If the diagnosis provided is not one that Medicare accepts as justification for the test, they won’t pay for it. Apparently, the diagnosis provided on the order for your particular test is not one that Medicare accepts.
Full Answer
Will Medicare pay for an A1c test sooner than 90 days?
Medicare will not pay for an A1c sooner than 90 days from the last one. Was one done less than 90 days before this one? Join or Login to remove this ad. T2 as of June 2009 but probably way before. Would talking to the doctor's office (admins) solve the problem? He hasn't been dxed with diabetes nor prediabetes.
Why won’t Medicare pay for a blood test?
If the diagnosis provided is not one that Medicare accepts as justification for the test, they won’t pay for it. Apparently, the diagnosis provided on the order for your particular test is not one that Medicare accepts.
Does Medicare cover HbA1c tests?
Medicare did not cover A1c, howver, deeming it "medically not necessary." If Medicare rejects the blood order claim, then apparently his AARP supplemental also doesn't kick in. Is this correct? You have to be a diabetic to have HbA1c test covered by Medicare Part B? Diagnostic testing is not covered?
How much does it cost to get an A1c test?
The A1c test, which doctors typically order every 90 days, is covered only once every three months. If more frequent tests are ordered, the beneficiary needs to know his or her obligation to pay the bill, in this case $66 per test.

Does Medicare pay for an A1C test?
Hemoglobin A1c Tests: Your doctor might order a hemoglobin A1c lab test. This test measures how well your blood glucose has been controlled over the past 3 months. Medicare may cover this test for anyone with diabetes if it is ordered by his or her doctor.
How often will Medicare cover A1C blood test?
The form, called an "Advance Beneficiary Notice of Noncoverage," or ABN, is a Medicare template intended to warn patients that Medicare imposes limits on coverage. The A1c test, which doctors typically order every 90 days, is covered only once every three months.
What diagnosis code covers A1C for Medicare?
Medicare recommends and provides coverage for diabetes screening tests through Part B Preventive Services for beneficiaries at risk for diabetes or those diagnosed with prediabetes....Table 1: HCPCS/CPT Codes and Descriptors.HCPCS/CPT CodesCode Descriptors83036Hemoglobin A1C3 more rows
Does Medicare cover diabetes testing?
If you qualify, Original Medicare covers diabetes screenings at 100% of the Medicare-approved amount when you receive the service from a participating provider. This means you pay nothing (no deductible or coinsurance).
What blood tests are not covered by Medicare?
Medicare does not cover the costs of some tests done for cosmetic surgery, insurance testing, and several genetic tests. There are also limits on the number of times you can receive a Medicare rebate for some tests. Your private health insurance may pay for diagnostic tests done while you are a patient in hospital.
What are the new guidelines for A1C?
ADA now recommends A1C below 7% or TIR above 70%, and time below range lower than 4% for most adults. In previous years, the Standards of Care included an “A1C Testing” subsection that recommended people with diabetes test their A1C two to four times a year with an A1C target below 7%.
What ICD 10 code covers hemoglobin A1C screening?
1.
How do I bill 83036 to Medicare?
Tests must be billed directly to Medicare by the laboratory or physician performing the test. If an outside laboratory performs a test on a referral from a physician, only the reference laboratory may legally bill Medicare for the procedure. The DOS is the date the specimen was collected.
What is the ICD 10 code for elevated hemoglobin A1C?
ICD-10-CM Diagnosis Code R97 R97.
What brand of glucose meter does Medicare 2020 cover?
This just in: Medicare will now cover Abbott's FreeStyle Libre real-time continuous glucose monitoring (CGM) system.
Does Medicare cover test strips for prediabetes?
Note: Medicare won't pay for any supplies not asked for, or for any supplies that were sent to a beneficiary automatically from suppliers. This includes blood glucose monitors, test strips, and lancets. Also, if a beneficiary goes to a pharmacy or supplier that is not enrolled in Medicare, Medicare will not pay.
What brand of glucose meter does Medicare 2022 cover?
Beginning Feb. 28, 2022, those using a Medtronic CGM integrated with the company's MiniMed insulin pumps will be able to get Medicare coverage for their transmitters, sensors and supplies.
What brand of glucose meter does Medicare 2020 cover?
Abbott's FreeStyle LibreThis just in: Medicare will now cover Abbott's FreeStyle Libre real-time continuous glucose monitoring (CGM) system.
Does Medicare cover 83036?
(2) the service must be medically necessary or indicated. Once these two criteria are met, Medicare pays for most clinical laboratory tests based on the Laboratory Fee Schedule.
How To Get Diabetes Supplies Through Medicare Part B
To get your diabetes supplies under Medicare Part B, you need a prescription from your doctor. The prescription should state:
Medicare Advantage Plans Cover Blood Tests
Learn more about how Medicare Advantage plans can cover your blood tests and may also offer additional benefits that aren’t covered by Original Medicare.
What Is An A1c Test
The hemoglobin A1c test tells you your average level of blood sugar over the past 2 to 3 months. Itâs also called HbA1c, glycated hemoglobin test, and glycohemoglobin. Itâs a lot like a baseball playerâs season batting average. A single game doesnât tell you how a player is performing in their career.
Artificial Pancreas Or Bi
An artificial pancreas is a closed-loop system with an insulin pump, real-time continuous glucose monitor and a small computing device to coordinate glucose sensing and insulin administration.
How Does The Ministry Know How Many Test Strips I Am Eligible For
Through your pharmacy, the Ministry of Health and Long-Term Cares Health Network System will track and automatically determine the number of blood glucose test strips that you are eligible to receive in a 365-day period. This is based on how you manage your diabetes, which is determined based on your prescription records for the past six months.
Glutamic Acid Decarboxylase Autoantibodies
Aetna considers measurement of autoantibodies to GAD medically necessary for distinguishing type 1 from type 2 diabetes when the clinical history is ambiguous and the results of testing will influence patient management. Measurement of anti-GAD antibodies is also considered medically necessary in diagnosing stiff-person syndrome.
Verify: Does Medicare Only Cover One Diabetic Test Strip A Day For Non
Viewer Betty Fischer said she took her doctors prescription to get four diabetic test strips a day to a CVS Pharmacy in White Plains, Maryland.
What is non coverage notice?
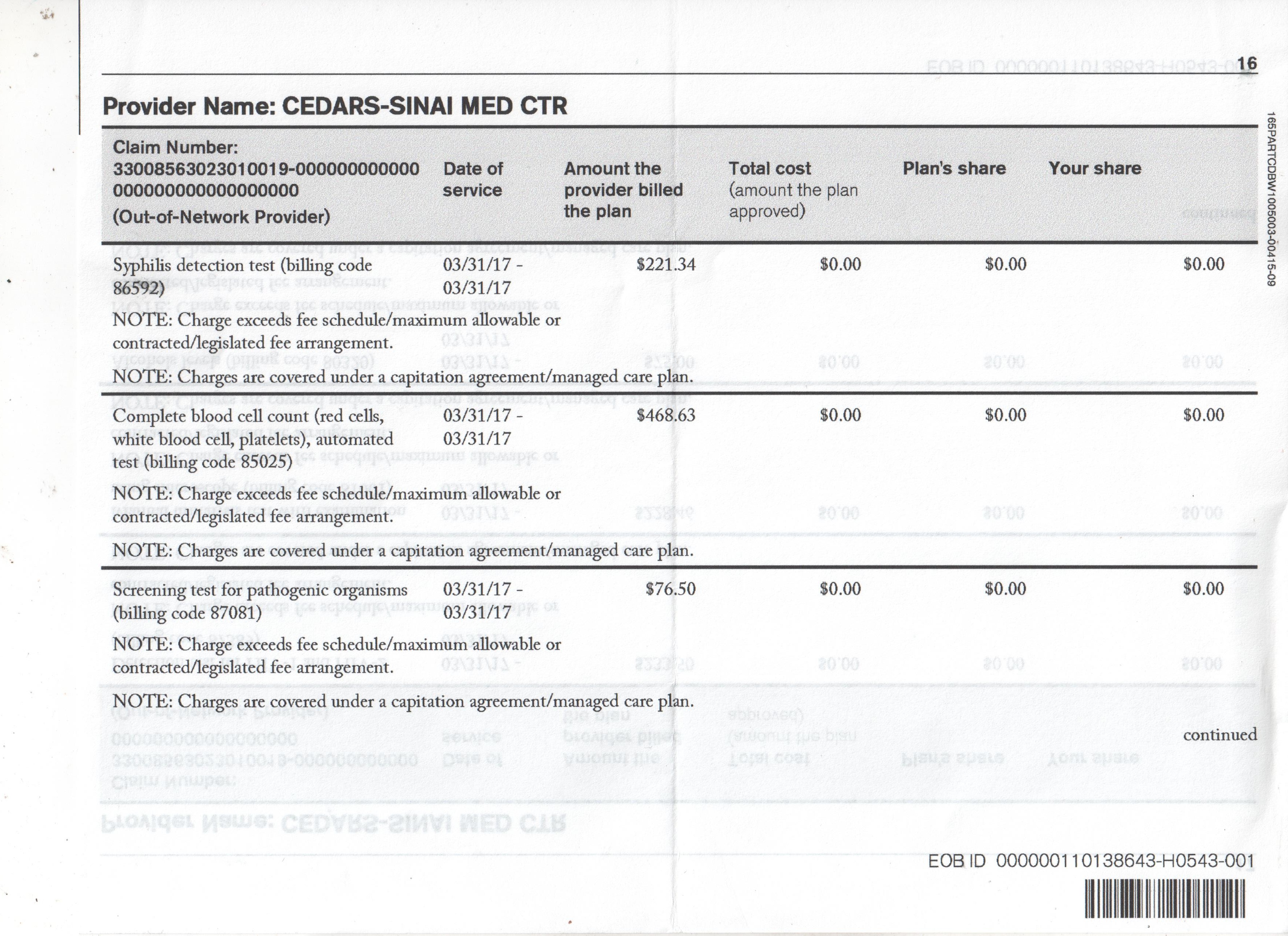
Lab's Non-Coverage Notice Deters Medicare Patients The national blood testing lab Quest Diagnostics has been handing thousands of Southern California Medicare patients with diabetes a "non-coverage" notice that physicians say is provoking patients to reject their essential A1c tests, which federal officials say violates Medicare rules . "This is a terribly ill-conceived administrative move that was done without consideration of the tremendously negative impact it is having on patient care," says Paul Speckart, MD, a San Diego endocrinologist. When patients in the practice he shares with four other doctors receive this form, "about one-third are canceling the test." The form, called an "Advance Beneficiary Notice of Noncoverage," or ABN, is a Medicare template intended to warn patients that Medicare imposes limits on coverage. The A1c test, which doctors typically order every 90 days, is covered only once every three months. If more frequent tests are ordered, the beneficiary needs to know his or her obligation to pay the bill, in this case $66 per test. If providers do not give patients these ABN forms to sign and the claims are denied, the provider is not entitled to collect directly from the patient. Continue reading >>
What does Medicare cover?
Medicare supports your self-care efforts by providing coverage for diabetes supplies and services. Medicare Part B covers testing and other supplies you may need plus some medical and education services. Medicare Part D covers diabetes medications and supplies for injecting or inhaling insulin.
How often does Medicare cover foot examinations?
Foot examination. Medicare Part B covers one foot examination every six months by a physician, podiatrist, or other licensed provider for someone who's been diagnosed with diabetic peripheral neuropathy resulting in loss of protective sensation. Hemoglobin A1c tests.
What is a glycosylated hemoglobin test?
Gly cated hemoglobin/protein levels are used to assess long-term glucose control in diabetes. Alternative names for these tests include glycated or glycosylated hemoglobin or Hgb, hemoglobin glycated or glycosylated protein, and fructosamine.
How often is the A1C test covered by Medicare?
The A1c test, which doctors typically order every 90 days, is covered only once every three months.
How many screenings does Medicare Part B cover?
When your doctor orders a screening test for you, Part B will cover up to two screenings per year. These screenings are covered 100% by Part B. Medicare Part B can also provide screenings for dyslipidemia, impaired glucose tolerance, high fasting glucose, and the very common hemoglobi Continue reading >>.
How much Medicare does a diabetic have to pay?
In general, you pay 20% of the Medicare-approved amount for diabetes supplies and services covered by Part B after the yearly deductible is met. Your percentage share of the cost is called coinsurance. You may pay a coinsurance amount or a copayment for items covered by Part D.
When will Medicare start paying for insulin?
Insulin savings through the Part D Senior Savings Model. Starting January 1, 2021, you may be able to get Medicare drug coverage that offers broad access to many types of insulin for no more than $35 for a month's supply.
What is original Medicare?
Your costs in Original Medicare. An agreement by your doctor, provider, or supplier to be paid directly by Medicare, to accept the payment amount Medicare approves for the service, and not to bill you for any more than the Medicare deductible and coinsurance. .
What is a Part B test?
Diabetes screenings. Part B covers certain doctors' services, outpatient care, medical supplies, and preventive services. covers glucose laboratory test screenings (with or without a carbohydrate challenge) if your doctor determines you’re at risk for developing diabetes. You may be eligible for up to 2 screenings each year.
Does Medicare cover blood sugar screening?
A history of high blood sugar (glucose) Medicare also covers these screenings if 2 or more of these apply to you: You’re age 65 or older. You’re overweight. You have a family history of diabetes (parents or siblings).
What to do if Medicare denied lab test?
These are but a few of the possibilities. If the lab bills you for the test because Medicare denied their request for payment, you should speak to your doctor. If an error was made, the doctor can notify the lab and give them a corrected diagnosis. The lab can then rebill Medicare for the test.
What is it called when a doctor orders a blood test?
When a doctor orders a blood test, they provide the lab with the justification for ordering the test. This is called the diagnosis . Many blood tests have limited coverage; that is, a test will be covered only for certain diagnoses. If the diagnosis provided is not one that Medicare accepts as justification for the test, they won’t pay for it.
What is shine in Florida?
SHINE is an award-winning statewide volunteer program that provides free, unbiased, and confidential counseling and information for people on Medicare, their families and caregivers. SHINE is a program of the Florida Department of Elder Affairs and is administered in partnership with the state’s 11 Aging and Disability Resource Centers (ADRCs). In Brevard County, our ADRC is the Senior Resource Alliance, located in Orlando.
How to contact a shine counselor?
To contact a SHINE volunteer counselor for confidential and unbiased assistance , call the Elder Helpline toll-free at 1-800-963-5337, or call 321-752-8080 locally. SHINE has counseling locations throughout Brevard County. Counselors can assist you by telephone or in person.
Where to write to Lance Jarvis?
If you have a question you would like the "Ask Lance" column to answer, write to Lance Jarvis at Senior Life, 7630 N. Wickham Road, Suite 105, Viera, FL 32940. You may also contact Jarvis by email at [email protected] or by telephone at 321-242-1235.
How often does Medicare cover fecal occult blood test?
Fecal occult blood test. Medicare covers a fecal occult blood test once every 12 months for people aged 50 years or above. The test checks for blood in the stool that a person cannot see with the naked eye. If the result is positive, it may indicate that some part of the digestive tract is bleeding.
How often does Medicare cover a Pap?
Pap test. Medicare generally covers Pap tests every 2 years for females , though some situations may require more frequent tests. For example, if a person had an abnormal Pap test in the previous 3 years and is of child-bearing age or at high risk of certain cancers, Medicare covers a Pap test once per year.
What is Medicare Advantage?
Medicare Advantage, or Medicare Part C, offers an alternative to Medicare parts A, B, and D. Medicare Advantage consists of Medicare-approved, private insurance companies that must follow the guidelines and rules of Medicare. Like parts A and B, Medicare Advantage plans cover the costs of blood work and other tests.
What is a coinsurance for Medicare?
Coinsurance: This is a percentage of a treatment cost that a person will need to self-fund. For Medicare Part B, this comes to 20%. Copayment: This is a fixed dollar amount that an insured person pays when receiving certain treatments. For Medicare, this usually applies to prescription drugs.
What is a complete blood count?
A complete blood count helps detect clotting problems, immune system disorders, blood cancers, and blood disorders such as anemia. It measures: red blood cells, which transport oxygen to all parts of the body. white blood cells, which fight infections. platelets, which are the fragments that enable the blood to clot.
Does Medicare cover blood work?
In some cases, Medicare Part A will cover the costs of blood work. Typically, a hospital or care facility will bill Part A when the person is staying within the facility. Medicare consists of three main parts: Part A: This is hospitalization insurance, which covers blood tests and other diagnostic laboratory tests that a doctor orders ...
Does Medicare pay for labs?
If a person with original Medicare goes to a Medicare-approved lab, they typically pay nothing for most diagnostic lab tests. However, there are exceptions when a person may need to pay part or all of the cost, such as when a doctor orders a lab test more often than Medicare coverage allows, or when a doctor orders a lab test that Medicare does not cover.
What is the purpose of blood test?
Blood tests are an important diagnostic tool doctors use to screen for risk factors and monitor health conditions. A blood test is generally a simple procedure to measure how your body is functioning and find any early warning signs. Medicare covers many types of blood tests. Trusted Source.
What is Medicare Part A?
Medicare Part A offers coverage for medically necessary blood tests. Tests can be ordered by a physician for inpatient hospital, skilled nursing, hospice, home health, and other related covered services. Medicare Part B covers outpatient blood tests ordered by a physician with a medically necessary diagnosis based on Medicare coverage guidelines.
How much is Medicare Part B 2021?
You have to meet your annual deductible for this coverage as well. In 2021, the deductible is $203 for most people. Remember, you also have to pay your monthly Part B premium, which is $148.50 in 2021 for most beneficiaries.
How often does Medicare cover mammograms?
once a year if you meet criteria. *Medicare covers diagnostic mammograms more often if your doctor orders them. You are responsible for the 20 percent coinsurance cost. Other nonlaboratory diagnostic screenings Medicare covers include X-rays, PET scans, MRI, EKG, and CT scans.
Does Medicare cover blood tests?
Medicare covers many types of common blood tests needed to diagnose and manage health conditions as long as they are medically necessary. Here are a few final tips to consider:
Does Medicare cover 20 percent coinsurance?
You have to pay your 20 percent coinsurance as well as your deductible and any copays. Remember to go to providers that accept assignment to avoid charges Medicare won’t cover. Helpful links and tools. Medicare offers a tool you can use to check which tests are covered.
Does Medicare cover ABN?
Medicare offers a tool you can use to check which tests are covered. You can also go here to look through the list of covered tests from Medicare. You can look through lists of codes and items Medicare does not cover. Before signing an ABN, ask about the cost of the test and shop around.
