medicare. About 20 percent of Medicare beneficiaries are dually ...
